Reduce Shoulder Tension with Somatic Practices and Electromyography*
Posted: November 20, 2022 Filed under: Uncategorized Leave a commentAdapted from Peper, E. & Booiman, A. (2022). Teaching awareness of shoulder tension with somatic practices and EMG. Biofeedback, 50(3), 80-85 https://doi.org/10.5298/1081-5937-50.03.02
I was totally surprised when I felt with my fingers my deltoid tightening, yet I was totally unaware that this muscles had tightened. No wonder that I am stiff and tight in my neck and shoulders at the end of the day. Now I interrupt my sitting and working with many movement and relaxation breaks and feel so much better at the end of the day. –Participant in training workshop
So many of us experience head, neck, shoulder and back problems as we do less physical movement and more static activities such as working at the computer, attending zoom meeting, driving in traffic, or communicating on their cellphone (David et al., 2021; Kumari, et al., 2021; Al-Hadidi et al., 2019). One contributing factor is that when we sit and work especially at the computer, we maintain covert low-level muscle tension. This unaware tension prevents regeneration and results in discomfort and pain at the end of the day (Kett et al., 2021; Sella, 2020; Whatmore & Kohli, 1968). This tension pattern can be reduced through somatic practices of small movement and muscle feedback with electromyography (EMG) so that the person may develop awareness of their covert tensions (Feldenkrais, 2009; Peper et al., 2010).
By experiencing and feeling the covert muscle tension, the person can understand how minimal movement and static positions can increase muscle tension that may cause discomfort. This unaware muscle tension can be monitored with electromyography (EMG) to show that the muscles have contracted of which the person is unaware as illustrated in the following two examples of looking at the screen (Figure 1) and lifting the shoulders during data entry (Figure 2).
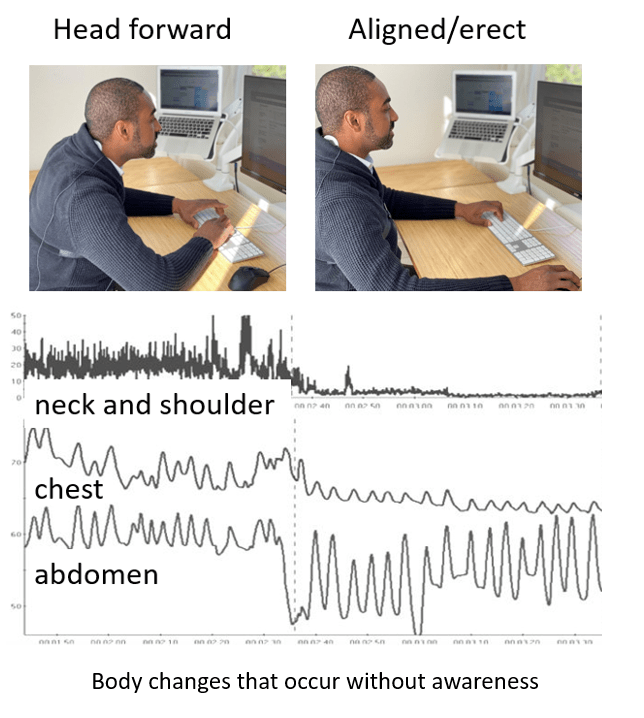
Figure 1. Effect of head craning forward to see the screen on neck and shoulder muscle tension and breathing pattern. Reproduced by permission from Peper, Harvey and Faass (2020).
When the person cranes their head forward to see the text on the screen, neck and back muscles tense. The person is unaware that neck and shoulder muscle tension increased, and breathing is irregular and thoracic when the head is forward. When the person sits erect, the muscle tension is lower and breathing is also slower and lower which supports regeneration.
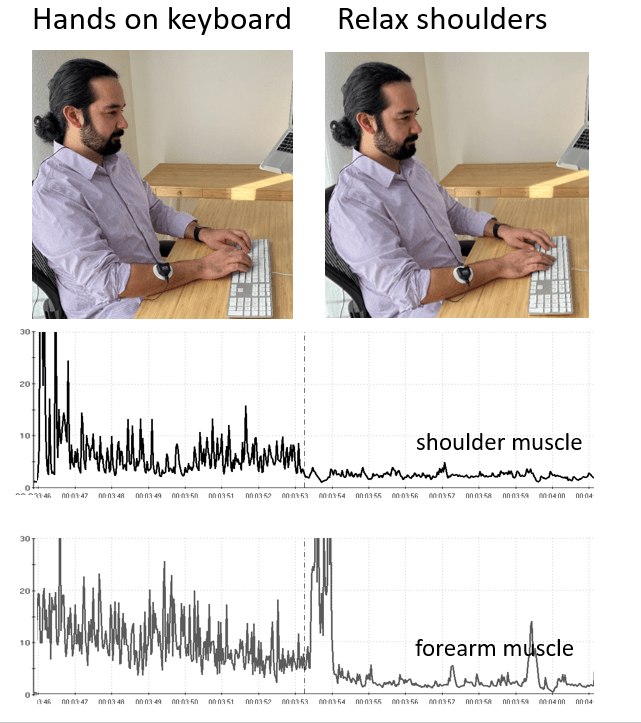
Figure 2. Effect of bringing the hands to the keyboard on shoulder and forearm tension. Reproduced by permission from Peper, Harvey, & Faass (2020).
When the person places their hands on the keyboard as compared to their hands resting on their lap, shoulder muscle and forearm tension often increase. Unknowingly, the participant raises their shoulders and holds that tension and postion as they rest their hands on the keyboard.
The purpose of the article is to:
- Emphasize the most people are unaware of holding low-level muscle tensions while working at the computer, texting or other tasks
- Offer somatic awareness practices and EMG monitoring as ways to demonstrate the covert tension
- Provide suggestions to reduce covert/dysponetic muscle tension.
Background
Neck, shoulder, back and eye discomfort have increased as many employees work at home. Unlike their office workstation, that may have been ergonomically arranged, at home the workstation is often their laptop placed on the kitchen table, desk, couch, bed or other location. When using a laptop, the person wither needs to lift their hands and arms up to the keyboard, which automatically increases the tension in the shoulders or look down at the keyboard, which increases neck and shoulder tension and causes the person to slouch. In many cases, the elbows are more abducted in order to type on the keyboard or use the mouse or trackpad. This abduction of elbows or the reaching forward and lifting of the arms occurs commonly if the desktop is too high (e.g, kitchen table as a desk) or if the person is pregnant or has larger waist. Similarly, arm and elbow abduction occur during daily activities such as stirring a pot, holding the steering wheel while driving, mousing at the computer, walking with objects attached to the belt that interfere with the swinging of the arms (e.g., the gun and Taser on the belt of police officer, hammer and other tools on the belt of a construction worker, or a backpack or handbag crossed over the shoulder), as shown in Figure 3a and 3b

Figure 3a, Walking with abducted arms to avoid hitting the hitting the object on the side of the waist.

Figure 3b. Arms forward and abducting while playing video games.
The abduction of the arm usually occurs without awareness of the resulting shoulder tension, except that at the end of the day the person feels stiffness, discomfort and sometimes pain in the shoulders.
Tactile experience of medial deltoid tension when abducting the arm developed by Wim Gijzen, PT
Part 1. Awareness of arm movement and tension
- Stand up and allow your arms to hang relaxed along the side of the trunk.
- Slightly move (abduct) your left arm away from the trunk (about 1 or 2 inches). Let the arm go and relax. Repeat this twice.
In most cases, participants report that they are aware that the arm started to move away from their trunk but unaware of the tension in the upper arm or shoulder (medial deltoid muscle).
Part 2. Feeling the muscle contraction of the unfelt muscle tension during abduction
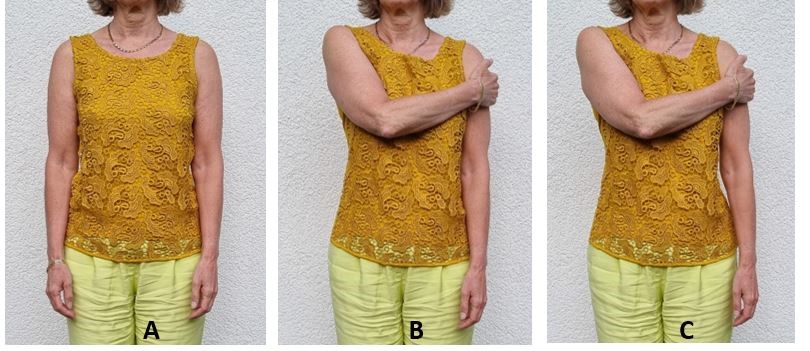
Figure 4. Standing relaxed with arms hanging down (A), feeling the medial deltoid (B), and moving the hand 1 or 2 inches away from the trunk while feeling the medial and posterior deltoid muscle activity (C).
- Stand relaxed and reach over with your right hand to your left shoulder. Place your fingers just over middle and backside of the top part of the upper arm (medial and posterior deltoid). Relax the shoulder and arm.
- Allow your right arm to hang down and be relaxed and feel the softness of the deltoid muscle.
- Begin to abduct your right arm 1–2 inches away from the side of your body. The same movement as you did in part 1b.
- Bring the arm back and relax. Repeat this movement twice.
Participants felt with their fingers the medial and posterior deltoid contracting before the arm even moved away from the body, even though they were unaware of the shoulder tension. In addition, they were surprised that the intent to move caused the muscle to tense.
EMG recording from deltoid muscle
EMG monitoring to demonstrate unaware muscle tension from the deltoid muscle as shown in Figure 5.
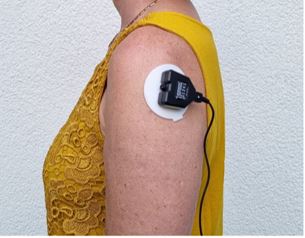
Figure 5. Electrode placement on the deltoid muscle.
- Place the electrodes over the deltoid as shown in Figure 5.
- Stand relaxed and begin to move (abduct) the left arm 1–2 inches away from the trunk as instructed in the previous exercise of the awareness exercise, and then relax.
- Stand relaxed and imagine that you are moving (abducting) the left arm 1–2 inches away from the trunk. Feel the elbow starting to move and then relax.
The moment the person begins to abduct—even though there is no visible movement of the arm and the person is unaware of the tension in their shoulder—the EMG recording of the medial and posterior deltoid shows the increased activity. In many cases even imagining and the movement will also increase the EMG activity, as shown in Figure 6.
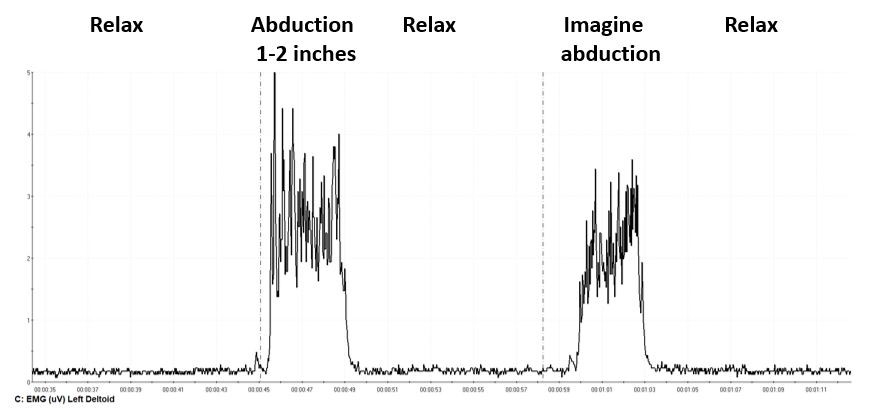
Figure 6. EMG recording of arm abduction and imagining the initiation of arm abduction
Discussion
Participants were surprised that they didn’t notice the muscle tension in their upper arm and shoulder until they felt it with their fingers or saw it on the EMG recording. Teaching participants to become aware of their muscle tension is a useful strategy to demonstrate that muscle tension occurs without awareness and demonstrate the need to take recuperation/regenerative breaks to relax the muscles. The important concept is that chronic low-level tension may lead to discomfort (Almendras & Peper, (2021). To reduce the risk of discomfort, the person needs interrupt static low-level tension with microbreaks or movement. Do the following practices to experience how experience how low static muscle tension causes discomfort.
The effect of static muscle tension
- Sit comfortably on a chair.
- Lift the right knee slightly up so that the foot is lifted one inch above the floor and keep holding it up, as illustrated in Figure 7. (For guided instructions see: https://peperperspective.com/2020/07/23/why-do-i-have-neck-and-shoulder-discomfort-at-the-computer/ [Peper, 2020])

Figure 7. Adapted from Peper, Harvey, & Faass, 2020; Peper, 2020Experience the effect of holding static muscle tension while lifting the knee up one or two inches. After a minute or so the person will experience the beginning of discomfort in their hip flexors.
Relax the leg and drop the foot to the floor.
Everyone reports that in less than a minute they became aware of the tension and discomfort. They also tend to hold their breath initially as they held their knee up. The discomfort increases if they continued to hold their knee up. Yet, these are the same muscles that we tighten and relax s during walking and then no discomfort occurs (Almendras & Peper, 2021).
The urge for movement after static muscle tension
- Make a fist and hold this for about 2 minutes.
- After a minute or so, experience the discomfort in your hand and forearm.
- Relax the fist and drop the hand on your lap.
After relaxing the hand, most people will move their fingers without thinking about it. When the person moves, the discomfort fades away. This experience illustrates that when discomfort occurs people need/tend to move. Each contraction is followed by short regeneration period.
These short practices illustrate how discomfort can develop if muscles are held contracted for extended time periods even at a very low level of tension.
Recommendations
- Guide participants through sensing the covert muscle tension of the deltoid so that they recognize that muscle contraction occurs without awareness.
- Guide the participant through the knee-lifting practice to understand the importance of relaxing muscles episodically.
- Encourage microbreaks to relax and regenerate the muscles (Peper, Harvey & Faass, 2020).
- Lift your arms up and let them flop down against the side of your body.
- Raise your shoulders and let them drop.
- Get up and move.
- Arrange the ergonomics so that the arms need not abduct.
- Place your hands on the steering wheel so that the upper arm can be relaxed while hanging downwards.
- Adjust the desk height so that the fingers can be at the keyboard without having to raise the shoulders or abduct the elbows. The keyboard height is usually lower than the height for a dining room table.
- Use a split keyboard so that the elbows are beside the trunk and flexed at about 90 degrees.
- Feel safe so that the arms and shoulder relax and to avoid triggering a defense reaction and protective posture.
- Practice stress reduction techniques, move or wiggle when feeling threatened, scared, or excessively sympathetically activated.
- Watch inspirational and uplifting media instead of fear-inducing media such as news.
- Take many large breaks (e.g., lunch walks, coffee breaks) and move the shoulders and arms so that the static tension is released.
- Interrupt static positions with short different activities (e.g. while working at home, clean the dishes during a break, put clothes in your washing machine, or do some stretches). When you perform different movements, the muscle activated in the previous activity can relax and regenerate.
As one of the participants said after taking many breaks during the day, “There is life after five.” What he meant was that before taking the breaks, he felt perfectly okay; however, after incorporating breaks, he had more energy and felt more alive at the end of the day.
*We thank Wim Gijzen, PT, for teaching the somatic exercise of feeling the deltoid muscle to develop awareness of muscle tension.
Listen to the expanded podcast created from this blogpost by Google Notebook LM.
See the following blogs to reduce TechStress:
References
Al-Hadidi, F., Bsisu, I., AlRyalat, S. A., Al-Zu’bi, B., Bsisu, R., Hamdan, M., Kanaan, T., Yasin, M., & Samarah, O. (2019). Association between mobile phone use and neck pain in university students: A cross-sectional study using numeric rating scale for evaluation of neck pain. PLoS ONE, 14(5), e0217231. https://doi.org/10.1371/journal.pone.0217231
Almendras, M. & Peper, E. (2021). Reactivate Your Second Heart, Biofeedback, 49(4), 99-102.https://doi.org/10.5298/1081-5937-49.04.07
David, D., Giannini, C., Chiarelli, F., & Mohn, A. (2021). Text Neck Syndrome in Children and Adolescents. International Journal of Environmental Research and Public Health, 18(4), 1565. https://doi.org/10.3390/ijerph18041565
Feldenkrais, M. (2009). Awareness through Movement: Easy-to-Do Health Exercises to Improve Your Posture, Vision, Imagination, and Personal Awareness. New York: Harper One.
Kett, A. R., Milani, T. L., & Sichting, F. (2021). Sitting for too long, moving too little: Regular muscle contractions can reduce muscle stiffness during prolonged periods of chair-sitting. Frontiers in Sports and Active Living, 3, 760533. https://doi.org/10.3389/fspor.2021.760533
Kumari, S., Kumar, R., & Sharma, D. (2021). Text Neck Syndrome: The Pain of Modern Era. International Journal of Health Sciences and Research, 11(11), 161–165. https://doi.org/10.52403/ijhsr.20211121
Peper, E. (July 23, 2020). Why do I have neck and shoulder discomfort at the computer? The PeperPerspective. https://peperperspective.com/2020/07/23/why-do-i-have-neck-and-shoulder-discomfort-at-the-computer/
Peper, E., Booiman, A., Tallard, M., & Takebayashi, N. (2010). Surface electromyographic biofeedback to optimize performance in daily life: Improving physical fitness and health at the worksite. Japanese Journal of Biofeedback Research, 37(1), 19–28. https://www.jstage.jst.go.jp/article/jjbf/37/1/37_KJ00006254804/_pdf
Peper, E., Harvey, R., & Faass, N. (2020). TechStress: How technology is hijacking our lives, strategies for coping, and pragmatic ergonomics. North Atlantic Books.
Sella, G.E. (2020). SEMG biofeedback reeducation and rehabilitation: The Sella protocol. Biofeedback, 48 (2): 41–44. https://doi.org/10.5298/1081-5937-48.1.3
Whatmore, G. B., & Kohli, D. R. (1968). Dysponesis: A neurophysiologic factor in functional disorders. Behavioral Science, 13(2), 102–124. https://doi.org/10.1002/bs.3830130203