Allow natural breathing with abdominal muscle biofeedback [1, 2]
Posted: April 26, 2016 Filed under: Breathing/respiration, self-healing, Uncategorized | Tags: abdominal breathing, biofeedback, EMG, Muscle feedback, respiration 7 CommentsWhen I allowed my lower abdomen to expand during inhalation without any striving and slightly constrict during exhalation, breathing was effortless. At the end of exhalation, I just paused and then the air flowed in without any effort. I felt profoundly relaxed and safe. With each effortless breath my hurry-up sickness dissipated.
Effortless breathing from a developmental perspective is a whole body process previously described by the works of Elsa Gindler, Charlotte Selver and Bess M. Mensendieck (Brooks, 1986; Bucholtz, 1994; Gilbert 2016, Mensendieck, 1954). These concepts underlie the the research and therapeutic approach of Jan van Dixhoorn (2008, 2014) and is also part of the treatment processes of Mensendieck/Cesar therapists (Profile Mensendeick) . During inhalation the body expands and during exhalation the body contracts. While sitting or standing, during exhalation the abdominal wall contracts and during inhalation the abdominal wall relaxes. This whole body breathing pattern is often absent in clients who tend to lift their chest and do not expand or sometimes even constrict their abdomen when they inhale . Even if their breathing includes some abdominal movement, often only the upper abdomen above the belly button moves while the lower abdomen shows limited or no movement. This may be associated with physical and emotional discomfort such as breathing difficulty, digestive problems, abdominal and pelvic floor pains, back pain, hyper vigilance, and anxiety. (The background, methodology to monitor and train with muscle biofeedback, and pragmatic exercises are described in detail in our recent published article, Peper, E., Booiman, A.C, Lin, I-M, Harvey, R., & Mitose, J. (2016). Abdominal SEMG Feedback for Diaphragmatic Breathing: A Methodological Note. Biofeedback. 44(1), 42-49.)
Some of the major factors that contribute to the absence of abdominal movement during breathing are (Peper et, 2015):
- ‘Designer jean syndrome’ (the modern girdle): The abdomen is constricted by a waist belt, tight pants or slimming underwear such as Spanx and in former days by the corset as shown in Figure 1 (MacHose & Peper, 1991; Peper & Tibbitts, 1994).
- Self-image: The person tends to pull his or her abdomen inward in an attempt to look slim and attractive.
- Defense reaction: The person unknowingly tenses the abdominal wall –a flexor response-in response to perceived threats (e.g., worry, external threat, loud noises, feeling unsafe). Defense reactions are commonly seen in clients with anxiety, panic or phobias.
- Learned disuse: The person covertly learned to inhibit any movement in the abdominal wall to protect themselves from experiencing pain because of prior abdominal injury or surgery (e.g., hernia or cesarean), abdominal pain (e.g., irritable bowel syndrome, dysmenorrhea, vulvodynia, pelvic floor pain, low back pain).
- Inability to engage abdominal muscles because of the lack of muscle tone.
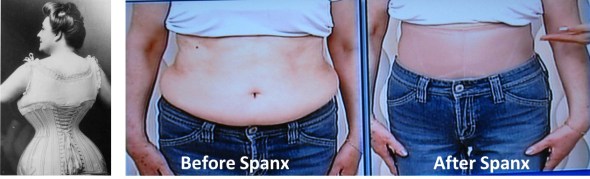 Figure 1. How clothing constricts abdominal movement. Previously it was a corset as shown on the left and now it is Spanx or very tight clothing which restricts the waist.
Figure 1. How clothing constricts abdominal movement. Previously it was a corset as shown on the left and now it is Spanx or very tight clothing which restricts the waist.
Whether the lower abdominal muscles are engaged or not (either by chronic tightening or lack of muscle activation), the resultant breathing pattern tends to be more thoracic, shallow, rapid, irregular and punctuated with sighst. Over time participants may not able to activate or relax the lower abdominal muscles during the respiratory cycle. Thus it is no longer involved in whole body movement which can usually be observed in infants and young children.
In our published paper by Peper, E., Booiman, A.C, Lin, I-M, Harvey, R., & Mitose, J. (2016), we describe a methodology to re-establish effortless whole body breathing with the use of surface electromyography (SEMG) recorded from the lower abdominal muscles (external/ internal abdominal oblique and transverse abdominis) and strategies to teach engagement of these lower abdominal muscles. Using this methodology, the participants can once again learn how to activate the lower abdominal muscles to flatten the abdominal wall thereby pushing the diaphragm upward during exhalation. Then, during inhalation they can relax the muscles of the abdominal wall to expand the abdomen and allow the diaphragm to descend as shown in Figure 2.
 Figure 2. Correspondence between respiratory strain gauge changes and SEMG activity during breathing. When the person exhales, the lower abdominal SEMG activity increases and when the person inhales the SEMG decreases.
Figure 2. Correspondence between respiratory strain gauge changes and SEMG activity during breathing. When the person exhales, the lower abdominal SEMG activity increases and when the person inhales the SEMG decreases.
The published article discusses the factors that contribute to the breathing dysregulation and includes guidelines for using SEMG abdominal recording. It describes in detail–with illustrations–numerous practices such as tactile awareness of the lower abdomen, active movements such as pelvic rocking and cats and dogs exercises that people can practice to facilitate lower abdominal breathing. One of these practices, Sensing the lower abdomen during breathing, is developed and described by Annette Booiman, Mensendieck therapist
Sensing the lower abdomen during breathing
The person place their hands below their belly button with the outer edge of hands resting on the groin. During inhalation, they practice bringing their lower abdomen/belly into their hands so that the person can feel the lower abdomen expanding. During exhalation, they pull their lower abdomen inward and away from their palms as shown in Figure 3.

Figure 3. Hands placed below the belly button to sense the movement of the lower abdomen.
Lower abdominal SEMG feedback is useful in retraining breathing for people with depression, rehabilitation after pregnancy, abdomen or chest surgery (e.g., Cesarean surgery, hernia, or appendectomy operations), anxiety, hyperventilation, stress-related disorders, difficulty to become pregnant or maintain pregnancy, pelvic floor problems, headache, low back pain, and lung diseases. As one participant reported:
“Biofeedback might be the single thing that helped me the most. When I began to focus on breathing, I realized that it was almost impossible for me since my body was so tightened. However, I am getting much better at breathing diaphragmatically because I practice every day. This has helped my body and it relaxes my muscles, which in turn help reduce the vulvar pain.”
REFERENCES
Mensendieck, B.M. (1954). Look better, feel better. Pymble, NSW, Australia: HarperCollins.
van Dixhoorn, J. (2008). Whole body breathing. Biofeedback. 3I(2), 54-58
Gilbert, C. (2016). Working with breathing , some early influences. Paper presented at the 47th Annual Meeting of the Association for Applied Psychophysiology and Biofeedback, Seattle WA, March 9-12, 2016.
1. Adapted from: Peper, E., Booiman, A., Lin, I-M, Harvey, R., & Mitose, J. (2016). Abdominal SEMG Feedback for Diaphragmatic Breathing: A Methodological Note. Biofeedback. 44(1), 42-49.
2. .I thank Annette Booiman for her constructive feedback in writing this blog.
Increase energy*
Posted: April 1, 2016 Filed under: self-healing, stress management, Uncategorized | Tags: cognitive therapy, energy level, health, Holistic health, stress management 2 CommentsAre you full of pep and energy, ready to do more? Or do you feel drained and exhausted? After giving at the office, is there nothing left to give at home? Do you feel as if you are on a treadmill that will never stop, that more things feel draining than energizing?
Feeling chronically drained is often a precursor for illness; conversely, feeling energized enhances productivity and encourages health. An important aspect of staying healthy is that one’s daily activities are filled more with activities that contribute to our energy than with tasks and activities that drain our energy. Similarly, Dr. John Gottman and colleagues have discovered that marriages prosper when there are many more positive appreciations communicated by each partner than negative critiques.
Energy is the subjective sense of feeling alive and vibrant. An energy gain is an activity, task, or thought that makes you feel better and slightly more alive—those things we want to or choose to do. An energy drain is the opposite feeling—less alive and almost depressed—those things we have to or must do; often something that we do not want to do. In almost all cases, it is not that we have to, should, or must do, it is a choice. Remember, even though you may say, “I have to study.” It is a choice. You can choose not to study and choose to drop out of school. Similarly, when you say, “I have to do the dishes,” it is still a choice. You can choose to do the dishes or let the dirty dishes pile up and just use paper plates.
Energy drains and gains are always unique to the individual; namely, what is a drain for one can be a gain for another. Energy drains can be doing the dishes and feeling resentful that your partner or children are not doing them, or anticipating seeing a person whom you do not really want to see. An energy gain can be meeting a friend and talking or going for a walk in the woods, or finishing a work project.
When patients with cancer start exploring what they truly would like to do and start acting on their unfulfilled dreams, a few experience that their health improves as documented by Dr. Lawrence LeShan in his remarkable book, Cancer as a Turning Point. So often our lives are filled with things that we should do versus want to do. In some cases, the lives we created are not the ones we wanted but the result of self-doubt and worry, “If I did do this, my family and friends won’t like me”, or “I am not sure I will be successful so I will do something that is safe.” Just ask yourself the question when you woke up this morning and most mornings this week, “How did you feel?” Did you felt happy and looking forward to the day?

Explore strategies to decrease the drains and increase the energy gains. Use the following exercise to increase your energy:
- For one week monitor your energy drains and energy gains. Monitor events, activities, thoughts, or emotions that increase or decrease energy at home and at work. For example some drains can include cleaning bathroom, cooking another meal, or talking to a family member on the phone, while gains can be taking a walk, talking to a friend, completing a work task. Be very honest, just note the events that change your energy level.
- After the week look over your notes and identify at least one activity that drains your energy and one activity that increases your energy
- Develop a strategy to decrease one of the energy drains. Be very specific how, where, when, with whom, and which situations decreasing the tasks that drain your energy. As you think about it, anticipate obstacles that may interfere with reducing your drains and develop new ways to overcome these obstacles such as trading tasks with others (I will cook if you clean the bathroom), setting time limits, giving yourself positive reward after finishing the task (a cup of tea, a text or phone message to a close friend, watching a video in the evening).
- Develop new ways how you can increase energy gains such as doing exercise, completing a task.
- Each day implement the behavior to reduce one less energy drain and increase one energy gain and observe what happens.
Initially it may seem impossible, many students and clients report that the practice made them aware, increased their energy, and they had more control over their lives than they thought. It also encouraged them to explore the question, “What is it that you really want to do?” So often we do energy drains because of convention, habit and fear which makes us feel powerless and suppresses our immune system thereby increasing the risk of illness. In observing the energy drains and energy gains, it may give the person a choice. Sometimes, the choice is not changing the tasks but how we think about it. Many of the things we do are not MUSTs; they are choices. I do the work at my job because I choose to benefits of earning money.
How your internal language impacts your energy**
Sit and think of something that you feel you have to do, should do, or must do. Something you slightly dread such as cleaning the dishes, doing a math assignment. While sitting say to yourself, “I have to do, should do, or must do_______________.” Keep repeating the phrase for a minute.
Then change your internal phrase and instead say one of the following phrases, “I choose to do,” “I look forward to doing,” or “I choose not to do _________.” Keep repeating the phrase for a minute.
Now compare how you felt. Almost all people feel slight less energy and more depressed when they are thinking, “I have to do,” “should do”, or must do”. While when they shifted the phrase to, “I choose to,” “I look forward to doing,” or “I choose not to do it,” they feel lighter, more expanded and more optimistic. When university students practice this change of language during the week, they find it was easier to start and complete their homework tasks.
Watch your thoughts; they become words.
Watch your words; they become actions.
Watch your actions; they become habits.
Watch your habits; they become character.
Watch your character; it becomes your destiny.
– Frank Outlaw
References
Gottman, J.M. & Silver, N. (2015). The Seven Principles for Making Marriage Work. New York: Harmony.
LeShan, L. (1999). Cancer as a Turning Point. New York: Plume
*Adapted from: Peper, E. (2016). Increase energy. Western Edition. April, pp4. http://thewesternedition.com/admin/files/magazines/WE-April-2016.pdf
**Adapted from: Gorter, R. & Peper, E. (2011). Fighting Cancer-A Nontoxic Approach to Treatment. Berkeley: North Atlantic Books, 107-200.