Breathing for Health: Four Part Audio Series for Regeneration and Well-Being
Posted: March 12, 2026 Filed under: attention, behavior, Breathing/respiration, CBT, emotions, healing, health, meditation, mindfulness, Pain/discomfort, relaxation, self-healing, stress management, Uncategorized | Tags: audio files, health, meditation, mental-health, mindfulness, wellness Leave a commentAdapted from Peper, E. (1990). Breathing for Health with Biofeedback. Montreal: Thought Technology Ltd and produced by Larry Klein.

Breathing is the most intimate rhythm of life. From the moment we are born until our last breath, our breath is always there—quietly sustaining us. And yet, most of the time, we are unaware of how we breathe or how profoundly it shapes our health. Learn how to use your breath to optimize your health and enhance your well-being.
Dysfunctional breathing patterns contribute significantly to a range of illnesses, ranging from chronic pain and anxiety to fatigue and stress-related disorders. For example, when anxious, breathing often becomes rapid and shallow; when calm, breathing tends to slow and deepen. Symptoms can often be reduced, and health, resilience, and a deep sense of well-being can be enhanced after mastering and implementing effortless breathing. Breathing affects the mind, body, emotions, and spirit; when you change your breathing, you change your state of being.
The audio series by Erik Peper was conceived and produced by Larry Klein co-founder of Thought Technology, Ltd in 1990 to make the science and practice of breathing with biofeedback accessible to everyone. Although it was recorded more than 35 years ago, the principles and instructions remain as relevant and evidence-based today as they were then.
It was designed to help you observe your own breathing patterns and cultivate the foundational skill of effortless diaphragmatic breathing. Even more importantly, it guides you in integrating this breathing pattern into daily activities so that it becomes your default—whether you are working, speaking, exercising, or resting.
The discussion and guided practices are both simple and profound. When you change how you breathe, you change how you regulate yourself. Breathing both reflects and influences your physiology, emotions, and cognitions—often outside of conscious awareness.
As you listen to and practice the techniques in this four-part audio series, you will develop greater awareness, appreciation, and mastery of effortless breathing. Enjoy applying these practices in everyday life until they become automatic. Like any skill, effortless breathing is learned through gentle, consistent practice—practice makes permanent.
Part 1: Background Information on Breathing
Listen once to understand the scientific foundations and underlying rationale
Part 2: Learning Slow Diaphragmatic Breathing
Listen repeatedly and practice consistently until the skill becomes natural, effortless, and reliable.
Part 3: Integrating Breathing in All Conditions
Alternate between Parts 2 and 3. Practice during everyday activities so the skill generalizes beyond formal sessions and becomes your default way of breathing.
Part 4: Integrating Breathing, Imagery and Meditation for Health
Experience how guided imagery and meditative awareness deepen and amplify the benefits of effortless breathing.
Additional Recommended Blogs to Support the Learning and Generalization of Effortless Breathing
Additional Recommended Blogs: How Breathing Can Help Relieve Pain
Hope for dry eyes and eye strain
Posted: March 2, 2026 Filed under: attention, behavior, Breathing/respiration, computer, digital devices, emotions, health, Pain/discomfort, relaxation, screen fatigue, self-healing, stress management, techstress, Uncategorized, vision, zoom fatigue | Tags: behavioral optometry, blinking, digital eye strain, dry eyes, eyes, ophthalmology, optometry, prarasympathetic regulation 1 CommentAdapted from: Peper, E., Yoshino, A., & Harvey, R. Hope for Dry eyes and Eye Strain: How Breathing-Blinking Patterns Influence Dry Eye.
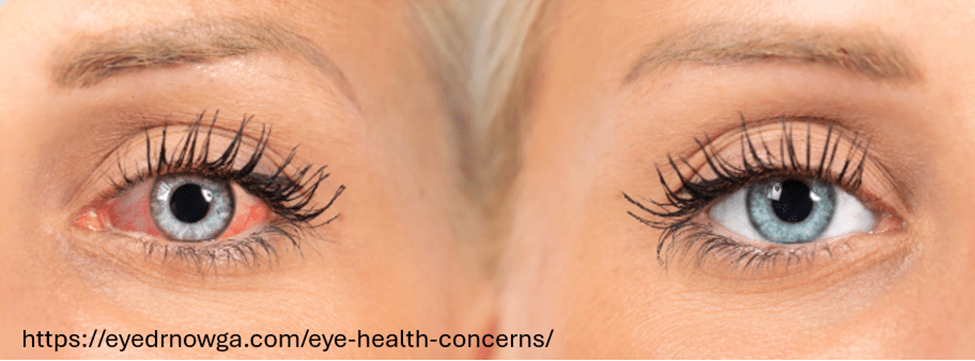
Many times during the day, I let my shoulders and face relax, and with each exhalation I feel the upper eyelids slightly dropping down at the same time as I am relaxing my jaw and mouth while sitting tall. I sense my tongue and throat sinking and feeling an increase in the space between my upper and lower molars. At the same time, I sense my eyes becoming soft and sinking down as my face muscle relax and are pulled down by gravity while sensing a gentle smile. My eyes are not trying to focus on anything. I continue to breathe slowly allowing a pause before inhaling and feel totally safe and at peace. While doing this, I sense moisture at the lower eyelids. After I have inhaled and as I exhale, I slowly open my eyes, and return to my work. My eyes feel slightly moist and as I blink, the eyelids glide smoothly over the corneal surface.
Background
Dry eyes and eye strain are far more common than most people realize. More than 50% of adults in the United States and Europe experience irritated or burning eyes, dryness, eye strain, headaches, tired or heavy eyes, sensitivity to bright light, and general eye discomfort (Wozniak et al., 2025). The prevalence increases with age and is higher among people who smoke, wear contact lenses, or spend excessive time looking at screens—typically more than six hours per day (Uchino et al,, 2013).
Prolonged, intense screen use—often referred to as digital eye strain or computer vision syndrome—occurs when people focus and concentrate, and the muscles involved with near vision contract and do not relax (Chu et al., 2014). During near vision, the ciliary muscles tighten around the lens to allow near focus, and the medial rectus muscles contract to converge the eyes. These muscles stay contracted and only relax when looking into the distance. This ongoing tension and increased sympathetic activation combined with reduced blinking decrease tearing, and contribute to dry eye symptoms because the tears are not able to provide adequate moisture. As a result, the eyes may become irritated, red and inflamed, which increases eye discomfort (Sheppard & Wolffsohn, 2018; Portello et al., 2012; Sheedy et al., 2003).
When someone is vigilant, fearful, or anticipates a threat, sympathetic activation increases (Ranti et al., 2020) and “eye blink are inhibited at precise moments in time so as to minimize the loss of visual information that occurs during a blink. The more important the visual information is to the viewer, the more likely he or she will be to inhibit blinking” (Ranti et al., 2020).
Without being aware, many people are in a chronic state of vigilance and unknowingly are scanning the world for threats to which they must react. Clinically, I often observe this when guiding clients in relaxation. For example, when I give the instruction, “Let me lift your hand,” some clients immediately lift their hand towards me. This nonverbal response suggests that they are constantly vigilant and are monitoring the world around them—always ready to act instead of trusting that they do not have to act and that the world is safe. In most cases, their breathing pattern tends to be shallow and thoracic.
Would it be possible that this ongoing vigilance,which increases sympathetic arousal contributes to the experience of dry eye syndrome? It could be one factor explaining why women have a higher incidence of dry eye disease as well as anxiety than men since the world is often less safe for women, and they breathe more thoracically and less diaphragmatically (abdominally) than men. Shallow chest breathing is also associated with increased in anxiety (Fugl-Meyer, 1974; Mendes et al., 2020; Wilhelm et al., 2001; Banushi eat al., 2023; McLean et al., 2011; Jalnapurkar, et al., 2018).
Note: The risk of dry eye can also be further increased by a wide range of medical conditions and medications, such as diabetes; glaucoma and glaucoma medications; allergies; autoimmune diseases; arthritis; thyroid disease; high cholesterol; acne treatments; antihistamines; antidepressants; and a history of refractive surgery, conjunctival infections, or corneal abrasions. Dry eye also occurs more frequently in women (Mohamed et al., 2024).
What is usually recommended to resolve dry eyes
The primary and effective first-line treatment to reduce the symptoms of dry eye disease is the use of artificial tears (lubricating eye drops) to provide relief (Maity et al., 2025). Another recommendation to reduce eye strain associated with computer use is to implement the 20/20/20 rule developed by the American Optometric Association–take a 20-second break every 20 minutes and look at something 20 feet away (AOA, 2026). Although the 20/20/20 practice can reduce eye strain and momentarily reduce some of the symptoms associated with dry eye disease especially if the eyes are closed, how we orient, breathe and look may contribute to the experience of dry eye discomfort.
Experience how to evoke dry eyes
Sit comfortably, look around, and observe how your eyes feel. Close your eyes. Now imagine there is a threat. Take a very quick gasp through an open mouth by inhaling into your upper chest and keep breathing very shallowly and irregularly. At the same time, open your eyes wide while being vigilant and looking for danger. Simultaneously, tense your body, inclining it slightly backward as if trying to avoid something. Do not blink, as you may miss the potential threat approaching you (adapted from Lemeignan et al., 1990; Bloch, 2017). A sample physiological recording of this pattern is shown in Figure 1.
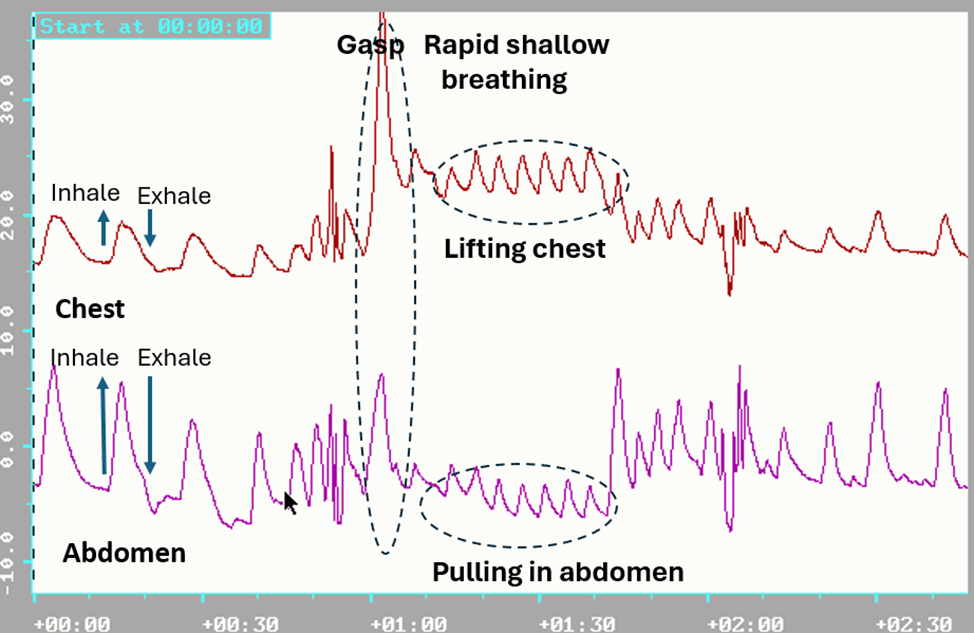
Figure 1. Breathing pattern in response to a threat; a rapid gasp into the chest and pulling the abdomen in to protect while breathing shallowly and rapidly.
Most participants report that almost immediately they feel their eyes getting cooler and after 15 seconds, drier. This facial, breathing, and posture pattern is an exaggeration of the somatic expression of fear that is evoked when we are vigilant and feel unsafe, and it increases sympathetic arousal (Kalawski, 2020).
In most cases, this pattern is automatic, and occurs without awareness, and increases sympathetic activity (Narkiewicz et al., 2006). On the other hand, slow diaphragmatic breathing tends to reduce sympathetic activity (Harada et al., 2014; Lehrer & Gevirtz, 2014). Clinically, the vigilance pattern can often be observed as a person slightly lifts and expands their chest during inhalation and drops and constricts it during exhalation, while breathing shallowly and rapidly without any abdomen expansion or constriction. It is often punctuated with brief breath holding and a reduced blinking rate during concentration.
To investigate these observations more systematically, we compared the practice of gasping while opening the eyes with gentle exhalation while opening the eyes—a pattern that may reduce sympathetic activation and alter the subjective sensation of eye dryness.
Participants: 13 males and 13 females; average age, 39 years
Procedure: While sitting comfortably with their eyes closed, participants were guided through the following two practices:
1.Gasp while opening the eyes
Sit comfortably and look around and observe how your eyes feel. Now close your eyes. Now imagine there is a threat. Take a very quick gasp through an open mouth by inhaling into your upper chest and keep breathing very shallowly and irregularly. At the same time, open your eyes wide while being vigilant and looking for danger. Simultaneously, tense your body, inclining it slightly backward as if trying to avoid something. Do not blink, as you may miss the potential threat approaching you. Repeat three times.
2. Gentle exhalation while opening the eyes
Sit comfortably and look around and observe how your eyes feel. Now close your eyes. Breathe comfortably and inhale by allowing your abdomen to extend and widen while feeling your eyes sinking in their sockets and becoming softer as you gently start exhaling. While gently exhaling, begin to open your eyes very slowly, looking down through your eyelashes without caring what you see, allowing your jaw and face muscles to relax and feeling a slight smile. When you feel the urge to inhale, allow your eyes to close and let your abdomen expand as you inhale slowly. Repeat three times.
After these two practices, the participants filled out a short assessment questionnaire in which they rated how their eyes felt on a scale from -5 (dry), 0 (normal), to 5 (moist/tearing), and rated which eye-opening procedure allowed their eyes to be more relaxed and moist.
Results
92.3% of the participants reported that opening their eyes during exhalation significantly increased eye relaxation and moisture, as shown in Figure 2. A one-way analysis of variance (ANOVA) revealed a significant difference between the inhale condition (M = −0.19, n = 26) and the exhale condition (M = 1.00, n = 25), F(1, 49) = 9.65, p = .003. The experience of eye irritation was correlated (r = 0.64) with the self-rating of experiencing anxiety and fear during the last three months.
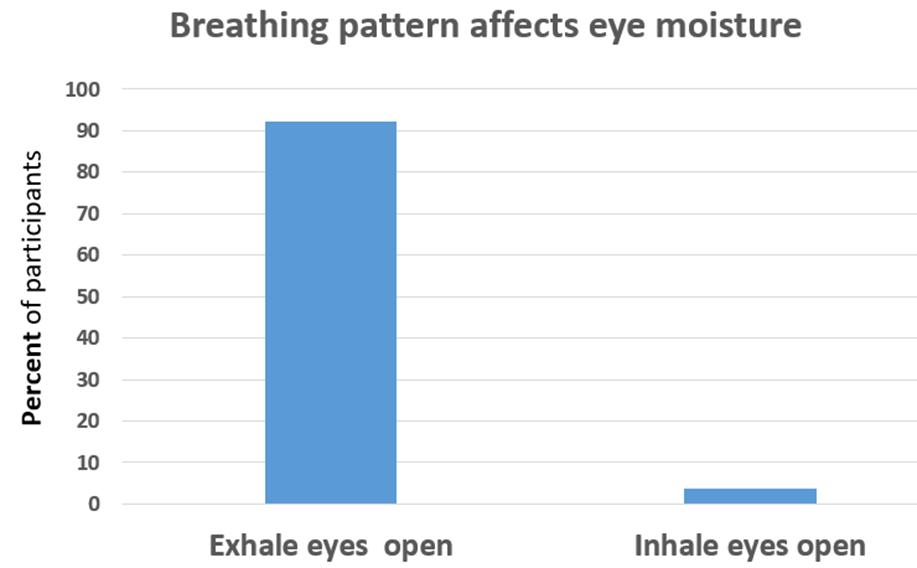
Figure 2. Gently opening the eyes during exhalation increases the experience of moisture and relaxation in the eyes.
Discussion
The results suggest that increased moisture and eye relaxation could be evoked by changing breathing-blinking patterns. Nearly all participants experienced an increase in tearing and eye relaxation; however, long-term benefits most likely occur if the person implements this practice many times during the day. By changing the breathingg-blink pattern and peacefully looking at the world with a smile, one would decrease sympathetic arousal and increase parasympathetic activity. This approach should be taught as the first self-care intervention to reduce eye irritation.
Recommendations to decrease dry eye and improve eye health
- Experience how the two different breathing and eye-opening practices described above affect your eye dryness or moistness.
- When you sense the first onset of minimal eye discomfort or when looking at screens on your computer or cellphone, implement the following practice for about 10 to 15 seconds. Allow your eyelids to close. Be aware of the sensations in your eyes, let your face and jaw relax as if they are being pulled down by gravity while sensing the eyes becoming soft and sinking into their sockets. Breathe diaphragmatically by allowing the abdomen to expand when you inhale. While gently exhaling, slowly open your eyes slightly while looking down with a gentle smile and sensing the moisture beginning to occur in the eyes. Repeat twice.
- During the day, implement the 20/20/20 vision-regeneration practice (every 20 minutes, take a 20-second break and look at something 20 feet away without caring what you see), as shown in Figure 3.
- Read and incorporated the many practices described in the superb book, Vision for Life; Ten Steps to Natural Eye Improvement, by Meir Schneider (2012).

Figure 3. The 20/20/20 rule poster to prevent eye strain (AOA, 2026).
Do these practices many times and be aware of the sensations in your eyes and face. This passive awareness, in conjunction with slower breathing, tends to reduce sympathetic arousal and increase parasympathetic activity, which facilitates increased tearing. As one participant reported when she practiced this:
What a surprise it was when I closed my eyes and breathed slowly and diaphragmatically, and then, as I began to exhale, I very slowly began to open my eyes while looking down and through my eyelashes, while feeling my eyes sink into their sockets. Tearing occurred spontaneously, and my eyes felt lubricated. What a relief. It provided hope that I could help myself instead of only depending on lubricating eye drops whenever my eyes felt dry and irritated.
Two books to maintain and improve vision and reduce techstress
Vision for Life: Ten Steps to Natural Eye Improvement by Meir Schneider (2016) offers many strategies you can immediately incorporate into your daily life to improve and restore your vision. It provides guidelines on how to reverse developing vision issues before they cause damage and how to remedy existing problems, including near- and far-sightedness, lazy eye, as well as more serious conditions such as cataracts, glaucoma, optic neuritis, detached retinas and retinal tears, macular degeneration, and retinitis pigmentosa.

TechStress: How Technology is Hijacking our Lives, Strategies for Coping, and Pragmatic Ergonomics by Erik Peper, Richard Harvey, and Nancy Faass (2020) offers practical tools to avoid the evolutionary traps that trip us up and address the problems associated with technological overuse. It includse effective strategies and practices that individuals can use to optimize their workspace, reduce physical strain, correct posture, and improve vision. It provides fresh insights on reducing stress and enhancing health.

Listen to the expanded podcast based on this blog produced with Google Notebook LM.
Additional blogs that offer strategies to improve vision
References
AOA. (2026). 20/20/20/ to prevent digital eyes strain. American Optometric Association. https://www.aoa.org/AOA/Images/Patients/Eye%20Conditions/20-20-20-rule.pdf
Banushi, B., Brendle, M., Ragnhildstveit, A., Murphy, T., Moore, C., Egberts, J., & Robison, R. (2023). Breathwork interventions for adults with clinically diagnosed anxiety disorders: A scoping review. Brain Sciences, 13(2), 256. https://doi.org/10.3390/brainsci13020256
Bloch, S. (2017). Alba Emoting: A scientific method for emotional induction. Scotts Valley, CA: CreateSpace Independent Publishing Platform. https://www.amazon.com/Alba-Emoting-Scientific-Emotional-Induction/dp/154254884
Chu, C.A., Rosenfield, M., Portello, J.K. (2014). Blink patterns: reading from a computer screen versus hard copy. Optom Vis Sci., 91(3),297-302. https://doi.org/10.1097/OPX.0000000000000157
Craig, J. P., Nichols, K. K., Akpek, E. K., et al. (2017). TFOS DEWS II definition and classification report. The Ocular Surface, 15(3), 276–283. https://doi.org/10.1016/j.jtos.2017.05.008
Dartt, D. A. (2009). Neural regulation of lacrimal gland secretory processes: Relevance in dry eye diseases. Progress in Retinal and Eye Research, 28(3), 155–177. https://doi.org/10.1016/j.preteyeres.2009.04.003
Fugi-Meyer, A.R. (1974). Relative respiratory contribution of the rib cage and the abdomen in males and females with special regard to posture. Respiration, 31(3), 240–251. https://doi.org/10.1159/000193113
Harada, D., Asanoi, H., Takagawa, J., Ishise, H., Ueno, H., Oda, Y., Goso, Y., Joho, S., & Inoue, H. (2014). Slow and deep respiration suppresses steady-state sympathetic nerve activity in patients with chronic heart failure: from modeling to clinical application. American Journal of Physiology-Heart and Circulatory Physiology, 307(8), H1159–H1168. https://doi.org/10.1152/ajpheart.00109.2014
Jalnapurkar, I., Allen, M., & Pigott, T. (2018). Sex differences in anxiety disorders: A review. Journal of Psychiatry, Depression & Anxiety, 4, 011. https://doi.org/10.24966/PDA-0150/100011
Kalawski, J.P. (2020) The Alba Method and the Science of Emotions. Integr. Psych. Behav. 54, 903–919. https://doi.org/10.1007/s12124-020-09525-4
Lehrer, P. M., & Gevirtz, R. (2014). Heart rate variability biofeedback: How and why does it work? Frontiers in Psychology, 5, Article 756. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4104929/
Lemeignan, M., Guitart, L., & Bloch, S. (1990). Autonomic differentiation of emotional effector pattern of 6 basic emotions. Proceedings of the Fifth International Congress of Psychophysiology, Budapest, July 9–14, 199
Maity, M., Allay, M. B., Ali, M. H., Basu, S., & Singh, S. (2025). Effect of different artificial tears on tear film parameters in dry eye disease. Optometry and Vision Science, 102(1), 37–43. https://doi.org/10.1097/OPX.0000000000002206
McLean, C. P., Asnaani, A., Litz, B. T., & Hofmann, S. G. (2011). Gender differences in anxiety disorders: Prevalence, course of illness, comorbidity and burden of illness. Journal of Psychiatric Research, 45(8), 1027–1035. https://doi.org/10.1016/j.jpsychires.2011.03.006
Mendes, L. P. S., Vieira, D. S. R., Gabriel, L. S., Ribeiro-Samora, G. A., Dornelas de Andrade, A., Brandão, D. C., Goes, M. C., Fregonezi, G. A. F., Britto, R. R., & Parreira, V. F. (2020). Influence of posture, sex, and age on breathing pattern and chest wall motion in healthy subjects. Brazilian Journal of Physical Therapy, 24(3), 240–248. https://doi.org/10.1016/j.bjpt.2019.02.007
Mohamed, Z., Alrasheed, S., Abdu, M., & Allinjawi, K. (2024). Dry eye disease prevalence and associated risk factors among the Middle East population: A systematic review and meta-analysis. Cureus, 16(9), e70522. https://doi.org/10.7759/cureus.70522
Narkiewicz, K., van de Borne, P., Montano, N., Hering, D., Kara, T., & Somers, V. K. (2006). Sympathetic neural outflow and chemoreflex sensitivity are related to spontaneous breathing rate in normal men. Hypertension, 47(1), 51–55. https://doi.org/10.1161/01.HYP.0000197613.47649.0
Peper, E., Harvey, R., & Faass, N. (2020). TechStress: How Technology is Hijacking our Lives, Strategies for Coping, and Pragmatic Ergonomics, North Atlantic Books. https://www.amazon.com/Beyond-Ergonomics-Prevent-Fatigue-Burnout/dp/158394768X
Portello, J.K., Rosenfield, M., Bababekova, Y., et al. (2012). Computer-related visual symptoms in office workers. Ophthalmic and Physiological Optics, 32, 375–82. https://doi.org/10.1111/j.1475-1313.2012.00925.x
Ranti, C., Jones, W., Klin, A. et al. Blink Rate Patterns Provide a Reliable Measure of Individual Engagement with Scene Content. Sci Rep 10, 8267 (2020). https://doi.org/10.1038/s41598-020-64999-x
Schneider, M. (2016). Vision for Life: Ten Steps to Natural Eye Improvement. North Atlantic Books. https://www.amazon.com/Vision-Life-Revised-Eyesight-Improvement/dp/1623170087
Sheedy, J.E., Hayes, J.N., & Engle, J.(2003). Is all asthenopia the same? Optom Vis Sci, 80, 732–9. https://doi.org/10.1097/00006324-200311000-00008
Sheppard, A. L., & Wolffsohn, J. S. (2018). Digital eye strain: prevalence, measurement and amelioration. BMJ open Ophthalmology, 3(1), e000146. https://doi.org/10.1136/bmjophth-2018-000146
Stern, M. E., Gao, J., Siemasko, K. F., Beuerman, R. W., & Pflugfelder, S. C. (2004). The role of the lacrimal functional unit in the pathophysiology of dry eye. Experimental Eye Research, 78(3), 409–416. https://doi.org/10.1016/j.exer.2003.09.003
Swamynathan, S. K., & Wells, A. (2020). Conjunctival goblet cells: Ocular surface functions, disorders that affect them, and the potential for their regeneration. The Ocular Surface, 18(1), 19–26. https://doi.org/10.1016/j.jtos.2019.11.005
Uchino, M., Yokoi, N., Uchino, Y., Dogru, M., Kawashima, M., Komuro, A., Sonomura, Y., Kato, H., Kinoshita, S., Schaumberg, D.A., & Tsubota, K. (2013). Prevalence of Dry Eye Disease and its Risk Factors in Visual Display Terminal Users: The Osaka Study. American Journal of Ophthalmology, 156(4), 759-766.e1, https://doi.org/10.1016/j.ajo.2013.05.040
The epidemiology of dry eye disease: report of the Epidemiology Subcommittee of the International Dry Eye WorkShop (2007). Ocul Surf. , 5(2), 93-107. https://doi.org/10.1016/s1542-0124(12)70082-4
Wilhelm, F. H., Gevirtz, R., & Roth, W. T. (2001). Respiratory dysregulation in anxiety, functional cardiac, and pain disorders: Assessment, phenomenology, and treatment. Behavior Modification, 25(4), 513–545. https://doi.org/10.1177/0145445501254003
Wozniak, P., et al. (2025, September 12–16). Dry eye symptoms, severity, treatment and unmet needs: An analysis of the United States of America and a multinational snapshot (NESTS Study) [Poster presentation]. 43rd Congress of the European Society of Cataract and Refractive Surgeons (ESCRS), Copenhagen, Denmark. https://www.sciencedaily.com/releases/2025/09/250914205829.htm
Ziemssen, F., & Ruprecht, K. W. (2005).Autonomic dysfunction in dry eye syndrome. Ophthalmologe, 102(8), 744–749. https://doi.org/10.1007/s00347-005-1169-1
Reduce Interpersonal Stress*
Posted: December 4, 2025 Filed under: attention, behavior, Breathing/respiration, CBT, emotions, Exercise/movement, healing, health, meditation, mindfulness, Pain/discomfort, stress management | Tags: health, mental-health, nutrition, wellness 3 CommentsAdapted from: Peper, E. & Harvey, R. Adjunctive techniques to reduce interpersonal stress at home. Biofeedback. 53(3), 54-57. https://rdcu.be/eMJqt

Stress often triggers defensive reactions—manifesting as anger, frustration, or anxiety that may mirror fight-or-flight responses. These reactions can reduce rational thinking, increase long-term health risks, and contribute to psychological and physiological disorders. and complicate the management of specific symptoms. Outlined are some pragmatic techniques that can be implemented during the day to interrupt and reduce stress.
After we had been living in our house for a few years, a new neighbor moved in next door. Within months, she accused us of moving things in her yard, blamed us when there was a leak in her house, claimed we were blowing leaves from her property onto other neighbors’ properties, and even screamed at her tenants to the extent that the police were called numerous times. Just looking at her house through the window was enough to make my shoulders tighten and leave me feeling upset.
When I drove home and saw her standing in front of her house, I would drive around the block one more time to avoid her while . . . feeling my body contract. Often, when I woke up in the morning, I would already anticipate conflict with my neighbor. I would share stories of my disturbing neighbor and her antics with my friends. They were very supportive and agreed with me that she was crazy. However, the acknowledgment and validation from my friends did not resolve my anger or indignation or the anxiety that was triggered whenever I saw my neighbor or thought of her. I spent far too much time anticipating and thinking about her, which resulted in tension in my own body—my heart rate would increase, and my neck and shoulders would tighten.
I decided to change. I knew I could not change her; however, I could change my reactivity and perspective. Thus, I practiced a “pause and recenter” technique. At the first moment of awareness that I was thinking about her or her actions, I would change my posture by sitting up straight, begin looking upward, breathe lower and slower, and then, in my mind’s eye, send a thought of goodwill streaming to her like an ocean wave flowing through and around her in the distance. I chose to do this series of steps because I believe that within every person, no matter how crazy or cruel, there is a part that is good, and it is that part I want to support.
I repeated this pause and recenter technique many times, especially whenever I looked in the direction of her house or saw her in her yard. I also reframed and reappraised her aggressive, negative behavior as her way of coping with her own demons. Three months later, I no longer reacted defensively. When I see her, I can say hello and discuss the weather without triggering my defensive reaction. I feel so much more at peace living where I am.
When stressed, angry, rejected, frustrated, or hurt, we so often blame the other person (Leary, 2015). The moment we think about that person or event, our anger, indignation, resentment, and frustration are triggered. We keep rehashing what happened. As we relive the experiences in our mind, we are unaware that we are also reliving bodily reactions to past events.
We are often unaware of the harm we are doing to ourselves until we experience physical symptoms such as high blood pressure, gastrointestinal distress, and muscle tightness along with behavioral and psychological symptoms such as insomnia, anxiety, or depression (Carney et al., 2006; Gerin et al., 2012). As we think of past events or interact again with a person involved in those past events, our body automatically responds with a defense reaction as if we were being threatened again in the present moment.
This defense reaction to memory of past threats from a “crazy” neighbor activates our fight-or-flight responses and increases sympathetic activation so that we can run faster and fight more ferociously to survive; however, this reaction also reduces blood flow through the frontal cortex—a process that reduces our ability to think rationally (van Dinther et al., 2024; Willeumier, et al., 2011). When we become so upset and stressed that our mind is captured by the other person, this reaction contributes to symptoms of chronic stress such as an increase in hypertension, myofascial pain, depression, insomnia, cardiovascular disease, and other chronic disorders (Duan et al., 2022; Russell et al., 2015; Suls, 2013).
Sharing our frustrations with friends and others is normal. It feels good to blame people for their personal limitations or mental illness; however, over time, blaming others avoids building adaptive capacity in strengthening skills that reduce chronic stress reactions (Fast & Tiedens, 2010; Lou et al., 2023). The time spent rehashing and justifying our feelings diminishes the time we spend in the present moment and our focus on upcoming opportunities.
In the moment of an encounter with a difficult neighbor, we may not realize that we have a choice. Some people keep living and reacting to past hurts or losses perpetually. Some people can learn to let go and/or forgive and make space in favor of considering new opportunities for learning and growth. Although the choice is ours, it is often very challenging to implement—even with the best intentions—because we react automatically when reminded of past hurts (seeing that person, anticipating meeting or actually meeting that person who caused the hurt, or being triggered by other events that evoke memories of the pain).
What Can You Do
Choose to change your response. Choose to reduce reactivity. Choosing adaptive reactions does not mean you condone what happened or agree that the other person was right. You are just choosing to live your life and not continue to be captured by nor react to the previous triggers. Many people report that after implementing some of the practices described below along with many other stress management techniques, their automatic reactivity was noticeably decreased. They report that their chronic stress symptoms were reduced and they have the freedom to live in present instead of being captured by the painful past.
Pause and Recenter by Sending Goodwill
Our automatic reaction to the trigger elicits a defense reaction that reduces our ability to think rationally. Therefore, the moment you anticipate or begin to react, take three very slow diaphragmatic breaths, inhaling for approximately 4–5 seconds and exhaling for about 5–6 seconds, where one in-and-out breath takes about 10 seconds to complete. As you inhale, allow your abdomen to expand; then as you exhale, slowly make yourself tall and look up. Looking up allows easier access to empowering and positive memories (Peper et al., 2017).
Continue looking up, inhaling slowly to allow the abdomen to expand. Repeat this slow breath again. On the third long, slow breath, while looking up, evoke a memory of someone in whose presence you felt at peace and who loves you, such as your grandmother, aunt, uncle, or even a pet. Reawaken positive feelings associated with memories of being loved. Allow a smile inwardly or outwardly and soften your eyes as you experience the loving memory.
Next, put your hands on your chest, take another long slow breath as your abdomen expands, and as you exhale bring your hands away from your chest and stretch them out in front of you. At the same time in your mind’s eye, imagine sending goodwill to that person involved in the interpersonal conflict that previously evoked your stress response. As if you are sending an ocean wave that is streaming outward to the person.
As you do the pause and recenter technique, remember you are not condoning what happened; instead, you are sending goodwill to that person’s positive aspect. From this perspective, everyone has an intrinsic component—however small—that some label as the individual’s human potential, Christ nature or Buddha nature.

Why would this be effective? This practice short-circuits the automatic stress response and provides time to recenter, interrupting ongoing rumination by shifting the mind away from thoughts about the person or event that induced stress toward a positive memory. By evoking a loving memory from the past, we facilitate a reduction in arousal, evoke a positive mood, and decrease sympathetic nervous system activation (Speer & Delgado, 2017). Slower diaphragmatic breathing also reduces sympathetic activation (Birdee et al., 2023; Siedlecki et al., 2022). By combining body-centered and mind-centered techniques, we can pause and create the opportunity to respond positively rather than reacting with anger and hurt.
Practice Sending Goodwill the Moment You Wake Up
So often when we wake up, we anticipate the challenges, and even the prospect of interacting with a person or event heightens our defense reaction. Therefore, as soon as you wake up, sit at the edge of the bed, repeat the previous practice, pause, and center. Then, as you sit at the edge of the bed, slightly smile with soft eyes, look up, and inhale as your abdomen expands. Then, stamp a foot into the floor while saying, “Today is a new day.” Next, inhale, allowing your abdomen to expand; as you look up, stamp the opposite foot on the floor while saying, “Today is a new day.” Finally, send goodwill to the person who previously triggered your defensive reaction.
Why would this be effective? Looking up makes it easier to access positive memories and thoughts. Stamping your foot on the ground is a nonverbal expression of determination and anchors the thought of a new day, thereby focusing on new opportunities (Feldman, 2022).
Interrupt the Stress Response with the ABCs
The moment you notice discomfort, pain, stress, or negative thoughts, interrupt the cycle with a simple ABC strategy (Peper, 2025):
- Adjust posture and look up
- Breathe by allowing your abdomen to relax and expand while inhaling
- Change your internal dialogue, smile and focus on what you want to do
Why would this be effective? By shifting your posture and gently looking upward, you make it easier to access positive and empowering memories and thoughts (Peper et al., 2019). This simple change in body position can interrupt habitual stress responses and open the doorway to more constructive states.
Slow, diaphragmatic breathing further supports this process by reducing sympathetic arousal and restoring a sense of calm. As your breathing deepens, clarity of mind increases, allowing you to respond rather than react (Peper et al, 2024b; Matto et al, 2025).
Equally important is transforming critical, judgmental, or negative self-talk into affirmative, supportive statements. Describe what you want to do—rather than what you want to avoid. This reframing creates a clear internal guide and significantly increases the likelihood that you will achieve your desired goals.
Complete the Alarm Reaction a Burst of Physical Activity
When you feel overwhelmed and fully captured by a stress reaction, one of the most effective strategies is to complete the fight-flight response with a brief burst of intense physical activity. This momentary action such as running in place, vigorously shaking your arms, or doing a few rapid push-offs from a wall (Peper et al., 2024a). After completing the physical activity implement your stress management strategies such as breathing, cognitive reframing, meditation, etc.
Why would this be effective? The intense physical activity discharges the excessive physiological arousal and interrupts the cycle of rumination. For practical examples and step-by-step guidance, see the article Quick Rescue Techniques When Stressed (Peper et al., 2024a) or the accompanying blog post: https://peperperspective.com/2024/02/04/quick-rescue-techniques-when-stressed/
Discuss Your Issue from the Third-Person Perspective
When thinking, ruminating, talking, texting, or writing about the event, discuss it from the third-person perspective. Replace the first-person pronoun “I” with “she” or “he.” For example, instead of saying “I was really pissed off when my boss criticized my work without giving any positive suggestions for improvement,” say “He was really pissed off when his boss criticized his work without offering any positive suggestions for improvement.”
Why would this be effective? The act of substituting the third-person pronoun for the first-person pronoun interrupts our automatic reactivity because it requires us to observe and change our language, which activates parts of the frontal cortex. This third-person/first-person process creates a psychological distance from our feelings, allowing for a more objective and calmer perspective on the situation, effectively reducing stress by stepping back from the immediate emotional response (Moser et al., 2017). This process can be interpreted as meaning that you are no longer fully captured by the emotions, as you are simultaneously the observer of your own inner language and speech.
Compare Yourself with Others Who are less Fortunate
When you feel sorry for yourself or hurt, take a breath, look upward, and compare yourself with others who are suffering much more. In that moment, consider yourself incredibly lucky compared with people enduring extreme poverty, bombings, or severe disfigurement. Be grateful for what you have.
Why would this be effective? Research shows that when we compare ourselves with people who are more successful, we tend to feel worse—especially when we have low self-esteem. However, when we compare ourselves with others who are suffering more, we tend to feel better (Aspinwall, & Taylor, 1993). This comparison relativizes our perspective on suffering, making our own hardships and suffering seem less significant compared with the severe suffering of others.
Conclusion
It is much easier to write and talk about these practices than to implement them. Reminding yourself to implement them can be very challenging. It requires significant effort and commitment. In some cases, the benefits are not experienced immediately; however, when practiced many times during the day for six to eight weeks, many people report feeling less resentment and experience a reduction in symptoms and improvements in health and relationships.
*This blog was inspired by the podcast “No Hard Feelings,” an episode on Hidden Brain produced by Shankar Vedantam (2025) that featured psychologist Fred Luskin, and the wisdom taught by Dora Kunz (Kunz & Peper, 1983, 1984a, 1984b, 1987).
See the following posts for more relevant information
References
Aspinwall, L. G., & Taylor, S. E. (1993). Effects of social comparison direction, threat, and self-esteem on affect, self-evaluation, and expected success. Journal of Personality and Social Psychology, 64(5), 708–722. https://doi.org/10.1037/0022-3514.64.5.708
Birdee, G., Nelson, K.,Wallston, K., Nian, H., Diedrich, A., Paranjape, S., Abraham, R., & Gamboa, A. (2023). Slow breathing for reducing stress: The effect of extending exhale. Complementary Therapies in Medicine, 73. https://doi.org/10.1016/j.ctim.2023.102937
Carney, C. E., Edinger, J. D., Meyer, B., Lindman, L., & Istre, T. (2006). Symptom-focused rumination and sleep disturbance. Behavioral Sleep Medicine, 4(4), 228–241. https://doi.org/10.1207/s15402010bsm0404_3
Defayette, A. B., Esposito-Smythers, C., Cero, I., Harris, K. M.,Whitmyre, E. D., & López, R. (2023). Interpersonal stress and proinflammatory activity in emerging adults with a history of suicide risk: A pilot study. Journal of Mood and Anxiety Disorders, 2. https://doi.org/10.1016/j.xjmad.2023.100016
Dienstbier, R. A. (1989). Arousal and physiological toughness: Implications for mental and physical health. Psychological Review, 96(1), 84. https://doi.org/10.1037/0033-95x.96.1.84
Duan, S., Lawrence, A., Valmaggia, L., Moll, J., & Zahn, R. (2022). Maladaptive blame-related action tendencies are associated with vulnerability to major depressive disorder. Journal of Psychiatric Research, 145, 70–76. https://doi.org/10.1016/j.jpsychires.2021.11.043
Fast, N. J., & Tiedens, L. Z. (2010). Blame contagion: The automatic transmission of self-serving attributions. Journal of Experimental Social Psychology, 46(1), 97–106. https://doi.org/10.1016/j.jesp.2009.10.007
Feldman, Y. (2022). The dialogical dance–A relational embodied approach to supervision. In C. Butte & T. Colbert (Eds.), Embodied approaches to supervision: The listening body (chap. 2). Routledge. https://www.amazon.com/Embodied-Approaches-Supervision-C%C3%A9line-Butt%C3%A9/dp/0367473348
Gerin,W., Zawadzki,M. J., Brosschot, J. F., Thayer, J. F., Christenfeld, N. J., Campbell, T. S., & Smyth, J. M. (2012). Rumination as a mediator of chronic stress effects on hypertension: A causal model. International Journal of Hypertension, 2012, 453465. https://doi.org/10.1155/2012/453465
Hase, A., O’Brien, J., Moore, L. J., & Freeman, P. (2019). The relationship between challenge and threat states and performance: A systematic review. Sport, Exercise, and Performance Psychology, 8(2), 123. https://doi.org/10.1037/spy0000132
Hassamal, S. (2023). Chronic stress, neuroinflammation, and depression: An overview of pathophysiological mechanisms and emerging anti-inflammatories. Frontiers in Psychiatry,
14, 1130989. https://doi.org/10.3389/fpsyt.2023.1130989
Kunz, D., & Peper, E. (1983). Fields and their clinical implications—Part III: Anger and how it affects human interactions. The American Theosophist, 71(6), 199–203. https://www.researchgate.net/publication/280777019_Fields_and_their_clinical_implications-Part_III_Anger_and_how_it_affects_human_interactions
Kunz, D., & Peper, E. (1984a). Fields and their clinical implications IV: Depression from the energetic perspective: Etiological underpinnings. The American Theosophist, 72(8), 268–275. https://www.researchgate.net/publication/280884054_Fields_and_their_clinical_implications_Part_IV_Depression_from_the_energetic_perspective-Etiological_underpinnings
Kunz, D., & Peper, E. (1984b). Fields and their clinical implications V: Depression from the energetic perspective: Treatment strategies. The American Theosophist, 72(9), 299–306. https://www.researchgate.net/publication/280884158_Fields_and_their_clinical_implications_Part_V_Depression_from_the_energetic_perspective-Treatment_strategies
Kunz, D., & Peper, E. (1987). Resentment: A poisonous undercurrent. The Theosophical Research Journal, IV(3), 54–59. Also in: Cooperative Connection, IX(1), 1–5. https://www.researchgate.net/publication/387030905_Resentment_Continued_from_page_4
Leary, M. R. (2015). Emotional responses to interpersonal rejection. Dialogues in Clinical Neuroscience, 17(4), 435–441. https://doi.org/10.31887/DCNS.2015.17.4/mleary
Lou, Y., Wang, T., Li, H., Hu, T. Y., & Xie, X. (2023). Blame others but hurt yourself: Blaming or sympathetic attitudes toward victims of COVID-19 and how it alters one’s health status. Psychology & Health, 39(13), 1877–1898. https://doi.org/10.1080/08870446.2023.2269400
Matto, D., Peper, E., & Harvey, R. (2025). Monitoring and coaching breathing patterns and rate. Townsend Letter-Innovative Health Perspectives. https://townsendletter.com/monitoring-and-coaching-breathing-patterns-and-rate/
Moser, J. S., Dougherty, A., Mattson, W. I., Katz, B., Moran, T. P.,Guevarra, D., Shablack, H.,Ayduk,O., Jonides, J., Berman, M. G., & Kross, E. (2017). Third-person self-talk facilitates emotion regulation without engaging cognitive control: Converging evidence from ERP and fMRI. Scientific Reports, 7(1), 4519. https://doi.org/10.1038/s41598-017-04047-3
Peper, E. (2025). Breathe Away Menstrual Pain- A Simple Practice That Brings Relief. the peper perspective-ideas on illness, health and well-being from Erik Peper. https://peperperspective.com/2025/11/22/6825/
Peper, E., Harvey, R., & Hamiel, D. (2019). Transforming thoughts with postural awareness to increase therapeutic and teaching efficacy. NeuroRegulation, 6(3), 153-169. https://doi.org/10.15540/nr.6.3.1533-1
Peper, E., Lin, I.-M., Harvey, R., & Perez, J. (2017). How posture affects memory recall and mood. Biofeedback, 45(2), 36–41. https://doi.org/10.5298/1081-5937-45.2.01
Peper, E., Oded, Y., & Harvey, R. (2024a). Quick somatic rescue techniques when stressed. Biofeedback, 52(1), 18–26. https://doi.org/10.5298/982312
Peper, E., Oded, Y., Harvey, R., Hughes, P., Ingram, H., & Martinez, E. (2024b). Breathing for health: Mastering and generalizing breathing skills. Townsend Letter-Innovative Health Perspectives. November 15, 2024. https://townsendletter.com/suggestions-for-mastering-and-generalizing-breathing-skills/
Russell, M. A., Smith, T. W., & Smyth, J. M. (2015). Anger expression, momentary anger, and symptom severity in patients with chronic disease. Annals of Behavioral Medicine, 50(2), 259–271. https://doi.org/10.1007/s12160-015-9747-7
Siedlecki, P., Ivanova, T. D., Shoemaker, J. K., & Garland, S. J. (2022). The effects of slow breathing on postural muscles during standing perturbations in young adults. Experimental Brain Research, 240, 2623–2631. https://doi.org/10.1007/s00221-022-06437-0
Speer, M. E., & Delgado, M. R. (2017). Reminiscing about positive memories buffers acute stress responses. Nature Human Behaviour, 1, 0093. https://doi.org/10.1038/s41562-017-0093
Suls, J. (2013). Anger and the heart: Perspectives on cardiac risk, mechanisms and interventions. Progress in Cardiovascular Diseases, 55(6), 538–547. https://doi.org/10.1016/j.pcad.2013.03.002
van Dinther, M., Hooghiemstra, A. M., Bron, E. E., Versteeg, A., et al. (2024). Lower cerebral blood flow predicts cognitive decline in patients with vascular cognitive impairment. Alzheimer’s & Dementia: The Journal of the Alzheimer’s Association, 20(1), 136–144. https://doi.org/10.1002/alz.13408
Vedantam, S. (2025). No hard feelings. Hidden brain. Accessed February 5, 2025. https://hiddenbrain.org/podcast/no-hard-feelings/
Willeumier, K., Taylor, D. V., & Amen, D. G. (2011). Decreased cerebral blood flow in the limbic and prefrontal cortex using SPECT imaging in a cohort of completed suicides. Translational Psychiatry, 1(8), e28. https://doi.org/10.1038/tp.2011.28
Zannas, A. S., & West, A. E. (2014). Epigenetics and the regulation of stress vulnerability and resilience. Neuroscience, 264, 157–170. https://doi.org/10.1016/j.neuroscience.2013.12.003
Breathe Away Menstrual Pain- A Simple Practice That Brings Relief *
Posted: November 22, 2025 Filed under: attention, behavior, biofeedback, Breathing/respiration, cognitive behavior therapy, education, emotions, Neck and shoulder discomfort, Pain/discomfort, posture, relaxation, self-healing, stress management, Uncategorized | Tags: dysmenorrhea, health, meditation, menstrual cramps, mental-health, mindfulness, wellness 2 CommentsAdapted from: Peper, E. Harvey, R., Chen, & Heinz, N. (2025). Practicing diaphragmatic breathing reduces menstrual symptoms both during in-person and synchronous online teaching. Applied Psychophysiology and Biofeedback, Published online: 25 October 2025. https://rdcu.be/eMJqt https://doi.org/10.1007/s10484-025-09745-7
“Once again, the pain starts—sharp, deep, and overwhelming—until all I can do is curl up and wait for it to pass. There’s no way I can function like this, so I call in sick. The meds take the edge off, but they don’t really fix anything—they just mask it for a little while. I usually don’t tell anyone it’s menstrual pain; I just say I’m not feeling well. For the next couple of days, I’m completely drained, struggling just to make it through.
Many women experience discomfort during menstruation, from mild cramps to intense, even disabling pain. When the pain becomes severe, the body instinctively responds by slowing down—encouraging rest, curling up to protect the abdomen, and often reaching for medication in hopes of relief. For most, the symptoms ease within a day or two, occasionally stretching into three, before the body gradually returns to balance.
Another helpful approach is to practice slow abdominal breathing, guided by a breathing app FlowMD. In our study led by Mattia Nesse, PhD, in Italy, the response of one 22-year-old woman illustrated the power of this simple practice.
“Last night my period started, so I was a bit discouraged because I knew I’d get stomach pain, etc. On the other hand, I said, “Okay, let’s see if the breathing works,” and it was like magic — incredible. I’ll need to try it more times to understand whether it consistently has the same effect, but right now it truly felt magical. Just 3 minutes of deep breathing with the app were enough, and I’m not saying I don’t feel any pain anymore, but it has decreased a lot, so thank you! Thank you again for this tool… I’m really happy!”
The Silent Burden of Menstrual Pain
Menstrual pain, or dysmenorrhea, affects most women at some point in their lives — often silently. For many, the monthly cycle brings not only physical discomfort but also shame, fatigue, and interruptions to work or school. It is one of the leading causes of absenteeism and reduced productivity worldwide (Itani et al., 2022; Thakur & Pathania, 2022). In addition, the estimated health cost ranged from US $1367 to US$ 7043 per year (Huang et al., 2021). Yet, despite its prevalence, most women are never taught how to use their own physiology to ease these symptoms.
The Study (Peper et al, 2025)
Seventy-five university women participated across two upper-division Holistic Health courses. Forty-nine practiced 30 minutes per day of breathing and relaxation over five weeks as well as practicing the moment they anticipated or felt discomfort; twenty-six served as a comparison group without a specific daily self-care routine. Students rated change in menstrual symptoms on a scale from –5 (“much worse”) to +5 (“much better”). For the detailed steps in training, see the blog: https://peperperspective.com/2023/04/22/hope-for-menstrual-cramps-dysmenorrhea-with-breathing/ (Peper et al., 2023).
What changed
The results were striking. Women who practiced breathing and relaxation showed significant decrease in menstrual symptoms compared to the non-intervention group (p = 0.0008) as shown in Figure 1.

Figure 1. Decrease in menstrual symptoms as compared to the control group after implementing slow diaphragmatic breathing.
Why does breathing and posture change have a beneficial effect?
When you stay curled up, your abdomen becomes compressed, leaving little room for the lower belly to relax or for the diaphragm to move freely. The result? Tension builds, and pain often increases.
To reverse this, create space for relaxation. Gently loosen your waist and let your abdomen expand as you inhale. Uncurl your body—lengthen your spine and open your chest, as shown in Figure 2. With each easy breath, you invite calm and allow your body to shift from tension to ease.
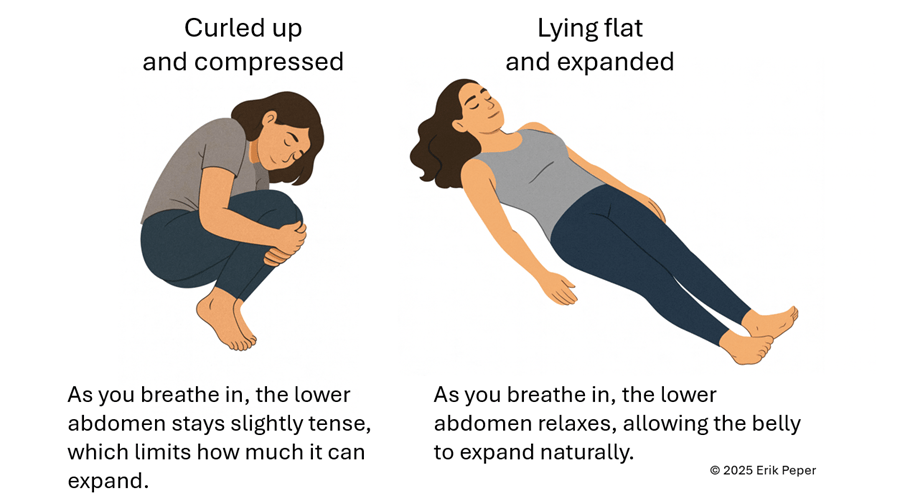
Figure 2. Curling up compresses the abdomen and prevents relaxation of the lower belly. In contrast, lying flat with the body gently expanded allows the abdomen to move freely with each breath, which can help reduce menstrual discomfort.
In contrast, slow abdominal or diaphragmatic breathing activates the body’s natural relaxation response. It quiets the stress-driven sympathetic nervous system, calms the mind, and improves circulation in the abdominal area. With each slow breath in, the abdomen gently expands while the pelvic floor and abdominal muscles relax. As you exhale, these muscles naturally tighten slightly, helping to massage and move blood and lymph through the abdominal region. This rhythmic movement supports healing and ease, as illustrated in Figure 3.
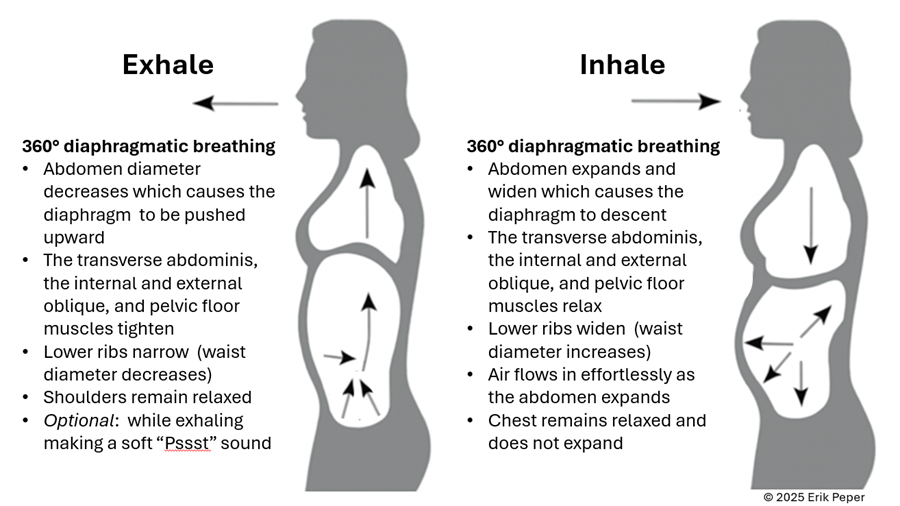
Figure 3. The dynamic process of diaphragmatic breathing.
The process of slower, lower diaphragmatic breathing
When lying down, rest comfortably on your back with your legs slightly apart. Allow your abdomen to rise naturally as you inhale and fall as you exhale. As you breathe out, imagine the air flowing through your abdomen, down your legs, and out through your feet. To deepen this sensation, you can ask a partner to gently stroke from your abdomen down your legs as you exhale—helping you sense the flow of release through your body.
Gently focus on slow, effortless diaphragmatic breathing. With each inhalation, your abdomen expands, and the lower belly softens. As you exhale, the abdomen gently goes down pushing the diaphragm upward and allowing the air to leave easily. Breathing slowly—about six breaths per minute—helps engage the body’s natural relaxation response.
If you notice that your breath is staying high in your chest instead of expanding through the abdomen, your symptoms may not improve and can even increase. One participant experienced this at first. After learning to let her abdomen expand with each inhalation while keeping her shoulders and chest relaxed, her next menstrual cycle was markedly easier and far less uncomfortable. The lesson is clear: technique matters.
“During times of pain, I practiced lying down and breathing through my stomach… and my cramps went away within ten minutes. It was awesome.” — 22-year-old college student
“Whenever I felt my cramps worsening, I practiced slow deep breathing for five to ten minutes. The pain became less debilitating, and I didn’t need as many painkillers.” — 18-year-old college student
These successes point out that it’s not just breathing — it’s how you breathe by providing space for the abdomen to expand during inhalation.
Practice: How to Do Diaphragmatic Breathing
- Find a quiet space. Lie on your back or sit comfortably erect with your shoulders relaxed.
- Place one hand on your chest and one on your abdomen.
- Inhale slowly through your nose for about 3–4 seconds. Let your abdomen expand as you breathe in — your chest should remain relaxed.
- Exhale gently through your mouth for 4—6 seconds, allowing the abdomen to fall or constrict naturally.
- As you exhale imagine the air moving down your arms, through your abdomen, down your legs, and out your feet
- Practice daily for 20 minutes and also for 5–10 minutes during the day when menstrual discomfort begins.
- Add warmth. Placing a warm towel or heating pad over your abdomen can enhance relaxation while lying on your back and breathing slowly.
With regular practice and implementing it during the day when stressed, this simple method can reduce cramps, promote calm, and reconnect you with your body’s natural rhythm.
Implement the ABCs during the day
The ABC sequence—adapted from the work of Dr. Charles Stroebel, who developed The Quieting Reflex (Stroebel, 1982)—teaches a simple way to interrupt stress reactions in real time. The moment you notice discomfort, pain, stress, or negative thoughts, interrupt the cycle with a simple ABC strategy:
A — Adjust your posture
Sit or stand tall, slightly arch your lower back and allowing the abdomen to expand while you inhale and look up. This immediately shifts your body out of the collapsed “defense posture’ and increases access to positive thoughts (Tsai et all, 2016; Peper et al., 2019)
B — Breathe
Allow your abdomen to expand as you inhale slowly and deeply. Let it get smaller as you exhale. Gently make a soft hissing sound as you exhale while helps the abdomen and pelvic floor to tighten. Then allow the abdomen to relax and widen which without effort draws the air in during inhalation. As you exhale, stay tall and imagine the air flowing through you and down your legs and out your feet.
C — Concentrate
Refocus your attention on what you want to do and add a gentle smile. This engages positive emotions, the smile helps downshift tension.
The video clip guides you through the ABCs process.
Integrate the breathing during the day by implementing your ABCs
When students practice relaxation technique and this method, they reported greater reductions in symptoms compared with a control group. By learning to notice tension and apply the ABC steps as soon as stress arises, they could shift their bodies and minds toward calm more quickly, as shown in Figure 4.
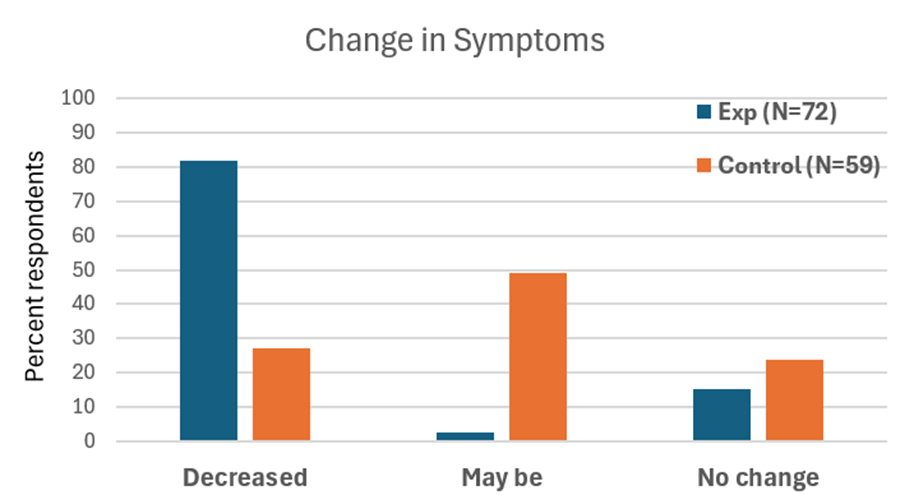
Figure 4. Change in symptoms after practicing a sequential relaxation and breathing techniques for four weeks.
Takeaway
Menstrual pain doesn’t have to be endured in silence or masked by medication alone. By practicing 30 minutes of slow diaphragmatic breathing daily and many times during the day, women may be able to reduce pain, stress, and discomfort — while building self-awareness and confidence in their body’s natural rhythms thereby having the opportunity to be more productive.
We recommend that schools and universities include self-care education—especially breathing and relaxation practices—as part of basic health curricula as this approach is scalable. Teaching young women to understand their bodies, manage stress, and talk openly about menstruation can profoundly improve well-being. It not only reduces physical discomfort but also helps dissolve the stigma that still surrounds this natural process,
Remember: Breathing is free—available anytime, anywhere and is helpful in reducing pain and discomfort. (Peper et al., 2025; Joseph et al., 2022)
See the following blogs for more in-depth information and practical tips on how to learn and apply diaphragmatic breathing:
REFERENCES
Itani, R., Soubra, L., Karout, S., Rahme, D., Karout, L., & Khojah, H.M.J. (2022). Primary Dysmenorrhea: Pathophysiology, Diagnosis, and Treatment Updates. Korean J Fam Med, 43(2), 101-108. https://doi.org/10.4082/kjfm.21.0103
Huang, G., Le, A. L., Goddard, Y., James, D., Thavorn, K., Payne, M., & Chen, I. (2022). A systematic review of the cost of chronic pelvic pain in women. Journal of Obstetrics and Gynaecology Canada, 44(3), 286–293.e3. https://doi.org/10.1016/j.jogc.2021.08.011
Joseph, A. E., Moman, R. N., Barman, R. A., Kleppel, D. J., Eberhart, N. D., Gerberi, D. J., Murad, M. H., & Hooten, W. M. (2022). Effects of slow deep breathing on acute clinical pain in adults: A systematic review and meta-analysis of randomized controlled trials. Journal of Evidence-Based Integrative Medicine, 27, 2515690X221078006. https://doi.org/10.1177/2515690X221078006
Peper, E., Booiman, A. & Harvey, R. (2025). Pain-There is Hope. Biofeedback, 53(1), 1-9. http://doi.org/10.5298/1081-5937-53.01.16
Peper, E., Chen, S., Heinz, N., & Harvey, R. (2023). Hope for menstrual cramps (dysmenorrhea) with breathing. Biofeedback, 51(2), 44–51. https://doi.org/10.5298/1081-5937-51.2.04
Peper, E., Harvey, R., Chen, S., & Heinz, N. (2025). Practicing diaphragmatic breathing reduces menstrual symptoms both during in-person and synchronous online teaching. Applied Psychophysiology and Biofeedback. Published online: 25 October 2025. https://rdcu.be/eMJqt https://doi.org/10.1007/s10484-025-09745-7
Peper, E., Harvey, R., & Hamiel, D. (2019). Transforming thoughts with postural awareness to increase therapeutic and teaching efficacy. NeuroRegulation, 6(3),153-169. https://doi.org/10.15540/nr.6.3.1533-1
Stroebel, C. (1982). The Quieting Reflex. New York: Putnam Pub Group. https://www.amazon.com/Qr-Quieting-Charles-M-D-Stroebel/dp/0399126570/
Thakur, P. & Pathania, A.R. (2022). Relief of dysmenorrhea – A review of different types of pharmacological and non-pharmacological treatments. MaterialsToday: Proceedings.18, Part 5, 1157-1162. https://doi.org/10.1016/j.matpr.2021.08.207
Tsai, H. Y., Peper, E., & Lin, I. M. (2016). EEG patterns under positive/negative body postures and emotion recall tasks. NeuroRegulation, 3(1), 23-27. https://doi.org/10.15540/nr.3.1.23
*Edited with the help of ChatGPT 5
The Power of No
Posted: March 6, 2025 Filed under: behavior, Breathing/respiration, CBT, cognitive behavior therapy, emotions, healing, health, self-healing, stress management, Uncategorized | Tags: assertiveness, emotional awareness, HIV, immune resilence, surviaval 1 CommentBrenda Stockdale, PhD and Erik Peper, PhD
Adapted from: Stockdale, B. & Peper, E. (2025). How the Power of No Supports Health and Healing. Townsend Letter-Innovative Health Perspectives, March15, 2025 https://townsendletter.com/the-power-of-no/

I felt exhausted and just wanted to withdraw to recharge. Just then, my partner asked me to go to the store to get some olive oil. I paused, took a deep breath, and checked in with myself. I realized that I needed to take care of myself. After a few seconds, I responded, “No, I cannot do it at this time.”
It was challenging to say this because, in the past, I would have automatically said “yes” to avoid disappointing my partner. However, by saying “yes” and ignoring my own needs, I would have become even more exhausted, hindering my recovery. I felt proud that I had said “no.” By listening to myself, I took charge and prioritized my own healing.
For many people, saying “no” feels unkind, and we want to be kind while avoiding burdening others. Nevertheless, how you answer this question may have implications for your health! Consider the following question and rate it on a scale from 1 (never) to 5 (always):
How often do you do favors for people when you really don’t want to? Namely, things you really don’t want to do but do anyway because someone asks you to and you don’t want to or can’t say “No.“
In analysis of numerous studies, Prof. George Solomon and Dr. Lydia Temoshok reported that a low score on this question (indicating the ability to say No) was the best predictor of related outcomes across studies, such as survivorship with AIDS as well as more favorable HIV immune measures (Solomon, et al, 1987). This aligns with research suggesting that excessive compliance, self-sacrifice, and conflict avoidance (i.e., people-pleasing) in individuals with cancer and chronic illness may weaken, rather than strengthen, their immune systems (Temoshok, & Dreher, 1992).
Unconsciously avoiding or suppressing distressing thoughts, emotions, or memories instead of dealing with them––a process known as repressive coping–– may even contribute to an increased risk of cancer and cardiovascular disease (Mund & Mitte, 2012). Avoiding emotional cues or dismissing feelings may seem self-protective but can lead to reflexive or automatic behavior such as saying “yes” when individuals would rather say “no.” Although the conflict may not be consciously recognized, it can manifest physiologically (Mund & Mitte, 2012). Paying attention to states of tension, or symptoms such as headache or loss of appetite can serve as a doorway to exploring unacknowledged feelings.
Automatically saying “yes” and sacrificing yourself may contribute to poor boundaries, leading to chronic stress which is linked to numerous health issues, including hypertension and immune dysfunction (Dai et al., 2020; Segerstrom et al., 2004; Deci & Ryan, 2008). Conversely, research indicates that individuals who assertively manage stress—rather than suppress emotions and avoid conflict—demonstrate stronger immune resilience (Ironson et al., 2005; Dantzer et al, 2018) and are better protected against burnout and prolonged emotional distress (Deci & Ryan, 2018).
When faced with illness––or even the possibly death––ask yourself: “Do I really want to do this, or am I doing it just to please my partner, children, parents, doctors, or society? By doing what truly brings me joy and meaning, what do I have to lose?” Altruism is valuable and an important part of maintaining health. At the same time boundaries and assertiveness are essential.
Psychologist Lawrence LeShan (1994) reported that when cancer patients began to seek and start singing their “own song,” their cancer regressed in numerous cases, and some experienced total remission. Living your own song means doing what you truly desire rather than following the expectations of parents, society, or economic pressures. It is important to keep in mind that while psychological factors can influence overall health, the development of cancer is a multifaceted process involving genetic, lifestyle and environmental factors.
The Key Question: When and How to Say “No”?
The answer lies in emotional awareness and acting on it. One woman with cancer confided, “I’ve operated in the realm of expected behavior for so long that I no longer know what I want or feel” (Stockdale, 2009). Teasing out our true feelings—hour by hour, as Bernie Siegel, M.D., recommends—helps us recognize where we stand (Siegel, 1986; Siegel & August, 2004). This practice fosters a sense of agency, a cornerstone of resilience that directly contributes to well-being.
For those accustomed to prioritizing others’ needs over their own, learning to say “No” takes practice. Although one may have feelings of vulnerability and even guilt by disappointing someone, one person shared that only after he stopped exclusively prioritizing others–and instead learned to love himself as well as his neighbor–did he realize how much people genuinely cared for him. Authentic connection is essential for well-being, but trust cannot develop without agency and the freedom to say “no.”
What to Do Before Automatically Saying Yes
When someone asks you for help or a favor, pause. Look up, take a slow, diaphragmatic breath, and ask yourself, “Do I want to do this? What would I recommend to another person to do in this situation?”
(In cases where you are asked or ordered to harm another person or do something illegally, ask yourself, “What would a moral person do?”)
If you feel that you would rather not—whether because you are tired or it interferes with your own priorities—say “No.” Saying “No” does not mean you are unwilling to help; it simply means that, at this moment, you are listening to yourself. When we listen to ourselves and act accordingly, we enhance our immune competence and self-healing.
Obviously, if saying “No” would put another person in danger or in crisis, then say “Yes,” if possible. However, true crises are rare. If emergencies happen frequently, they are not true crises or emergencies but rather a result of poor planning.
Saying “No” can be challenging, but if you constantly say “Yes,” you may eventually become resentful and exhausted, increasing your stress and decreasing your ability to heal. You may even notice that when your own well-being is appropriately prioritized you will be in a better position to show up for others in a whole-hearted way, when it is right for them and for you.
Saying “No” Can Be Life-Saving
Beyond personal relationships, saying “No” can be crucial in medical settings. Anthony Kaveh, M.D., a Stanford- and Harvard-trained anesthesiologist and integrative medicine specialist, asserts, “Nice patients come out last” (Kaveh, 2024). Kaveh emphasizes that trusting our instincts is crucial, as the fear of displeasing others can lead to dangerous “fake nice” behavior.
See the YouTube video #1 Mistake You Make with Doctors: Medical Secrets (https://www.youtube.com/watch?v=9-E3CHHX05c)
A case example is illustrated by Tracy who was hospitalized with complex fractures of the tibia and fibula. After five surgeries, she felt something was terribly wrong–she knew she was dying. However, the nurses dismissed her concerns. Taking control, she infuriated the staff by calling 911, which prompted a doctor to check on her. It was discovered that excessive negative pressure applied to the drain caused five pints of her blood to flow into her leg causing compartment syndrome.
She was bleeding to death. Tracy’s intuition, resilience, and refusal to comply saved her life. Kaveh argues that those who don’t trust their instincts are more likely to err on the side of “nice” and suffer as a result.
Learning to say “No” is empowering as illustrated by one woman who discovered its importance in a cancer educational group she attended. She shared her success in saying “No” with humor, explaining, “I just tell people it’s this group’s fault because I used to be a nice person.”
Learning to listen to yourself before agreeing or disagreeing to do something, may also help you maintain your integrity when faced with pressure to follow an immoral suggestion or order. So often due to social, economic, corporate, or political pressure, people may be asked to do something they later regret (Sah, 2025). The courage to disagree and act according to your moral consciousness is the bases of the Nuremberg Code, established by the American judges in 1947 at the Nuremberg trials for Nazi doctors (Shuster, 1997).
Finally, learning to say “No” and listen to your needs takes practice and time. Explore the following Body Dialogue technique to tap into your intuitive wisdom. You can use it anytime you need clarity about your feelings and responses to life’s challenges.
Breathe in deeply and engage all your senses. When you are ready, focus on the sensation of breathing. You don’t have to make anything happen, just feel the air moving in and out. Your lungs, vital to energy production, obtain oxygen from the atmosphere and bring it to millions of specialized cells. All without your conscious awareness, your breath moves in and out, removing toxins and waste from your body and bringing oxygen in.
The beautiful filtering process even protects your heart. That great organ, pumping rhythmically, picks up the oxygen and delivers it to all the vessels of your body, contracting more than two billion times during a normal lifespan. With deep appreciation for this magnificent pump, move your attention down into your abdomen. On the right side is the largest organ in your body, your liver. This amazing organ filters toxins and chemicals, and aids in digestion. This powerhouse of function can even regenerate itself after losing as much as three quarters of its tissue. With a sense of admiration, imagine all that these great and vital organs accomplish. With gratitude, slowly move on to your spleen, your pancreas and all the other organs and systems of your body, taking your time to appreciate and acknowledge all that they do for you.
Consider the multitude of vital functions that take place every minute of every day and thank your body for all that is right with you. All of these complex functions take place without effort or even awareness on your behalf––they just happen. Ask now if there something you can do for your body to help it heal, repair or regenerate more completely. Listen closely to your own intuitive awareness. Is there anything you can do to make your body’s job easier or reduce a burden of some kind? Gently notice if there are any thoughts or behaviors that make some symptoms worse or better. What feels heavy or burdensome? Who or what in your life feels supportive? As you review the past few days or weeks what would you like to adjust? When might saying ‘no’ would bring a sense of relief? Imagine what it would be like to operate in your own best interest. What might that include?
Are there positive feelings you would like to experience more often? If you had to choose just one, what would it be? In what way could you bring more of that quality into your life? In your mind’s eye, see that happening now. Feel the peace or the joy or whatever it is you have chosen radiate throughout your being. And if it seems good to you, carry it with you, back to the present moment and enjoy the fullness of that sensation. When it seems right to you, again focus gently on your body, bringing your attention back to the chair or the place you happen to be. And filled with gratitude, stretch your arms wide with appreciation for all that is right with you.
Additional useful blogs
References
Dai, S., Mo, Y., Wang, Y., Xiang, B., Liao, Q., Zhou, M., Li, X., Li, Y., Xiong, W., Li, G., Guo, C., & Zeng, Z. (2020). Chronic Stress Promotes Cancer Development. Frontiers in oncology, 10, 1492. https://doi.org/10.3389/fonc.2020.01492
Dantzer, R., Cohen, S., Russo, S. J., & Dinan, T. G. (2018). Resilience and immunity. Brain, behavior, and immunity, 74, 28–42. https://doi.org/10.1016/j.bbi.2018.08.010
Deci, E. L., & Ryan, R. M. (2008). Self-determination theory: A macrotheory of human motivation, development, and health. Canadian Psychology / Psychologie canadienne, 49(3), 182–185. https://doi.org/10.1037/a0012801
Deci, E. L., & Ryan, R. M. (2018). Self-determination theory: Basic psychological needs in motivation, development, and wellness. New York: Guilford Publications. https://www.amazon.com/Self-Determination-Theory-Psychological-Motivation-Development/dp/1462538967
Ironson, G., O’Cleirigh, C., Fletcher, M. A., Laurenceau, J. P., Balbin, E., Klimas, N., Schneiderman, N., & Solomon, G. (2005). Psychosocial factors predict CD4 and viral load change in men and women with human immunodeficiency virus in the era of highly active antiretroviral treatment. Psychosomatic medicine, 67(6), 1013–1021. https://doi.org/10.1097/01.psy.0000188569.58998.c8
Kaveh, A. (2024). #1 Mistake You Make With Doctors. Medical Secrets, YouTube, https://www.youtube.com/watch?v=9-E3CHHX05c
LeShan, L. (1994). Cancer As a Turning Point: A Handbook for People with Cancer, Their Families, and Health Professionals – Revised Edition. New York: Penguin Publishing Group. https://www.amazon.com/Cancer-As-Turning-Point-Professionals/dp/0452271371
Mund, M., & Mitte, K. (2012). The costs of repression: a meta-analysis on the relation between repressive coping and somatic diseases. Health psychology : official journal of the Division of Health Psychology, American Psychological Association, 31(5), 640–649. https://doi.org/10.1037/a0026257
Sah, S. (2025. Defy: The power of no in a world that demands yes. London: One World Publications. https://www.amazon.com/Defy-Power-World-That-Demands/dp/0593445775
Shuster, E. (1997). Fifty years later: The significance of the Nuremberg code. The New England Journal of Medicine, 337(20), 1436-1440. https://doi.org/10.1056/NEJM199711133372006
Segerstrom, S. C., & Miller, G. E. (2004). Psychological stress and the human immune system: a meta-analytic study of 30 years of inquiry. Psychological bulletin, 130(4), 601–630. https://doi.org/10.1037/0033-2909.130.4.601
Siegel, B. (1986). Love, medicine & miracles. New York: William Morrow Paperbacks; https://www.amazon.com/Love-Medicine-Miracles-Bernie-Siegel-dp-B00A2KKOBI
Siegel, B. & August, Y. (2004). Help Me Heal. Hay House. https://www.amazon.com/Help-Heal-Bernie-Siegel-M-D/dp/1401900607/
Solomon, G. F., Temoshok, L., O’Leary, A., & Zich, J. (1987). An intensive psychoimmunologic study of long-surviving persons with AIDS. Pilot work, background studies, hypotheses, and methods. Annals of the New York Academy of Sciences, 496, 647–655. https://doi.org/10.1111/j.1749-6632.1987.tb35825.x
Stockdale, B. (2009). You can beat the odds: Surprising factors behind chronic illness and cancer––the 6-week program for Optimal Immunity. Boulder, CO: Sentient Publications. https://www.amazon.com/You-Can-Beat-Odds-Surprising-ebook/dp/B00KMDKOVA
Temoshok L. (1987). Personality, coping style, emotion and cancer: towards an integrative model. Cancer surveys, 6(3), 545–567. https://pubmed.ncbi.nlm.nih.gov/3326661/
Temoshok, L., & Dreher, H. (1992). The type C connection: The behavioral links to cancer and immune dysfunction. New York: Random House. https://www.amazon.com/Type-Connection-Behavioral-Cancer-Health/dp/0394575237
Use the power of your mind to transform health and aging
Posted: February 18, 2025 Filed under: attention, behavior, cancer, CBT, cognitive behavior therapy, COVID, education, health, meditation, mindfulness, Pain/discomfort, placebo, stress management, Uncategorized | Tags: health, imimune function, longevity, mental-health, mind-body, nutrition, Reframing, wellness Leave a commentMost of the time when I drive or commute by BART, I listen to podcasts (e.g., Freakonomics, Hidden Brain, this podcast will kill you, Science VS, Huberman Lab). although many of the podcasts are highly informative; , rarely do I think that everyone could benefit from it. The recent podcast, Using your mind to control your health and longevity, is an exception. In this podcast, neuroscientist Andrew Huberman interviews Professor Ellen Langer. Although it is three hours and twenty-two minute long, every minute is worth it (just skip the advertisements by Huberman which interrupts the flow). Dr. Langer delves into how our thoughts, perceptions, and mindfulness practices can profoundly influence our physical well-being.
She presents compelling evidence that our mental states are intricately linked to our physical health. She discusses how our perceptions of time and control can significantly impact healing rates, hormonal balance, immune function, and overall longevity. By reframing our understanding of mindfulness—not merely as a meditative practice but as an active, moment-to-moment engagement with our environment—we can harness our mental faculties to foster better health outcomes. The episode also highlights practical applications of Dr. Langer’s research, offering insights into how adopting a mindful approach to daily life can lead to remarkable health benefits. By noticing new things and embracing uncertainty, individuals can break free from mindless routines, reduce stress, and enhance their overall quality of life. This podcast is a must-listen for anyone interested in the profound connection between mind and body. It provides valuable tools and perspectives for those seeking to take an active role in their health and well-being through the power of mindful thinking. It will change your perspective and improve your health. Listen to or watch the interview:
Youtube: https://www.youtube.com/watch?v=QYAgf_lfio4

Useful blogs to reduce stress
From Conflict to Calm: Reframing Stress and Finding Peace with Difficult People
Posted: February 6, 2025 Filed under: attention, behavior, Breathing/respiration, CBT, emotions, healing, health, Neck and shoulder discomfort, Pain/discomfort, stress management | Tags: anger, anger management, conflict resolution, Reframing, resentment 8 Comments
Adapted from: Peper, E. (2025, Feb 15). From Conflict to Calm: Reframing Stress and Finding Peace with Difficult People. Townsend Letter-Innovative Health Perspectives. https://townsendletter.com/from-conflict-to-calm-reframing-stress-and-finding-peace-with-difficult-people/
After living in our house for a few years, a new neighbor moved in next door. Within months, she accused us of moving things in her yard, blamed us when there was a leak in her house, dumped her leaves from her property onto other neighbors’ properties, and even screamed at her tenants to the extent that the police were called numerous times.
Just looking at her house through the window was enough to make my shoulders tighten and leave me feeling upset. When I drove home and saw her standing in front of her house, I would drive around the block one more time to avoid her while feeling my body contract. Often, when I woke up in the morning, I would already anticipate conflict with my neighbor. I would share stories of my disturbing neighbor and her antics with my friends. They were very supportive and agreed with me that she was crazy.
However, this did not resolve my anger, indignation, or the anxiety that was triggered whenever I saw her or thought of her. I spent far too much time anticipating and thinking about her, which resulted in tension in my own body—my heart rate would increase, and my neck and shoulders would tighten. I decided to change. I knew I could not change her; however, I could change my reactivity and perspective.
Thus, I practiced the “Pause and Recenter” technique described in the blog. At the first moment of awareness that I was thinking about her or her actions, I would change my posture by sitting up straight and looking upward, breathe lower and slower, and then, in my mind’s eye, send a thought of goodwill streaming to her like an ocean wave flowing through and around her in the distance. I choose to do this because I believe that within every person, no matter how crazy or cruel, there is a part that is good, and it is that part I want to support.
I repeated this many times—whenever I looked in the direction of her house or saw her in her yard. I also reframed her aggressive, negative behavior as her way of coping with her own demons. Three months later, I no longer react defensively. When I see her, I can say hello and discuss the weather without triggering my defensive reaction. I feel so much more at peace living where I am.
When stressed, angry, rejected, frustrated, or hurt, we so often blame the other person. The moment we think about that person or event, our anger, indignation, resentment, and frustration are triggered. We keep rehashing what happened. As we do this, we are unaware that we are reliving the past event and are often unaware of the harm we are doing to ourselves until we experience symptoms such as high blood pressure, gastrointestinal distress, insomnia, anxiety, or muscle tightness. As we think of the event or interact again with that person, our body automatically responds with a defense reaction as if we are actually being threatened. This response activates the defense to protect ourselves from harm— the person is not a threat like the saber-toothed tiger ready to attack. Yet we respond as if the person is the tiger.
This defense reaction activates our “fight or flight” responses and increases sympathetic activation so that we can run faster and fight more ferociously to survive; however, it reduces blood flow through the frontal cortex—a process that reduces our ability to think rationally (Willeumier, et al., 2011; van Dinther et al., 2024). When we become so upset and stressed that our mind is captured by the other person, it contributes to an increase in hypertension, myofascial pain, depression, insomnia, cardiovascular disease, and other chronic disorders (Russel et al., 2015; Suls, 2013; Duan et al., 2022).
Our initial response of sharing our frustrations with others is normal. It feels good to blame the other; however, over time, the only person who gets hurt is yourself (Fast & Tiedens, 2010; Lou et al., 2023). The time spent rehashing and justifying our feelings diminishes our time we are in the present moment or focus on upcoming opportunities.
We may not realize that we have a choice. We can keep living and reacting to past hurt or losses, or we can let go and/or forgive and make space for new opportunities. Although the choice is ours, it is often very challenging to implement—even with the best intentions—as we react automatically when reminded of the past hurt (seeing that person, anticipating meeting or actually meeting that person who caused the hurt, or being triggered by other events that evoke memories of the pain).
What can you do
If choose to change your response and reactivity, it does not mean you condone what happened or agree that the other person was right. You are just choosing to live your life and not continue to be captured and react to the previous triggers. Many people report that after implementing some of the practices described below or others stress management techniques frequently their automatic reactivity was significantly reduced. They report that their symptoms are reduced and have the freedom to live in present instead of being captured by the painful past.
Pause and recenter
Our automatic reaction to the trigger elicits a defense reaction that reduces our ability to think rationally. Therefore, the moment you anticipate or begin to react, take three very slow diaphragmatic breaths. As you inhale, allow your abdomen to expand; then, as you exhale slowlymake your yourself tall and look up. Looking up allows easier access to empowering and positive memories (Peper et al., 2017). Continue looking up and inhale slowly allow the abdomen to expand. Repeat this slow breath again.
On the third breath, while looking up, evoke a memory of someone in whose presence you felt at peace and who loves –you such as your grandmother, aunt or uncle or your dog. Reawaken that feeling associated with that memory. Allow a smile with soft eyes to come to your face as you experience the loving memory. Then, put your hands on your chest, take a breath as your abdomen to expands, and as you exhale, bring your hands away from your chest and stretch them out in front of you. At the same time, in your mind’s eye imagine sending good will to that person or conflict that previously evoked your stress response.
As you do this, you are not condoning what happened; instead, you are sending goodwill to that person’s positive aspect. From this perspective, everyone has an intrinsic component—however small—that some label as Christ nature or Buddha nature.
Why could this be effective? This practice short-circuits the automatic stress response and provides time to recenter. It interrupts ongoing rumination by shifting the mind away from thoughts about the person or event that induces stress and toward a positive memory. Evoking a loving memory from the past facilitates a reduction in arousal, evokes a positive mood, and decreases sympathetic nervous system activation (Speer & Delgado, 2017). Additionally, slower diaphragmatic breathing reduces sympathetic activation (Birdee et al., 2023; Siedlecki et al., 2022). By combining body and mind, we can pause and create the opportunity to respond positively rather than reacting with anger and hurt.
Practice sending goodwill the moment you wake up
So often when we wake up, we already anticipate the challenges and even the prospect of interacting with person or event heightens our defense reaction. Therefore, as soon as you wake up, sit at the edge of the bed, repeat the previous practice, Pause and Center. Then, as you sit at the edge of the bed, slightly smile with soft eyes, look up, inhale as your abdomen expand. Then, stamp your right foot into the floor while saying, “Today is a new day.” Next, inhale allowing your abdomen expand; as you look up, stamp your left foot on the floor while saying, “Today is a new day.” Finally, send goodwill to the person who previously triggered your defensive reaction.
Why could this be effective?
Looking up makes it easier to access positive memories and thoughts. Stamping your foot on the ground is a non-verbal expression of determination and anchors the thought of a new day, thereby focuses on new opportunities (Feldman, 2022).
Discuss your issue from the third-person perspective instead of the first-person perspective
When thinking, ruminating, talking, texting, or writing about the event, discuss it from the third-person perspective. Replace the first-person pronoun “I” with “she” or “he.” For example, instead of saying:
I was really pissed off when my boss criticized my work without giving any positive suggestions for improvement,
Say:
He was really pissed off when his boss criticized his work without offering any positive suggestions for improvement.
Why could this be effective? The act of substituting the third person pronoun for the first-person pronoun interrupts our automatic reactivity because it requires us to observe and change our language, which activating the frontal cortex. This process creates a psychological distance from our feelings, allowing for a more objective and calmer perspective on the situation. It effectively reducing stress by stepping back from the immediate emotional response (Moser et al., 2017). It means that you are no longer fully captured by the emotions, as you are simultaneously the observer of your own inner language and speech.
Compare yourself to others who are suffering more
When you feel sorry for yourself or hurt, take a breath, look upward, and compare yourself to others who are suffering much more. In that moment, consider yourself incredibly lucky compared to people enduring extreme poverty, bombings, or severe disfigurement. Be grateful for what you have.
Why could this be effective? The research data shows that if we have low self-esteem when we compare ourselves to people who are more successful (healthier, richer, or successful), we feel worse in comparison and if we compare ourselves to other who are suffering more we feel better (Aspinwall, & Taylor, 1993). The comparision relativize our suffering. Thus our own suffering become less significant compared to the other people’s severe suffering.
Research shows that when we compare ourselves to people who are more successful (healthier, richer, or more accomplished), we tend to feel worse—especially if we have low self-esteem. However, when we compare ourselves to others who are suffering more, we tend to feel better (Aspinwall, & Taylor, 1993). This comparison relativizes our suffering, making our own hardships and suffering seem less significant compared to the severe suffering of others.
Interrupt the stress response
When overwhelmed by a stress reaction, implement the recue techniques described in the article, Quick rescue techniques when stress (Peper, Oded and Harvey, 2024) and the blog to help reduce stress. https://peperperspective.com/2024/02/04/quick-rescue-techniques-when-stressed/
Conclusion
It is much easier to write and talk about these practices than to actually do them. Remembering and reminding yourself to implement them can be very challenging. It requires significant effort and commitment. In most cases, the benefits are not experienced immediately. However, when practiced many times over weeks and months, many people report feeling less resentment, experience a reduction in symptoms, and improvements in health and relationships.
*This blog was inspired by the podcast, No hard feelings, that featured psychologist Fred Luskin. It is an episode on Hidden Brain, produced by Shankar Vedantam (2025) and the wisdom taught by Dora Kunz (Kunz & Peper, 1983; Kunz and Peper, 1984a; Kunz and Peper, 1984b; Kunz and Peper, 1987).
Useful blog that complement the concepts in this blog
References
Aspinwall, L. G., & Taylor, S. E. (1993). Effects of social comparison direction, threat, and self-esteem on affect, self-evaluation, and expected success. Journal of Personality and Social Psychology, 64(5), 708–722. https://doi.org/10.1037/0022-3514.64.5.708
Birdee, G., Nelson, K., Wallston, K., Nian, H., Diedrich, A., Paranjape, S., Abraham, R., & Gamboa, A. (2023). Slow breathing for reducing stress: The effect of extending exhale. Complementary Therapies in Medicine, 73. https://doi.org/10.1016/j.ctim.2023.102937
Duan, S., Lawrence, A., Valmaggia, L., Moll, J. & Zahn, R. (2022). Maladaptive blame-related action tendencies are associated with vulnerability to major depressive disorder. Journal of Psychiatric Research, 145, 70-76. https://doi.org/10.1016/j.jpsychires.2021.11.043
Fast, N.J. & Tiedens, L.Z. (2010). Blame contagion: The automatic transmission of self-serving attributions. Journal of Experimental Social Psychology, 46(1), 97-106. https://doi.org/10.1016/j.jesp.2009.10.007
Feldman, Y. (2022). The Dialogical Dance-A Relational Embodied Approach to Supervision. In Butte, C. & Colbert, T. (Eds). Embodied Approaches to Supervision-The Listening Body. London: Routledge. https://www.amazon.com/Embodied-Approaches-Supervision-C%C3%A9line-Butt%C3%A9/dp/0367473348
Kunz, D. & Peper, E. (1983). Fields and Their Clinical Implications-Part III: Anger and How It Affects Human Interactions. The American Theosophist, 71(6), 199-203. https://www.researchgate.net/publication/280777019_Fields_and_their_clinical_implications-Part_III_Anger_and_how_it_affects_human_interactions
Kunz, D. & Peper, E. (1984a). Fields and Their Clinical Implications IV: Depression from the Energetic Perspective: Etiological Underpinnings. The American Theosophist, 72(8), 268-275. https://biofeedbackhealth.org/wp-content/uploads/2011/01/fields-and-their-clinical-implications-iv-depression-from-the-energetic-perspectivive.pdf
Kunz, D. & Peper, E. (1984b). Fields and Their Clinical Implications V: Depression from the Energetic Perspective: Treatment Strategies. The American Theosophist, 72(9), 299-306. https://biofeedbackhealth.org/wp-content/uploads/2011/01/fields-and-their-clinical-implications-part-v-depression-treatment-strategies.pdf
Kunz, D. & Peper, E. (1987). Resentment: A poisonous undercurrent. The Theosophical Research Journal. IV (3), 54-59. Also in: Cooperative Connection. IX (1), 1-5. https://www.researchgate.net/publication/387030905_Resentment_Continued_from_page_4
Lou, Y., Wang, T., Li, H., Hu, T. Y., & Xie, X. (2023). Blame others but hurt yourself: blaming or sympathetic attitudes toward victims of COVID-19 and how it alters one’s health status. Psychology & Health, 39(13), 1877–1898. https://doi.org/10.1080/08870446.2023.2269400
Moser, J. S., Dougherty, A., Mattson, W. I., Katz, B., Moran, T. P., Guevarra, D., Shablack, H., Ayduk, O., Jonides, J., Berman, M. G., & Kross, E. (2017). Third-person self-talk facilitates emotion regulation without engaging cognitive control: Converging evidence from ERP and fMRI. Scientific reports, 7(1), 4519. https://doi.org/10.1038/s41598-017-04047-3
Oneda, B., Ortega, K., Gusmão, J. et al. (2010). Sympathetic nerve activity is decreased during device-guided slow breathing. Hypertens Res, 33, 708–712. https://doi.org/10.1038/hr.2010.74
Peper, E., Oded, Y, & Harvey, R. (2024). Quick somatic rescue techniques when stressed. Biofeedback, 52(1), 18–26. https://doi.org/10.5298/982312
Peper, E., Lin, I-M., Harvey, R., & Perez, J. (2017). How posture affects memory recall and mood. Biofeedback.45 (2), 36-41. https://doi.org/10.5298/1081-5937-45.2.01
Russell, M. A., Smith, T. W., & Smyth, J. M. (2016). Anger Expression, Momentary Anger, and Symptom Severity in Patients with Chronic Disease. Annals of behavioral medicine : a publication of the Society of Behavioral Medicine, 50(2), 259–271. https://doi.org/10.1007/s12160-015-9747-7
Siedlecki, P., Ivanova, T.D., Shoemaker, J.K. et al. (2022). The effects of slow breathing on postural muscles during standing perturbations in young adults. Exp Brain Res, 240, 2623–2631. https://doi.org/10.1007/s00221-022-06437-0
Speer, M. & Delgado, M. (2017).Reminiscing about positive memories buffers acute stress responses. Nat Hum Behav 1, 0093 (2017). https://doi.org/10.1038/s41562-017-0093
Suls J. (2013). Anger and the heart: perspectives on cardiac risk, mechanisms and interventions. Progress in cardiovascular diseases, 55(6), 538–547. https://doi.org/10.1016/j.pcad.2013.03.002
van Dinther, M., Hooghiemstra, A. M., Bron, E. E., Versteeg, A., Leeuwis, A. E., Kalay, T., Moonen, J. E., Kuipers, S., Backes, W. H., Jansen, J. F. A., van Osch, M. J. P., Biessels, G. J., Staals, J., van Oostenbrugge, R. J., & Heart-Brain Connection consortium (2024). Lower cerebral blood flow predicts cognitive decline in patients with vascular cognitive impairment. Alzheimer’s & dementia : the journal of the Alzheimer’s Association, 20(1), 136–144. https://doi.org/10.1002/alz.13408
Vedantma, S. (2025). Hidden Brain episode, No hard feelings. Accessed February 5, 2025. https://hiddenbrain.org/podcast/no-hard-feelings/
Willeumier, K., Taylor, D. V., & Amen, D. G. (2011). Decreased cerebral blood flow in the limbic and prefrontal cortex using SPECT imaging in a cohort of completed suicides. Translational psychiatry, 1(8), e28. https://doi.org/10.1038/tp.2011.28
Suggestions for mastering and generalizing breathing skills
Posted: October 30, 2024 Filed under: attention, behavior, biofeedback, Breathing/respiration, CBT, cellphone, cognitive behavior therapy, emotions, ergonomics, healing, health, mindfulness, Neck and shoulder discomfort, Pain/discomfort, posture, relaxation, self-healing, stress management, Uncategorized | Tags: abdominal beathing, anxiety, diaphragmatic braething, health, hyperventilation, meditation, mental-health, mindfulness, mouth breathing, Toning 3 CommentsAdapted from: Peper, E., Oded, Y., Harvey, R., Hughes, P., Ingram, H., & Martinez, E. (2024). Breathing for health: Mastering and generalizing breathing skills. Townsend Letter-Innovative Health Perspectives. November 15, 2024. https://townsendletter.com/suggestions-for-mastering-and-generalizing-breathing-skills/

Breathing techniques are commonly employed with complimentary treatments, biofeedback, neurofeedback or adjunctive therapeutic strategies to reduce stress and symptoms associated with excessive sympathetic arousal such as anxiety, high blood pressure, insomnia, or gastrointestinal discomfort. Even though it seems so simple, some participants experience difficulty in mastering effortless breathing and/or transferring slow breathing skills into daily life. The purpose of this article is to describe: 1) factors that may interfere with learning slow diaphragmatic breathing (also called cadence or paced breathing, HRV or resonant frequency breathing along with other names), 2) challenges that may occur when learning diaphragmatic breathing, and 3) strategies to generalize the effortless breathing into daily life.
Background
A simple two-item to-do list could be: ‘Breathe in, breathe out.’ Simple things are not always easy to master. Mastering and implementing effortless ‘diaphragmatic’ or ‘abdominal belly’ breathing may be simple, yet not easy. Breathing is a dynamic process that involves the diaphragm, abdominal, pelvic floor and intercostal muscles that can include synchronizing the functions of the heart and lungs and may result in cardio-respiratory synchrony or coupling, as well as ‘heart-rate variability breathing training (Codrons et al., 2014; Dick et al., 2014; Elstad et al., 2018; Maric et al., 2020; Matic et al., 2020). Improving heart-rate variability is a useful approach to reduce symptoms of stress and promotes health and reduce anxiety, asthma, blood pressure, insomnia, gastrointestinal discomfort and many other symptoms associated with excessive sympathetic activity (Lehrer & Gevirtz, 2014; Xiao et al., 2017; Jerath et al., 2019; Chung et al., 2021; Magnon et al., 2021; Peper et al., 2022).
Breathing can be effortful and In some cases people have dysfunctional breathing patterns such as breath holding, rapid breathing (hyperventilation), shallow breathing and lack of abdominal movement. This usually occurs without awareness and may contribute to illness onset and maintenance. When participants learn and implement effortless breathing, symptoms often are reduced. For example, when college students are asked to practice effortless diaphragmatic breathing twenty-minutes a day for one week, as well as transform during the day dysfunction breathing patterns into diaphragmatic breathing, they report a reduction in shallow breathing, breath holding,, and a decrease of symptoms as shown in Fig 1 (Peper et al, 2022).

Figure 1. Percent of people who reported that their initial symptoms improved after practicing slow diaphragmatic breathing for twenty minutes per day over the course of a week (reproduced from: Peper et al, 2022).
Most students became aware of their dysfunctional breathing and substituted slow, diaphragmatic breathing whenever they realized they were under stress; however, some students had difficulty mastering ‘effortless’ (e.g., automated, non-volitional) slow, diaphragmatic breathing that allowed abdominal expansion during inhalation.
Among those had more difficulty, they tended to have almost no abdominal movement (expansion during inhalation and abdominal constriction during exhalation). They tended to breathe shallowly as well as quickly in their chest using the accessory muscles of breathing (sternocleidomastoid, pectoralis major and minor, serratus anterior, latissimus dorsi, and serratus posterior superior).
The lack of abdominal movement during breathing reduced the movement of lymph as well as venous blood return in the abdomen; since; the movement of the diaphragm (the expansion and constriction of the abdomen) acts a pump. Breathing predominantly in the chest may increase the risk of anxiety, neck, back and shoulder pain as well as increase abdominal discomfort, acid reflux, irritable bowel, dysmenorrhea and pelvic floor pain (Banushi et al., 2023; Salah et al., 2023; Peper & Cohen, 2017; Peper et al., 2017; Peper et al., 2020, Peper et al., 2023). Learning slow, diaphragmatic or effortless breathing at about six breaths per minute (resonant frequency ) is also an ‘active ingredient’ in heartrate variability (HRV) training (Steffen et al., 2017; Shaffer & Meehan, 2020).
1. Factors that interfere with slow, diaphragmatic breathing
Difficulty allowing the skeletal and visceral muscles in the abdomen to expand or constrict in ‘three-dimensions’ (e.g., all around you in 360 degrees) during inhalation or exhalation. Whereas internal factors under volitional control and will mediate breathing practices, external factors can restrict and moderate the movement of the muscles. For example:
Clothing restrictions (designer jeans syndrome). The clothing is too tight around the abdomen; thereby, the abdomen cannot expand (MacHose & Peper, 1991; Peper et al., 2016). An extreme example were the corsets worn in the late 19th century that was correlated with numerous illnesses.
Suggested solutions and recommendations: Explain the physiology of breathing and how breathing occurs by the diaphragmatic movement. Discuss how babies and dogs breathe when they are relaxed; namely, the predominant movement is in the abdomen while the chest is relaxed. This would also be true when a person is sitting or standing tall. Discuss what happens when the person is eating and feels full and how they feel better when they loosen their waist constriction. When their belt is loosened or the waist button of their pants is undone, they usually feel better.
Experiential practice. If the person is wearing a belt, have the person purposely tighten their belt so that the circumference of the stomach is made much smaller. If the person is not wearing a belt, have them circle their waist with their hands and compress it so that the abdomen can not expand. Have them compare breathing with the constricted waist versus when the belt is loosened and then describe what they experienced.
Most participants will feel it is easier to breathe and much more comfortable when the abdomen is not constricted.
Previous abdominal injury. When a person has had abdominal surgery (e.g., Cesarean section, appendectomy, hernia repair, or episiotomy), they unknowingly may have learned to avoid pain by not moving (relaxing or tensing) the abdomen muscles (Peper et al., 2015; Peper et al., 2016). Each time the abdomen expands or constricts, it would have pulled on the injured area or stitches that would have cause pain. The body immediately learns to limit movement in the affected area to avoid pain. The reduction in abdominal movement becomes the new normal ‘feeling’ of abdominal muscle inactivity and is integrated in all daily activities. This is a process known as ‘learned disuse’ (Taub et al., 2006). In some cases, learned disuse may be combined with fear that abdominal movement may cause harm or injury such as after having a kidney transplant. The reduction in abdominal movement induces shallow thoracic breathing which could increase the risk of anxiety and would reduce abdominal venous and lymph circulation that my interfere with the healing.
Suggested solutions and recommendations. Discuss the concept of learned disuse and have participant practice abdominal movement and lower and slower breathing.
Experiential practices: Practicing abdominal movements
Sit straight up and purposely exhale while pulling the abdomen in and upward and inhale while expanding the abdomen. Even with these instructions, some people may continue to breathe in their chest. To limit chest movement, have the person interlock their hands and bring them up to the ceiling while going back as far as possible. This would lock the shoulders and allows the abdomen to elongate and thereby increase the diaphragmatic movement by allowing the abdomen to expand. If people initially have held their abdomen chronically tight then the initial expansion of abdomen by relaxing those muscle occurs with staccato movement. When the person becomes more skilled relaxing the abdominal muscles during inhalation the movement becomes smoother.
Make a “psssssst” sound while exhaling. Sit tall and erect and slightly pull in and up the abdominal wall and feel the anus tightening (pulling the pelvic floor up) while making the sound. Then allow inhalation to occur by relaxing the stomach and feeling the anus go down.
Use your hands as feedback. Sit up straight, placing one hand on the chest and another on the abdomen. While breathing feel the expansion of the abdomen and the contraction of the abdomen during exhalation. Use a mirror to monitor the chest-muscle movement to ensure there is limited rising and falling in this area.
Observe the effect of collapsed sitting. When sitting with the lower back curled, there is limited movement in the lower abdomen (between the pubic region and the umbilicus/belly button) and the breathing movement is shallower without any lower pelvic involvement (Kang et al., 2016). This is a common position of people who are working at their computer or looking at their cellphone.
Experiential practice: looking at your cellphone
Sit in a collapsed position and look down at your cellphone. Look at the screen and text as quickly as possible.
Compare this to sitting up and then lift the cell phone at eye level while looking straight ahead at the cellphone. Look at the screen and text as quickly as possible.
Observe how the position effected your breathing and peripheral awareness. Most likely, your experience is similar those reported by students. Close to 85%% of students who complete this activity reported that their breathing was shallower sitting slouched versus erect and about 85% of the students reported that their peripheral awareness and vision improved when sitting erect (Peper et al., 2024).
Suggested solutions and recommendations. Be aware how posture affect breathing. While sitting, place a rolled-up towel against the lower back so that the person sits more erect which would allow the abdomen to expand when inhaling.
Self-image, self-esteem, and confidence. Participants may hold their abdomen in because they want to look slim (sometimes labeled as the “hourglass syndrome” associate expanding the abdomen as unattractive (PTI, 2023). A flat abdomen is culturally reinforced by social media and fashion models and encouraged in some activities such as ballet. On the other hand, some people purposely puff up their chest to increase size and dominance (Cohen & Leung, 2009).
Suggested solutions and recommendations. Discuss the benefits of diaphragmatic breathing including its ability to reduce anxiety in social settings that may enhance confidence. Similar to an earlier suggestion, have the person explore clothing with a looser waist that still supports feelings of attractiveness and power.
Feeling anxious, fearful or threatened. The normal physiological stress reaction is a slight gasp with the tightening of the abdomen muscles for protection when a stressor occurs (Gilbert, 1998; Ekerholt & Bergland., 2008). The stressor can be an actual physical event, social situation or thoughts and emotions. Shallow breathing is a natural self-protective response. This pattern is often maintained until one feels ‘safe’ enough to relax, which for many can have a duration of the entire day or until finding the relative safety of sleep.
Suggested solutions and recommendations. Discuss how the physiological stress reaction is a normal response pattern that the person most likely learned in early childhood for self-protection. This pattern is often observed in clients who are emotionally sensitive and/or react excessively to a variety of stimuli. Note that some people have learned not to show their reactivity on their face or in the overt behaviors, yet they continue to breathe shallowly as a telltale sign of ‘distress.’ People who breath shallowly may experience this response as burdensome. Discuss with them how to reframe their sensitivity as a gift; namely, they are more aware of other people’s reactions and emotions. They just need to learn how not to respond automatically. Encourage awareness of their breath-holding and shallow breathing. Follow this by teaching them to replace the dysfunctional breathing with slow, diaphragmatic breathing at 6-breaths-per-minute. A possible training sequence is the following:
- Teach slow, diaphragmatic breathing
- Practice evoking a stressor and the moment the client senses the stress response, shallow breaths or holds their breath have them shift to slow, diaphragmatic breathing.
- If the person slouches in response to stress, the moment they become aware of slouching, have then sit erect, look up and then breathe diaphragmatically. (Peper et al., 2019)
Experiential practice: Transform stressful thoughts by looking up, breathing, and changing thoughts.
Evoke a stressor and then attempt to reframe the experience (cognitive behavior therapy or CBT approach).
Compare this to evoking a stressor, then shift to an upright position while looking up, take a few slow, diaphragmatic breaths, and reframe the experience.
In almost all cases, when the client shifts position, looks up and then reframes, the stress reaction is significantly reduced and it is much easier to reframe the experiences positively compared to when only attempting to reframe the experience (Peper et al., 2019).
Diaphragmatic breathing feels abnormal. How you breathe habitually is what feels normal unless there is overt illness such as asthma or emphysema. Any new pattern usually feels abnormal. When the person shifts their breathing pattern, such as in a transition from habitual shallow chest breathing to slower diaphragmatic abdominal breathing, it feels strange and wrong.
Suggested solutions and recommendations. Discuss the concept that habitual patterns are normal (e.g., a person who typically slouches when standing straight may experience that they are going to fall backwards). Emphasize the importance of making a shift in posture and leaning into the discomfort of the new experience. Often after practicing slow diaphragmatic breathing, the person may report feeling much more relaxed (e.g., sensing heaviness and warmth) with their fingers increasing in temperature.
2. Challenges that may occur when learning diaphragmatic breathing
Ideally, breathing is an effortless diaphragmatic process as described by the phrase, “it breathes me” (Luthe & Schultz, 1970; Luthe, 1979); however, some participants struggle to achieve this type of breathing. The following are common challenges and possible solutions:
Distraction and internal dialogue. Many people struggle with thoughts jumping from one area to another. Some people refer to this mental state as “monkey mind.”
Suggested solutions and recommendations. Validate that distraction and internal dialogue are normal and require continual managing and practice to overcome. Experimental Practice: Have the person train focus during diaphragmatic breathing techniques by focusing on 1 item in the room. Remind them that when thoughts arise, note them briefly instead of engaging with them and then refocus on the item. Start with increments of time and increase with practice.
Effect of gravity on breathing. In the vertical position, exhalation occurs when the abdomen constricts (slight tightening of the transverse and oblique abdominal muscles and the pelvic floor) pushes the diaphragm up, allowing the air to go out. It needs to push against gravity.
In the vertical position, inhalation occurs when the abdominal muscles and pelvic floor muscles relax and the abdomen widens in all directions (360 degrees) which causes the diaphragm to descend as it is being pulled down by gravity. This process allows effortless inhalation. The experience is the opposite when lying supine on one’s back. While lying down, gravity pulls on the abdomen that cause the diaphragm to go upward allowing the air to flow out during exhalation. Inhalation takes work because as the diaphragm descends it has to push the abdominal content upward against gravity.
Experiential practice: Erect versus supine
- Vertical position. Begin by exhaling completely by pulling the abdomen in and up while staying erect and not pressing/contracting the chest downward. At the end of exhalation, allow the abdomen to relax (pop out) and feel how the air is sucked in without trying to inhale
- Horizontal position. Begin by lying down, with the face pointing up. Inhale by expanding your abdomen and pushing your abdomen upward against gravity. Then let exhalation occur while totally relaxing as gravity pushes the abdomen downward, which pushes the diaphragm upward into the chest allowing the air to flow out. Optionally, place a small bag of rice/beans (e.g., approximately one to five pound or. One-half to two kilograms) on your lower abdomen while lying down. When you inhale, push the weight upward and away from you by allowing the stomach, but not the chest, to expand. Allow exhalation to occur as the weight pushes your abdomen down and upward into your chest. The weight is useful as it allows the mind to focus more easily on the task of feeling the movement of the abdomen.
Over breathing/hyperventilation. Even breathing at about six breaths per minute can cause hyperventilation can occur. Hyperventilation occurs when a person is breathing in excess of the metabolic needs of the body and thereby eliminating more carbon dioxide. The result is respiratory alkalosis and an elevated blood pH as the dissolved carbon dioxide (pCO2) in the blood is reduced (Folgering, 1999).
The most common symptoms of over breathing are colder sweaty hands and light-headedness. If this starts to occur, focus on decreasing the airflow during exhalation by exhaling through pursed lips making the sound, “Pssssssst.” While making this sound, make the sound softer with less airflow. Alternatively, have them imagine a holding a dandelion flower a few inches from their lips and blow so softly the seeds do not blow away. The blowing away of the seed is the feedback that you are blowing to hard as shown in Figure 2.

Figure 2. Dandelion seeds as feedback when the person is blowing with too much effort. Alternatively, we recommend that the client imagine smelling the scent/fragrance of a flower that usually causes nose inhalation and then exhale gently through pursed lips ast if the air flows over a candle and, the flame does not move back and forth.
Mouth breathing. Mouth breathing contributes to disturbed sleep, snoring, sleep apnea, dry mouth upon waking, fatigue, allergies, ear infections, attention deficit disorders, crowded miss-aligned teeth, and poorer quality of life (Kahn & Ehrlich, 2018). Even the risk of ear infections in children is 2.4 time higher for mouth breathers than nasal breathers (van Bon et al, 1989) and nine and ten year old children who mouth breath have significantly poorer quality of life and have higher use of medications (Leal et al, 2016).
Breathing through the nose is associated with deeper and slower breathing rate than mouth breathing. Nose breathing reduces airway irritation since the nose filters, humidifies, warms/cools the inhaled air as well as reduces the air turbulence in the upper airways. The epithelial cells of the nasal cavities produce nitric oxide that are carried into the lungs when inhaling during nasal breathing (Lundberg & Weitzberg, 1999). The nitric oxide contributes to healthy respiratory function by promoting vasodilation, aiding in airway clearance, exerting antimicrobial effects, and regulating inflammation (McKeown, 2019; Allen, 2024). Note that alternate nostril breathing, such as breathing in one nostril for 5-seconds and out of the other for 5-seconds is another technique which some people find beneficial.
Slower breathing approaches also facilitates sympathetic parasympathetic balance and reduces airway irritation. If the person breathes habitually through their mouth, refer them to health care provider to explore factors that may contribute to mouth breathing such as enlarged tonsils and adenoids or deviated septum. In addition, explore environmental factors that could contribute nasal inflammation such as allergies or foods such as dairy (Al-Raby, 2016).
Performance anxiety. Many participants are concerned about their performance. The direct instructions such as “follow the graphic” causes the person to try hard to breathe with too much effort. Explore some of the following indirect strategies to interrupt ongoing cognitive judgements and self-talk.
- Toning or humming (Peper et al., 2019a). While exhaling, have the person hum a sound with their mouth closed. Let the sound go for about 6 seconds, relax, inhale and hum again. Toning is very similar except you verbalize a tone such as “Oammm.” (For detailed instructions on toning, see: Anziani & Peper (2021)).
- Stroking down arms and legs during exhalation. Have a partner gently stroke down your arms from your shoulder past your fingertips as you are exhaling. The downward stroking is in rhythm with the exhalation. As the arm is being stroked, attend to the sensations going down the arms. Be sure that the toucher exhales at the same time and the stroking down the arm takes about six seconds. After being stroked for a few times, have the person imagine that each time they exhale they feel a flow down through their arms and out their fingers.
- Repeat the same process while stroking down the legs from the side of their hips to their toes.
- Finally, have the person imagine/feel the sensation streaming down their legs with each exhalation.
- Many participants will report that they sense a steaming going down their arms, that they hands warm up, and their thought have stopped.
- Integrated body movement with breathing especially flexion and contraction (Meehan & Shaffer, 2023). Integrate the normal response of flexion that induces exhalation and extension evokes inhalation. Be careful that the flexion movement does not encourage participants to compress their chest during exhalation, which tends to encourage chest breathing. Have the person focus on their head staying tall and erect. Have the person sit straight up with their feet slight apart and their hands palm down on their lap. Allow inhaling to initiate as the person simultaneously arches their lower back expanding the stomach, separating the knees and turning the hands palm up. Initiate exhalation while simultaneously bringing the knees together, turning the palms face down on the thighs and rolling the pelvic back slightly rounding the lower back. Do the movements smoothly while keeping the legs and shoulders relaxed.
Flooded by emotions. Although very rare, at times when the person allows the abdomen to relax, they may experience by the emotions from a past trauma as the habitual bracing patterns are relaxed.
Suggested solutions and recommendations. Validate these emotions for the person. Explain that this is a normal process that may occur if past trauma has occurred. Clients who have had past trauma often experience hypervigilance, which may interfere with the relaxation response that occurs during more optimal states of breathing. Transitioning to a more optimal rest state may be uncomfortable for a person who has experienced trauma because it reduces hypervigilance. This can feel uncomfortable as hypervigilance in these cases serves a protective role, even if it is an illusory feeling of protection from future harm. Since persistent hypervigilance can interfere with the relaxation response, the benefits of allowing a relaxation response to occur through slower breathing should be highlighted. Grounding techniques as described by Peper et al (2024a) can be useful to become centered.
3. Strategies to generalize the effortless breathing into daily life.
Generalizing the skill occurs after having mastered diaphragmatic breathing in different positions (sitting, standing, lying down, and while performing tasks). It is important to remember that our breathing patterns are conditioned with our behavior. Become aware how breathing affects cognitions and emotions and how emotions and cognitions affects breathing. The following are some strategies that may facilitate learning and generalizing the slower breathing skills.
Observing how our behavior affects our breathing: Anything that may evoke the alarm or defense reaction tends to cause the person gasp and/or hold their breath. For example, when a person is sitting peacefully, make an unexpected noise behind their back or movement in their periphery of vision. In most cases they will gasp or hold their breath. Usually, they are unaware of this process unless they are asked what happened to their breathing. The major reason for the breath holding is that the stimuli triggers an alarm/defense reaction and when we hold our breath our hearing is more acute (we can hear approaching danger earlier). The problem is that we give this response when there is no actual, immediate or present threat.
Experiential practice. Sit comfortably. Now as quickly as possible without rotating the head, look with your eyes to the extreme right and then left and back and forth as if trying to identify danger at the periphery. Do this for a few eye movements. Almost everyone holds their breath when doing this exercise. For generalizing the skill, ask the person to observe during the day situations in which they hold their breath, ask them if it was necessary and encourage them to start diaphragmatic breathing.
Observing how breathing affects our thoughts and emotions. Breathing patterns are intrinsically linked to our emotions and thoughts as illustrated in the many language phrases such as sigh of relief, full of hot air, waiting with bated breath. At the same time, our breathing patterns also affect our thoughts. For instance, when we breathe shallowly and more rapidly, we can induce feelings of fear or anxiety. If we gasp, we can experience thought stopping.
Experiential practices: Incomplete exhalation: Observe what happens when you exhale less than you inhale. Begin by exhaling only 70% of the air you inhaled, then inhale and exhale again only 70% of the air you just inhaled continue this for 30 seconds. Many people will experience the onset of anxiety symptoms, lightheadedness, dizziness, neck and shoulder tension, etc. (Peper & MacHose, 1993). If you experience symptoms during this exercise and you have experienced these symptoms in the past, it is likely that unknowingly breathing in a dysfunctional pattern could have evoked them. Therefore, practicing effortless breathing may interrupt and reduce the symptoms. Do this practice while observing the person carefully and immediately interrupt and distract the person if they start feeling dizzy, too anxious, or trigger the beginning of a panic attack or PTSD symptoms.
Experiential practice: Gasp or sniff-hold sniff. Observe what happens when you are performing a cognitive task and you rapidly gasp or do sniff-hold-sniff again before exhaling. Begin by sequentially subtracting mentally, the number 7 from 146 (e.g., 146, 139, 132….). Do this as rapidly as possible and do not make a mistake. While doing the subtracting, take a rapid gasp (such as one is triggered by surprise or fear), alternatively, take a quick sniff through your nose, hold your breath and take another sniff on top of the first one, then exhale. Whereas subtrating numbers is a skill most adults can perform, the ‘time pressure’ along with the direction to avoid mistakes may be the ‘immediate’ source of strain. Whether it was the time pressure, the direction to avoid mistakes or the direction to gasp, observe what happened to your thinking process. In almost all cases, your higher-order thoughts (doing the sequential subtraction under time pressure while gasping) have disappeared, replaced by the immediate thoughts of ‘performance anxiety.’
If you blank out on exams or experience anxiety, gasping and breath holding may be one of the factors that increases symptoms and affects your performance. If you are aware that you are holding your breath or gasped, use that as the cue to shift to slow diaphragmatic breathing and you may find that your performance improves. Therefore, observe when and where you were blanking out, gasping and/or holding your breathing then substitute slow, effortless diaphragmatic breathing.
How to develop awareness and interrupting of dysfunctional breathing response. Most participants are unaware of their somatic responses until symptoms occur. Being aware of the initiation of a somatic response may assist you in identifying triggers and interrupting the developing process. A significant component of the training is symptom prescription rehearsal.
Symptom prescription is a practice in which the participant simulates/acts out the psychophysiological pattern associated with their symptoms. They amplify the body pattern until they feel the onset of the actual symptoms. The moment the person feels the beginning of the symptom, they stop the practice and initiate slow breathing and relaxation. After practicing the symptom rehearsal, they are instructed to become aware of the onset of the symptom and then use that signal to trigger the effortless breathing while looking up and shifting the body into an upright sitting position (Peper et al., 2019). Gasping and breath holding are normal responses to unexpected stimuli; however, they may trigger sympathetic activation even when there is no actual danger.
Experiential practice: Developing awareness on neck and shoulder tension:
Sit comfortably and practice effortless breathing for a minute. Take a fearful gasp and observe what happens in your body (e.g., slight neck and upper chest tension, light headedness, slight radiating pain into the eye, etc.). Shift back to effortless breathing until all symptoms /sensations have disappeared.
- Now gasp with less effort and observe the first sensations, use the awareness of first sensations to trigger the effortless breathing and continue to breathe until symptoms have disappeared
- Continue this practice. Reduce the gasping effort each time.
- After having developed the initial somatic sensation then during the day observe what triggers this response and immediately shift to slower diaphragmatic breathing. After you have shifted to effortless breathing, reflect on the trigger. Was it necessary to react? If yes, explore strategies to resolve the issue.
The same process can be done to assist with desensitization to painful memories or stressful events. Each time the person becomes aware of their somatic reaction to an evoked memory or stressful event, they shift to effortless diaphragmatic breathing. If they find that it is difficult to interrupt the emotional memories and it triggers more and more negative thoughts and associations, use the sniff-hold-sniff technique and follow that with box-breathing or any of the other quick somatic rescue techniques (Peper et al., 2024a). Box-breathing in this context could include a brief breath-holding. A typical box-breathing technique is to breath in for a count of four, hold for a count of four, breath out for a count of four, then breath in again for a count of four, continuing the figurative 4-4-4-4 count of breathing.
Practice slower diaphragmatic breathing during the day. Implement effortless diaphragmatic breathing through regeneration and interrupting the stress response.
- Support regeneration. Each day set aside 10 to 20 minutes to practice slow effortless diaphragmatic breathing at about 6-breaths-per-minute. In the beginning 10 to 20 minutes may be too long, thus in some cases have the person practice a few times a day for two minutes and slowly build up to 10 or more minutes. The practice is not just a mechanical process of breathing it includes mindfulness training. Namely, as you are breathing each time you exhale imagine a flow doing down your arms and legs and as you inhale an energy coming into you. Whenever your attention drifts bring it back to the breathing.
- Integrate breathing with daily activities. Practice slower breather before eating, after putting the seat belt on in the car, or whenever a notification pops up on the cell phone.
- Set reminders and alarms on your phone to check how you are feeling and breathing. Leave notes on nearby furniture such as a nightstand, on the shower door, and/or on the kitchen table as reminders to be mindful of your breath. If stressed or breathing shallowly, take a moment to breathe slowly.
- Interrupt the stress response. During the day when you are aware that you shallow breathe, are holding your breath, feel anxious, experience neck and shoulder tightness, or worry and use that as a cue to shift position by sitting or standing more erect, looking upward and take a few slow diaphragmatic breaths.
- Use cue condition to facilitate this process. Each time you begin the practice smell a specific aroma or do some behavioral movement and then do the breathing. After a while the aroma or behavioral movement will become the classically conditioned cue to trigger the effortless breathing.
- Use role rehearsal and conditioning to generalize the skill. Generalizing the skills often takes more time than what may be expected. In a culture where instant relief is expected— implied message associated with medication— self-mastery techniques are different and challenging as they take time to master the skill and implement them during daily life. The process of mastery is similar to learning to play a musical instrument or sports. Learning to play the violin requires practice as well as practice with failures along the way until one is ready for more challenging musical pieces, recitals, or performances.
A useful strategy to implement the learning is role rehearsal in the office, at home at work, and in real life. It is usually much easier to practice these skills in a safe space such as your own room or, with a therapist compared to with other people or, at work. To generalize the skill most efficiently, it can be helpful to practice in a safe environment while imagining being in the actual stressful location This process is illustrated by the strategy to reduce social anxiety and menstrual cramps.
Social anxiety when seeing my supervisor. Master effortless breathing in a safe environment. Role rehearsal in imagery. If you observed that you held your breath when your supervisor is around, begin with imagery when your supervisor is not present. Sit, comfortably. Let go of muscle tension and breathe effortlessly, evoking a scenario where your supervisor is walking by and continue to breathe slowly as you imagine the scene. Role rehearsal in action. Ask another person to role-play your supervisor. Sit, comfortably. Let go of muscle tension and breathe effortlessly. Have this person walk into the room in a similar way that your supervisor would. Imagine that person is your supervisor while practicing your effortless breathing. Repeat until the effortless breathing is more automatic. Practice many times in real life. Whenever the rehearsed situation occurs, implement slower paced breathing.
Menstrual cramps that causes most women to curl up and breathe shallowly when experiencing menstrual cramps (Peper et al., 2023). Master effortless breathing in a safe environment. Practice breathing lying down. While lying down, breathe diaphragmatically by having a three-to-five-pound weight such as a bag of rice or hot water pad on your abdomen. If you have a partner, have the person stroke your legs from the abdomen to your toes while you exhale. Role rehearse experiencing pain and then practice lower diaphragmatic breathing. Namely, tighten your abdomen as if you have discomfort, then focus on relaxing the buttocks and sensing the air flowing down your legs and out your feet as you exhale. Practice in real life. A few days before you expected menstruation, practice slow diaphragmatic breathing several times for at least 5-10 minutes during the day. When your menstruation starts practice the slower and lower breathing while imagining the air flowing down the abdomen, through the legs and out the feet.
Summary/Conclusion
Breathing is the mind-body bridge. It usually occurs without awareness and breathing changes affect our thought, emotions and body. Mastering and implementing slower breathing during the day takes time and practice. By observing when breathing patterns change, participants may identify internal and external factors that affect breathing which provides an opportunity to implement effortless diaphragmatic breathing to optimize health as well as resolve some of the triggers. As one 20-year-old, female student reported,
The biggest benefit from learning diaphragmatic breathing was that it gave me the feeling of safety in many moments. My anxiety tended to make me feel unsafe in many situations but homing in and mastering diaphragmatic breathing helped tremendously. I shifted from constant chest breathing to acknowledging it and in turn, reminding myself to breathe with my diaphragm.
References
Allen, R. (2024). The health benefits of nose breathing. Nursing in General Practice. http://hdl.handle.net/10147/559021
Al-Rabia, M.W. (2016). Food-induced immunoglobulin E-mediated allergic rhinitis. J Microsc Ultrastruct, 4(2), 69-75. https://doi.org/doi.org/10.1016/j.jmau.2015.11.004
Anziani, M. & Peper, E. (2021). Healing from paralysis-Music (toning) to activate health. Peperperspective –ideas on illness, health and well-being from Erik Peper. Accessed April 16, 2024. https://peperperspective.com/2021/11/22/healing-from-paralysis-music-toning-to-activate-health/
Banushi, B., Brendle, M., Ragnhildstveit, A., Murphy, T., Moore, C., Egberts, J., & Robison, R. (2023). Breathwork Interventions for Adults with Clinically Diagnosed Anxiety Disorders: A Scoping Review. Brain Sci. 13(2), 256. https://doi.org/10.3390/brainsci13020256
Chung, A.H., Gevirtz, R.N., Gharbo, R.S. et al. (2021).Pilot Study on Reducing Symptoms of Anxiety with a Heart Rate Variability Biofeedback Wearable and Remote Stress Management Coach. Appl Psychophysiol Biofeedback 46, 347–358. https://doi.org/10.1007/s10484-021-09519-x
Cohen, D. & Leung, A.K.Y. (2009). The hard embodiment of culture. European Journal of Social Psychology, 9, 1278–1289 https://doi.org/10.1002/ejsp.671
Codrons, E., Bernardi, N. F., Vandoni, M., & Bernardi, L. (2014). Spontaneous group synchronization of movements and respiratory rhythms. PloS one, 9(9), e107538. https://doi.org/10.1371/journal.pone.0107538
Dick, T. E., Mims, J. R., Hsieh, Y. H., Morris, K. F., & Wehrwein, E. A. (2014). Increased cardio-respiratory coupling evoked by slow deep breathing can persist in normal humans. Respiratory physiology & neurobiology, 204, 99-111. https://doil.org/10.1016/j.resp.2014.09.013
Ekerholt, K. & Bergland, A. (2008). Breathing: A sign of life and a unique area for reflection and action. Physical therapy, 88(7), 832-840. https://doi.org/10.2522/ptj.20070316
Elstad, M., O’Callaghan, E. L., Smith, A. J., Ben-Tal, A., & Ramchandra, R. (2018). Cardiorespiratory interactions in humans and animals: rhythms for life. American Journal of Physiology-Heart and Circulatory Physiology, 315(1), H6-H17. https://doi.org/10.1152/ajpheart.00701.2017
Folgering, H. (1999). The pathophysiology of hyperventilation syndrome. Monaldi Arch Chest Dis, 54(4), 365-72. https://pubmed.ncbi.nlm.nih.gov/10546483/
Gilbert, C. (1998). Emotional sources of dysfunctional breathing. Journal of bodywork and movement therapies, 2(4), 224-23. https://doi.org/10.1016/S1360-8592(98)80019-3
Jerath, R., Beveridge, C., & Barnes, V.A. (2019). Self-Regulation of Breathing as an Adjunctive Treatment of Insomnia. Front Psychiatry, 9(780). https://doi.org/10.3389/fpsyt.2018.00780
Kahn, S. & Ehrlich, P.R. (2018). Jaws. Stanford, CA: Stanford University Press. https://www.amazon.com/Jaws-Hidden-Epidemic-Sandra-Kahn/dp/1503604136/ref=tmm_hrd_swatch_0?_encoding=UTF8&qid=1685135054&sr=1-1
Kang, K.W., Jung, S.I., Lee, do Y., Kim, K., & Lee, N.K. (2016) Effect of sitting posture on respiratory function while using a smartphone. J Phys Ther Sci, 28(5), 1496-8. https://doi.org/10.1589/jpts.28.1496
Leal, R.B., Gomes, M.C., Granville-Garcia, A.F., Goes, P.S.A., & de Menezes, V.A. (2016). Impact of Breathing Patterns on the Quality of Life of 9- to 10-year-old Schoolchildren. American Journal of Rhinology & Allergy, 30(5):e147-e152. https://doi.org/10.2500/ajra.2016.30.4363
Lehrer, P.M. & Gevirtz, R. (2014). Heart rate variability biofeedback: how and why does it work? Front Psychol. 5, 756. https://doi.org/10.3389/fpsyg.2014.00756
Lundberg, J.O. & Weitzberg, E. (1999). Nasal nitric oxide in man. Thorax. (10):947-52. https://doi.org/10.1136/thx.54.10.947
Luthe, W. (1979). About the Methods of Autogenic Therapy. In: Peper, E., Ancoli, S., Quinn, M. (eds). Mind/Body Integration. Springer, Boston, MA. https://doi.org/10.1007/978-1-4613-2898-8_12
Luthe, W. & Schultz, J. H. (1970). Autogenic therapy: Medical applications. New York: Grune and Stratton. https://www.amazon.com/Autogenic-Therapy-II-Medical-Applications/dp/B001J9W7L6
MacHose, M., & Peper, E. (1991). The effect of clothing on inhalation volume. Biofeedback and Self-Regulation, 16(3), 261–265. https://doi.org/10.1007/BF01000020
Magnon. V., Dutheil, F., & Vallet, G.T. (2021). Benefits from one session of deep and slow breathing on vagal tone and anxiety in young and older adults. Sci Rep. 11(1),19267. https://doi.org/10.1038/s41598-021-98736-9
Maric, V., Ramanathan, D., & Mishra, J. (2020). Respiratory regulation & interactions with neuro-cognitive circuitry. Neuroscience & Biobehavioral Reviews, 112, 95-106. https://doi.org/10.1016/j.neubiorev.2020.02.001
Matić, Z., Platiša, M. M., Kalauzi, A., & Bojić, T. (2020). Slow 0.1 Hz breathing and body posture induced perturbations of RRI and respiratory signal complexity and cardiorespiratory coupling. Frontiers in physiology, 11, 24. https://doi.org/10.3389/fphys.2020.00024
McKeown, P. (2021). The Breathing Cure: Develop New Habits for a Healthier, Happier, and Longer Life. Boca Raton, Fl “Humanix Books. https://www.amazon.com/BREATHING-CURE-Develop-Healthier-Happier/dp/1630061972/
Meehan, Z.M. & Shaffer, F. (2023). Adding Core Muscle Contraction to Wrist-Ankle Rhythmical Skeletal Muscle Tension Increases Respiratory Sinus Arrhythmia and Low-Frequency Power. Appl Psychophysiol Biofeedback. 48(1), 127-134. https://doi.org/10.1007/s10484-022-09568-w
McKeown, P. (2021). The breathing cure: Develop new habits for a healthier, happier, and longer life. Humanix Books. https://www.amazon.com/BREATHING-CURE-Develop-Healthier-Happier/dp/1630061972/
Peper, E., Booiman, A., Lin, I-M, Harvey, R., & Mitose, J. (2016). Abdominal SEMG Feedback for Diaphragmatic Breathing: A Methodological Note. Biofeedback. 44(1), 42-49. https://doi.org/10.5298/1081-5937-44.1.03
Peper, E., Chen, S., Heinz, N. & Harvey, R. (2023). Hope for menstrual cramps (dysmenorrhea) with breathing. Biofeedback, 51(2), 44–51. https://doi.org/10.5298/1081-5937-51.2.04
Peper, E. & Cohen, T. (2017). Inhale to Breathe Away Pelvic Floor Pain and Enjoy Intercourse. Biofeedback, 45 (1), 21–24. https://doi.org/10.5298/1081-5937-45.1.04
Peper, E., Gilbert, C.D., Harvey, R. & Lin, I-M. (2015). Did you ask about abdominal surgery or injury? A learned disuse risk factor for breathing dysfunction. Biofeedback. 34(4), 173-179. https://doi.org/10.5298/1081-5937-43.4.06
Peper, E., Harvey, R., Cuellar, Y., & Membrila, C. (2022). Reduce anxiety. NeuroRegulation, 9(2), 91–97. https://doi.org/10.15540/nr.9.2.91
Peper, E., Harvey, R., & Hamiel, D. (2019). Transforming thoughts with postural awareness to increase therapeutic and teaching efficacy. NeuroRegulation, 6(3),153-169. https://doi.org/10.15540/nr.6.3.153
Peper, E., Harvey, R. & Rosegard, E. (2024). Increase attention, concentration and school performance with posture feedback. Biofeedback, 52(2). https://doi.org/10.5298/1081-5937-52.02.07 or https://www.researchgate.net/publication/383151816_WHAT_ABOUT_THIS_Increase_Attention_Concentration_and_School_Performance_with_Posture_Feedback
Peper, E. & MacHose, M. (1993). Symptom prescription: Inducing anxiety by 70% exhalation. Applied Psychophysiology and Biofeedback, 18(3), 133-138. https://doi.org/10.1007/BF00999790
Peper, E., Mason, L., Harvey, R., Wolski, L, & Torres, J. (2020). Can acid reflux be reduced by breathing? Townsend Letters-The Examiner of Alternative Medicine, 445/446, 44-47. https://www.townsendletter.com/article/445-6-acid-reflux-reduced-by-breathing/
Peper, E., Mason, L., Huey, C. (2017). Healing irritable bowel syndrome with diaphragmatic breathing. Biofeedback. 45(4), 83–87. https://doi.org/10.5298/1081-5937-45.4.04
Peper, E., Oded, Y., & Harvey, R. (2024a). Quick somatic rescue techniques when stressed. Biofeedback, 52(1), 18–26. https://doi.org/10.5298/982312
Peper, E., Pollack, W., Harvey, R., Yoshino, A., Daubenmier, J. & Anziani, M. (2019a). Which quiets the mind more quickly and increases HRV: Toning or mindfulness? NeuroRegulation, 6(3), 128-133. https://doi.org/10.15540/nr.6.3.12
Peper, E., Swatzyna, R., & Ong, K. (2023). Mouth breathing and tongue position: a risk factor for health. Biofeedback. 51(3), 74–78 https://doi.org/10.5298/912512
PTI. (2023 August 3). Often suck your stomach in to look slimmer in pictures? It can lead to ‘hourglass syndrome.’ The Economic Times Panache. Accessed March 26, 2024. https://economictimes.indiatimes.com/magazines/panache/often-suck-your-stomach-in-to-look-slimmer-in-pictures-it-can-lead-to-hourglass-syndrome/articleshow/102392681.cms?from=mdr
Salah, H.M., Goldberg, L.R., Molinger, J., Felker, G.M., Applefeld, W., Rassaf, T., Tedford, R.J., Mirro, M., Cleland, J.GF., & Fudim, M. (2022). Diaphragmatic Function in Cardiovascular Disease: JACC Review Topic of the Week, Journal of the American College of Cardiology, 80(17), 1647-1659. https://doi.org/10.1016/j.jacc.2022.08.760
Shaffer, F. & Meehan, Z.M. (2020). A Practical Guide to Resonance Frequency Assessment for Heart Rate Variability Biofeedback. Frontiers in Neuroscience,14. https://www.frontiersin.org/journals/neuroscience/articles/10.3389/fnins.2020.570400
Steffen, P.R., Austin, T., DeBarros, A., & Brown, T. (2017). The Impact of Resonance Frequency Breathing on Measures of Heart Rate Variability, Blood Pressure, and Mood. Front Public Health, 5, 222. https://doi.org/10.3389/fpubh.2017.00222
Taub, E., Uswatte, G., Mark, V. W., Morris, D. M. (2006). The learned nonuse phenomenon: Implications for rehabilitation. Europa Medicophysica, 42(3), 241-256. https://pubmed.ncbi.nlm.nih.gov/17039223/
van Bon, M.J., Zielhuis, G.A., Rach, G.H., & van den Broek, P. (1989). Otitis media with effusion and habitual mouth breathing in Dutch preschool children. Int J Pediatr Otorhinolaryngol, (2), 119-25. https://doi.org/10.1016/0165-5876(89)90087-6
Xiao, M., Zi-Qi, Y., Gong, Z.Q., Zhang, H., Duan, N.Y., Shi, Y.T,, Wei, G.X., Li, Y.F. (2017).The Effect of Diaphragmatic Breathing on Attention, Negative Affect and Stress in Healthy Adults. Front Psychol. 8(874). https://doi.org/10.3389/fpsyg.2017.00874
Cellphones affects social communication, vision, breathing, and health: What to do!
Posted: September 4, 2024 Filed under: ADHD, attention, behavior, Breathing/respiration, cellphone, computer, digital devices, educationj, ergonomics, health, laptops, Neck and shoulder discomfort, posture, screen fatigue, self-healing, stress management, techstress, Uncategorized, vision, zoom fatigue | Tags: communication, myopia, pedestrian deaths, peripheral vision, text neck 7 CommentsAdapted from: Peper, E. & Harvey, R. (2024). Cell phones affects social communication, vision, breathing, and mental and physical health: What to do! TownsendLetter-The Examiner of Alternative Medicine,September 15, 2024. https://townsendletter.com/smartphone-affects-social-communication-vision-breathing-and-mental-and-physical-health-what-to-do/

Abstract
Smartphones are an indispensable part of our lives. Unfortunately too much of a ‘good thing’ regarding technology can work against us, leading to overuse, which in turn influences physical, mental and emotional development among current ‘Generation Z’ and ‘Millennial’ users (e.g., born 1997-2012, and 1981-1996, respectively). Compared to older technology users, Generation Z report more mental and physical health problems. Categories of mental health include attentional deficits, feelings of depression, anxiety social isolation and even suicidal thoughts, as along with physical health complaints such as sore neck and shoulders, eyestrain and increase in myopia. Long duration of looking downward at a smartphone affects not only eyestrain and posture but it also affects breathing which burden overall health. The article provides evidence and practices so show how technology over use and slouching posture may cause a decrease in social interactions and increases in emotional/mental and physical health symptoms such as eyestrain, myopia, and body aches and pains. Suggestions and strategies are provided for reversing the deleterious effects of slouched posture and shallow breathing to promote health.
We are part of an uncontrolled social experiment
We, as technology users, are all part of a social experiment in which companies examine which technologies and content increase profits for their investors (Mason, Zamparo, Marini, & Ameen, 2022). Unlike University research investigations which have a duty to warn of risks associated with their projects, we as participants in ‘profit-focused’ experiments are seldom fully and transparently informed of the physical, behavioral and psychological risks (Abbasi, Jagaveeran, Goh, & Tariq, 2021; Bhargava, & Velasquez, 2021). During university research participants must be told in plain language about the risks associated with the project (Huh-Yoo & Rader, 2020; Resnik, 2021). In contrast for-profit technology companies make it possible to hurriedly ‘click through’ terms-of-service and end-user-license-agreements, ‘giving away’ our rights to privacy, then selling our information to the highest bidder (Crain, 2021; Fainmesser, Galeotti, & Momot, 2023; Quach et al., 2022; Yang, 2022).
Although some people remain ignorant and or indifferent (e.g., “I don’t know and I don’t care”) about the use of our ‘data,’ an unintended consequence of becoming ‘dependent’ on technology overuse includes the strain on our mental and physical health (Abusamak, Jaber & Alrawashdeh, 2022; Padney et al., 2020). We have adapted new technologies and patterns of information input without asking the extent to which there were negative side effects (Akulwar-Tajane, Parmar, Naik & Shah, 2020; Elsayed, 2021). As modern employment shifted from predominantly blue-collar physical labor to white collar information processing jobs, people began sitting more throughout the day. Workers tended to look down to read and type. ‘Immobilized’ sitting for hours of time has increased as people spend time working on a computer/laptop and looking down at smartphones (Park, Kim & Lee, 2020). The average person now sits in a mostly immobilized posture 10.4 hours/day and modern adolescents spent more than two thirds of their waking time sitting and often looking down at their smartphones (Blodgett, et al., 2024; Arundell et al., 2019).
Smartphones are an indispensable part of our lives and is changing the physical and mental emotional development especially of Generation Z who were born between 1997-2012 (Haidt, 2024). They are the social media and smartphone natives (Childers & Boatwright, 2021). The smartphone is their personal computer and the gateway to communication including texting, searching, video chats, social media (Hernandez-de-Menendez, Escobar Díaz, & Morales-Menendez, 2020; Nichols, 2020; Schenarts, 2020; Szymkowiak et al., 2021). It has 100,000 times the processing power of the computer used to land the first astronauts on the moon on July 20, 1969 according to University of Nottingham’s computer scientist Graham Kendal (Dockrill, 2020). More than one half of US teens spend on the average more than 7 hours on daily screen time that includes watching streaming videos, gaming, social media and texting and their attention span has decreased from 150 seconds in 2004 to an average of 44 seconds in 2021 (Duarte, F., 2023; Mark, 2022, p. 96).
For Generation Z, social media use is done predominantly with smartphones while looking down. It has increased mental health problems such as attentional deficits, depression, anxiety suicidal thoughts, social isolation as well as decreased physical health (Haidt, 2024; Braghieri et al., 2023; Orsolini, Longo & Volpe, 2023; Satılmış, Cengız, & Güngörmüş, 2023; Muchacka-Cymerman, 2022; Fiebert, Kistner, Gissendanner & DaSilva, 2021; Mohan et al., 2021; Goodwin et al., 2020).
The shift in communication from synchronous (face-to-face) to asynchronous (texting) has transformed communications and mental health as it allows communication while being insulated from the other’s reactions (Lewis, 2024). The digital connection instead of face-to-face connection by looking down at the smart phone also has decreased the opportunity connect with other people and create new social connections, with three typical hypotheses examining the extent to which digital technologies (a) displace/ replace; (b) compete/ interfere with; and/or, (c) complement/ enhance in-person activities and relationships (Kushlev & Leitao, 2020).
As described in detail by Jonathan Haidt (2024), in his book, The Anxious Generation, the smartphone and the addictive nature of social media combined with the reduction in exercise, unsupervised play and childhood independence was been identified as the major factors in the decrease in mental health in your people (Gupta, 2023). This article focuses less on distraction such as attentional deficits, or dependency leading to tolerance, withdrawal and cravings (e.g., addiction-like symptoms) and focuses more on ‘dysregulation’ of body awareness (posture and breathing changes) and social communication while people are engaged with technology (Nawaz,Bhowmik, Linden & Mitchell, 2024).
The excessive use of the smartphones is associated with a significant reduction of physical activity and movement leading to a so-called sedentarism or increases of sitting disease (Chandrasekaran & Ganesan, 2021; Nakshine, Thute, Khatib, & Sarkar, 2022). Unbeknown to the smartphone users their posture changes, as they looks down at their screen, may also affect their mental and physical health (Aliberti, Invernizzi, Scurati & D’lsanto, 2020).
(1) Explore how looking at your smartphone affects you (adapted from: Peper, Harvey, & Rosegard, 2024)
For a minute, sit in your normal slouched position and look at your smartphone while intensely reading the text or searching social media. For the next minute sit tall and bring the cell phone in front of you so you can look straight ahead at it. Again, look at your smartphone while intensely reading the text or searching social media.
Compare how the posture affects you. Most likely, your experience is similar to the findings from students in a classroom observational study. Almost all experienced a reduction in peripheral awareness and breathed more shallowly when they slouched while looking at their cellphone.
Decreased peripheral awareness and increased shallow breathing that affects physical and mental health and performance. The students reported looking down position reduces the opportunity of creating new social connections. Looking down my also increases the risk for depression along with reduced cognitive performance during class (Peper et al., 2017; Peper et al., 2018).
(2) Explore how posture affects eye contact (adapted from the exercise shared by Ronald Swatzyna, 2023)[2]
Walk around your neighborhood or through campus either looking downwards or straight ahead for 30 minutes while counting the number of eye contacts you make.
Most likely, when looking straight ahead and around versus slouched and looking down you had the same experience as Ronald Swatzyna (2023), Licensed Clinical Social Worker. He observed that when he walked a three-mile loop around the park in a poor posture with shoulders forward in a head down position, and then reversed direction and walked in good posture with the shoulders back and the head level, he would make about five times as many eye contacts with a good posture compared to the poor posture.
Anecdotal observations, often repeated by many educators, suggest before the omnipresent smartphone, students would look around and talk to each other before a university class began. Now, when Generation Z students enter an in-person class, they sit down, look down at their phone and tend not to interact with other students.
(3) Experience the effect of face-to-face in-person communication
During the first class meeting, ask students to put their cellphones away, meet with three or four other students for a few minutes, and share a positive experience that happened to them last week as well as what they would like to learn in the class. After a few minutes, ask them to report how their energy and mood changed.
In our observational class study with 24 junior and senior college students in the in-person class and 54 students in the online zoom class, almost all report that that their energy and positive mood increased after they interacted with each other. The effects were more beneficial for the in-person small group sharing than the online breakout groups sharing on Zoom as shown in Figure 1.

Figure 1. Change in subjective energy and mood after sharing experiences synchronously in small groups either in-person or online.
Without direction of a guided exercise to increase social connections, students tend to stay within their ‘smartphone bubble’ while looking down (Bochicchio et al., 2022). As a result, they appear to be more challenged to meet and interact with other people face-to-face or by phone as is reflected in the survey data that Generation Z is dating much less and more lonely than the previous generations (Cox et al., 2023).
What to do:
- Put the smartphone away so that you do not see it in social settings such as during meals or classes. This means that other people can be present with you and the activity of eating or learning.
- Do not permit smartphones in the classroom including universities unless it is required for a class assignment.
- In classrooms and in the corporate world, create activities that demands face-to-face synchronous communication.
- Unplug from the audio programs when walking and explore with your eyes what is going on around you.
(4) Looking down increases risk of injury and death
Looking down at a close screen reduces peripheral awareness and there by increases the risk of accidents and pedestrian deaths. Pedestrian deaths are up 69% since 2011 (Cova, 2024) and have consistently increased since the introduction of the iPhone in 2007 as shown in Figure 3.

Figure 3. Increase in pedestrian death since the introduction of the iphone (data plotted from https://www.iihs.org/topics/fatality-statistics/detail/pedestrians)
In addition, the increase use of mobile phones is also associated with hand and wrist pain from overuse and with serious injuries such as falls and texting while driving due to lack of peripheral awareness. McLaughlin et al (2023) reports an increase in hand and wrist injuries as well serious injuries related to distracted behaviors, such as falls and texting while driving. The highest phone related injuries (lacerations) as reported from the 2011 to 2020 emergency room visits were people in the age range from 11–20 years followed by 21–30 years.
What to do:
- Do not walk while looking at your smartphone. Attend to the environment around you.
- Unplug from the audio podcasts when walking and explore with your eyes what is going on around you.
- Sit or stop walking when answering the smartphone to reduce the probability of an accident.
- For more pragmatic suggestions, see the book, TechStress: How Technology is Hijacking Our Lives, Strategies for Coping, and Pragmatic Ergonomics, by Peper, Harvey and Faass (2020).
(5) Looking at screens increases the risk of myopia
Looking at a near screen for long periods of time increases the risk of myopia (near sightedness) which means that distant vision is more blurry. Myopia has increased as children predominantly use computers or, smartphones with smaller screen at shorter distances. By predominantly focusing on nearby screens without allowing the eye to relax remodels the eyes structure. Consequently, myopia has increase in the U.S. from 25 percent in the early 1970s to nearly 42 percent three decades later (OHSU, 2022).
Looking only at nearby screens, our eyes converge and the ciliary muscles around the lens contract and remain contracted until the person looks at the far distance. The less opportunity there is to allow the eyes to look at distant vision, the more myopia occurs. in Singapore 80 per cent of young people aged 18 or below have nearsightedness and 20 % of the young people have high myopia as compared to 10 years ago (Singapore National Eye Centre, 2024). The increase in myopia is a significant concern since high myopia is associated with an increased risk of vision loss due to cataract, glaucoma, and myopic macular degeneration (MMD). MMD is rapidly increasing and one of the leading causes of blindness in East Asia that has one of the highest myopia rates in the world (Sankaridurg et al., 2021).
What to do:
- Every 20 minutes stop looking at the screen and look at the far distance to relax the eyes for 20 seconds.
- Do not allow young children access to cellphones or screens. Let them explore and play in nature where they naturally alternate looking at far and near objects.
- Implement the guided eye regenerating practices descrubed in the article, Resolve eyestrain and screen fatigue, by Peper (2021).
- Read Meir Schneider’s (2016) book, Vision for Life, for suggestions how to maintain and improve vision.
(6) Looking down increases tech neck discomfort
Looking down at the phone while standing or sitting strains the neck and shoulder muscles because of the prolonged forward head posture as illustrated in the YouTube video, Tech Stress Symptoms and Causes (DeWitt, 2018). Using a smartphone while standing or walking causes a significant increase in thoracic kyphosis and trunk (Betsch et al., 2021). When the head is erect, the muscle of the neck balance a weight of about 10 to 12 pounds or, approximately 5 kilograms; however, when the head is forward at 60 degrees looking at your cell phone the forces on the muscles are about 60 pound or more than 25 kilograms, as illustrated in Figure 4 (Hansraj, 2014).

Figure 4. The head forward position puts as much as sixty pounds of pressure on the neck muscles and spine (by permission from Dr. Kenneth Hansraj, 2014).
This process is graphically illustrated in the YouTube video, Text Neck Symptoms and Causes Video, produced by Veritas Health (2020).
What to do:
- Keep the phone in front of you so that you do not slouch down by having your elbow support on the table.
- Every ten minutes stretch, look up and roll your shoulders backwards.
- Wear a posture feedback device such as the UpRight Go 2 to remind you when you slouch to change posture and activity (Peper et al., 2019; Stuart, Godfrey & Mancini, 2022).
- Take Alexander Technique lessons to improve your posture (Cacciatore, Johnson, & Cohen, 2020; AmAT, 2024; STAT, 2024).
(7) Looking down increases negative memory recall and depression
In our previous research, Peper et al. (2017) have found that recalling hopeless, helpless, powerless, and defeated memories is easier when sitting in a slouched position than in an upright position. Recalling positive memories is much easier when sitting upright and looking slightly upward than sitting slouched position. If attempting to recall positive memories the brain has to work hard as indicated by an significantly higher amplitudes of beta2, beta3, and beta4 EEG (i.e., electroencephalograph) when sitting slouched then when sitting upright (Tsai et al., 2016).
Not only does the postural position affect memory recall, it also affects mental math under time-pressure performance. When students sit in a slouched position, they report that is much more difficult to do mental math (serial 7ths) than when in the upright position (Peper et al., 2018). The effect of posture is most powerful for the 70% of students who reported that they blanked out on exams, were anxious, or worried about class performance or math. For the 30% who reported no performance anxiety, posture had no significant effect. When students become aware of slouching thought posture feedback and then interrupt their slouching by sitting up, they report an increase in concentration, attention and school performance (Peper et al., 2024).
How we move and walk also affects our subjective energy. In most cases, when people sit for a long time, they report feeling more fatigue; however, if participants interrupt sitting with short movement practices they report becoming less fatigue and improved cognition (Wennberg et al., 2016). The change in subjective energy and mood depends upon the type of movement practice. Peper & Lin (2012) reported that when students were asked to walk in a slow slouching pattern looking down versus to walk quickly while skipping and looking up, they reported that skipping significantly increased their subjective energy and mood while the slouch walking decreased their energy. More importantly, student who had reported that they felt depressed during the last two years had their energy decrease significantly more when walking very slowly while slouched than those who did not report experiencing depression. Regardless of their self-reported history of depression, when students skipped, they all reported an increase in energy (Peper & Lin, 2012; Miragall et al., 2020).
What to do:
- Walk with a quick step while looking up and around.
- Wear a posture feedback device such as the UpRight Go 2 to remind you when you slouch to change posture and activity (Peper et al., 2019; Roggio et al., 2021).
- When sitting put a small pillow in the mid back so that you can sit more erect (for more suggestions, see the article by Peper et al., 2017a, Posture and mood: Implications and applications to therapy).
- Place photo and other objects that you like to look a slightly higher on your wall so that you automatically look up.
(8) Shallow breathing increases the risk for anxiety
When slouching we automatically tend to breathe slightly faster and more shallowly. This breathing pattern increases the risk for anxiety since it tends to decrease pCO2 (Feinstein et al., 2022; Meuret, Rosenfield, Millard & Ritz, 2023; Paulus, 2013; Smits et al., 2022; Van den Bergh et al., 2013). Sitting slouched also tends to inhibit abdominal expansion during the inhalation because the waist is constricted by clothing or a belt –sometimes labeled as ‘designer jean syndrome’ and may increase abdominal symptoms such as acid reflux and irritable bowel symptoms (Engeln & Zola, 2021; Peper et al., 2016; Peper et al., 2020). When students learn diaphragmatic breathing and practice diaphragmatic breathing whenever they shallow breathe or hold their breath, they report a significant decrease in anxiety, abdominal symptoms and even menstrual cramps (Haghighat et al., 2020; Peper et al., 2022; Peper et al., 2023).
What to do:
- Loosen your belt and waist constriction when sitting so that the abdomen can expand.
- Learn and practice effortless diaphragmatic breathing to reduce anxiety.
Conclusion
There are many topics related to postural health and technology overuse that were addressed in this article. Some topics are beyond the scope of the article, and therefore seen as limitations. These relate to diagnosis and treatment of attentional deficits, or dependency leading to tolerance, withdrawal and cravings (e.g., addiction-like symptoms), or of modeling relationships between factors that contribute to the increasing epidemic of mental and physical illness associated with smartphone use and social media, such as hypotheses examining the extent to which digital technologies (a) displace/ replace; (b) compete/ interfere with; and/or, (c) complement/ enhance in-person activities and relationships. Typical pharmaceutical ‘treat-the-symptom’ approaches for addressing ‘tech stress’ related to technology overuse includes prescribing ‘anxiolytics, pain-killers and muscle relaxants’ (Kazeminasab et al., 2022; Kim, Seo, Abdi, & Huh, 2020). Although not usually included in diagnosis and treatment strategies, suggesting improving posture and breathing practices can significantly affect mental and physical health. By changing posture and breathing patterns, individuals may have the option to optimize their health and well-being.
See the book, TechStress-How Technology is Hijacking our Lives, Strategies for Coping and Pragmatic Ergonomics by Erik Peper, Richard Harvey and Nancy Faass. Available from: https://www.amazon.com/Beyond-Ergonomics-Prevent-Fatigue-Burnout/dp/158394768X/

Explore the following blogs for more background and useful suggestions
References
Abbasi, G. A., Jagaveeran, M., Goh, Y. N., & Tariq, B. (2021). The impact of type of content use on smartphone addiction and academic performance: Physical activity as moderator. Technology in Society, 64, 101521. https://doi.org/10.1016/j.techsoc.2020.101521
Abusamak, M., Jaber, H. M., & Alrawashdeh, H. M. (2022). The effect of lockdown due to the COVID-19 pandemic on digital eye strain symptoms among the general population: a cross-sectional survey. Frontiers in Public Health, 10, 895517. https://doi.org/10.3389/fpubh.2022.895517
Akulwar-Tajane, I., Parmar, K. K., Naik, P. H., & Shah, A. V. (2020). Rethinking screen time during COVID-19: impact on psychological well-being in physiotherapy students. Int J Clin Exp Med Res, 4(4), 201-216. https://doi.org/10.26855/ijcemr.2020.10.014
Aliberti, S., Invernizzi, P. L., Scurati, R., & D’Isanto, T. (2020). Posture and skeletal muscle disorders of the neck due to the use of smartphones. Journal of Human Sport and Exercise , 15 (3proc), S586-S598. https://www.jhse.ua.es/article/view/2020-v15-n3-proc-posture-skeletal-muscle-disorders-neck-smartpho; https://air.unimi.it/retrieve/handle/2434/774436/1588570/HSE%20-%20Posture%20and%20skeletal%20muscle%20disorders.pdf
AmSAT. (2024). American Society for the Alexander Technique. Accessed July 27, 2024. https://alexandertechniqueusa.org/
Arundell, L., Salmon, J., Koorts, H. et al. (2019). Exploring when and how adolescents sit: cross-sectional analysis of activPAL-measured patterns of daily sitting time, bouts and breaks. BMC Public Health 19, 653. https://doi.org/10.1186/s12889-019-6960-5
Bhargava, V. R., & Velasquez, M. (2021). Ethics of the attention economy: The problem of social media addiction. Business Ethics Quarterly, 31(3), 321-359. https://doi.org/10.1017/beq.2020.32
Betsch, M., Kalbhen, K., Michalik, R., Schenker, H., Gatz, M., Quack, V., Siebers, H., Wild, M., & Migliorini, F. (2021). The influence of smartphone use on spinal posture – A laboratory study. Gait Posture, 85, 298-303. https://doi.org/10.1016/j.gaitpost.2021.02.018
Blodgett, J.M., Ahmadi, M.N., Atkin, A.J., Chastin, S., Chan, H-W., Suorsa, K., Bakker, E.A., Hettiarcachchi, P., Johansson, P.J., Sherar,L. B., Rangul, V., Pulsford, R.M…. (2024). ProPASS Collaboration , Device-measured physical activity and cardiometabolic health: the Prospective Physical Activity, Sitting, and Sleep (ProPASS) consortium, European Heart Journal, 45(6) 458–471, https://doi.org/10.1093/eurheartj/ehad717
Bochicchio, V., Keith, K., Montero, I., Scandurra, C., & Winsler, A. (2022). Digital media inhibit self-regulatory private speech use in preschool children: The “digital bubble effect”. Cognitive Development, 62, 101180. https://doi.org/10.1016/j.cogdev.2022.101180
Braghieri, L., Levy, R., & Makarin, A. (2022). Social Media and Mental Health (July 28, 2022). Available at SSRN: https://ssrn.com/abstract=3919760 or http://dx.doi.org/10.2139/ssrn.3919760
Cacciatore, T. W., Johnson, P. M., & Cohen, R. G. (2020). Potential mechanisms of the Alexander technique: Toward a comprehensive neurophysiological model. Kinesiology Review, 9(3), 199-213. https://doi.org/10.1123/kr.2020-0026
Chandrasekaran, B., & Ganesan, T. B. (2021). Sedentarism and chronic disease risk in COVID 19 lockdown–a scoping review. Scottish Medical Journal, 66(1), 3-10. https://doi.org/10.1177/0036933020946336
Childers, C., & Boatwright, B. (2021). Do digital natives recognize digital influence? Generational differences and understanding of social media influencers. Journal of Current Issues & Research in Advertising, 42(4), 425-442. https://doi.org/10.1080/10641734.2020.1830893
Cox, D.A., Hammond, K.E., & Gray, K. (2023). Generation Z and the Transformation of American Adolescence: How Gen Z’s Formative Experiences Shape Its Politics, Priorities, and Future. Survey Center of American Life, November 23, 2023. Accessed July 4, 2024. https://www.americansurveycenter.org/research/generation-z-and-the-transformation-of-american-adolescence-how-gen-zs-formative-experiences-shape-its-politics-priorities-and-future/
Crain, M. (2021). Profit over privacy: How surveillance advertising conquered the internet. U of Minnesota Press. https://www.amazon.com/Profit-over-Privacy-Surveillance-Advertising/dp/1517905044
Cova, E. (2024). Pedestrian fatalities at historic high. Smart Growth America (data from U.S. Department of Transportation (USDOT). Accessed July 2, 2024. https://smartgrowthamerica.org/pedestrian-fatalities-at-historic-high/
Duarte, F. (2023). Average Screen Time for Teens (2024). Exploding Topics. Accessed July 5, 2024. https://explodingtopics.com/blog/screen-time-for-teens#average
DeWitt, D. (2018). How Does Text Neck Cause Pain? Spine-Health October 26, 2018. Accessed July 5, 2024. https://www.spine-health.com/conditions/neck-pain/how-does-text-neck-cause-pain
Dockrill, P. (2020). Your laptop charger is more powerful than Apollo11’s computer, says apple developer. Science Alert, Janural 12, 2020. Accessed July 4, 2024. https://www.sciencealert.com/apollo-11-s-computer-was-less-powerful-than-a-usb-c-charger-programmer-discovers
Elsayed, W. (2021). Covid-19 pandemic and its impact on increasing the risks of children’s addiction to electronic games from a social work perspective. Heliyon, 7(12). https://doi.org/10.1016/j.heliyon.2021.e08503
Engeln, R., & Zola, A. (2021). These boots weren’t made for walking: gendered discrepancies in wearing painful, restricting, or distracting clothing. Sex roles, 85(7), 463-480. https://doi.org/10.1007/s11199-021-01230-9
Fainmesser, I. P., Galeotti, A., & Momot, R. (2023). Digital privacy. Management Science, 69(6), 3157-3173. https://doi.org/10.1287/mnsc.2022.4513
Feinstein, J. S., Gould, D., & Khalsa, S. S. (2022). Amygdala-driven apnea and the chemoreceptive origin of anxiety. Biological psychology, 170, 108305. https://10.1016/j.biopsycho.2022.108305
Fiebert, I., Kistner, F., Gissendanner, C., & DaSilva, C. (2021). Text neck: An adverse postural phenomenon. Work, 69(4), 1261-1270. https://doi.org/10.3233/WOR-213547
Goodwin, R. D., Weinberger, A. H., Kim, J. H., Wu. M., & Galea, S. (2020). Trends in anxiety among adults in the United States, 2008–2018: Rapid increases among young adults. Journal of Psychiatric Research. 130, 441–446. https://doi.org/10.1016/j.jpsychires.2020.08.014
Gupta, N. (2023). Impact of smartphone overuse on health and well-being: review and recommendations for life-technology balance. Journal of Applied Sciences and Clinical Practice, 4(1), 4-12. https://doi.org/10.4103/jascp.jascp_40_22
Haghighat, F., Moradi, R., Rezaie, M., Yarahmadi, N., & Ghaffarnejad, F. (2020). Added Value of Diaphragm Myofascial Release on Forward Head Posture and Chest Expansion in Patients with Neck Pain: A Randomized Controlled Trial. Research Square. https://doi.org/10.21203/rs.3.rs-53279/v1
Haidt, J. (2024). The Anxious generation: How the great rewiring of childhood is causing an epidemic of mental illness. New York: Penguin Press. https://www.anxiousgeneration.com/book
Hansraj, K.K. (2014). Assessment of stresses in the cervical spine caused by posture and position of the head. Surg Technol Int. 25, 277-279. https://pubmed.ncbi.nlm.nih.gov/25393825/
Hernandez-de-Menendez, M., Escobar Díaz, C. A., & Morales-Menendez, R. (2020). Educational experiences with Generation Z. International Journal on Interactive Design and Manufacturing (IJIDeM), 14(3), 847-859. https://doi.org/10.1007/s12008-020-00674-9
Huh-Yoo, J., & Rader, E. (2020). It’s the Wild, Wild West: Lessons learned from IRB members’ risk perceptions toward digital research data. Proceedings of the ACM on Human-Computer Interaction, 4(CSCW1), 1-22. https://doi.org/10.1145/3392868
IIHS (2024). Fatality Facts 2022Pedestrians. The Insurance Institute for Highway Safety (IIHS). Accessed July 2, 2024. https://www.iihs.org/topics/fatality-statistics/detail/pedestrians
Kazeminasab, S., Nejadghaderi, S. A., Amiri, P., Pourfathi, H., Araj-Khodaei, M., Sullman, M. J., … & Safiri, S. (2022). Neck pain: global epidemiology, trends and risk factors. BMC musculoskeletal disorders, 23, 1-13. https://doi.org/10.1186/s12891-021-04957-4
Kim, K. H., Seo, H. J., Abdi, S., & Huh, B. (2020). All about pain pharmacology: what pain physicians should know. The Korean journal of pain, 33(2), 108-120. https://doi.org/10.3344/kjp.2020.33.2.108
Kushlev, K., & Leitao, M. R. (2020). The effects of smartphones on well-being: Theoretical integration and research agenda. Current opinion in psychology, 36, 77-82. https://doi.org/10.1016/j.copsyc.2020.05.001
Lewis, H.R. (2024). Mechanical intelligence and counterfeit humanity. Harvard Magazine, 126(6), 38-40. https://www.harvardmagazine.com/2024/07/harry-lewis-computers-humanity#google_vignette
Mark, G. (2023). Attention Span: A Groundbreaking Way to Restore Balance, Happiness and Productivity. Toronto, Canada: Hanover Square Press. https://www.amazon.com/Attention-Span-Finding-Fighting-Distraction-ebook/dp/B09XBJ29W9
Mason, M. C., Zamparo, G., Marini, A., & Ameen, N. (2022). Glued to your phone? Generation Z’s smartphone addiction and online compulsive buying. Computers in Human Behavior, 136, 107404. https://doi.org/10.1016/j.chb.2022.107404
McLaughlin, W.M., Cravez, E., Caruana, D.L., Wilhelm, C., Modrak, M., & Gardner, E.C. (2023). An Epidemiological Study of Cell Phone-Related Injuries of the Hand and Wrist Reported in United States Emergency Departments From 2011 to 2020. J Hand Surg Glob, 5(2),184-188. https://doi.org/10.1016/j.jhsg.2022.11.009
Meuret, A. E., Rosenfield, D., Millard, M. M., & Ritz, T. (2023). Biofeedback Training to Increase Pco2 in Asthma With Elevated Anxiety: A One-Stop Treatment of Both Conditions?. Psychosomatic medicine, 85(5), 440-448. https://doi.org/10.1097/PSY.0000000000001188
Miragall, M., Borrego, A., Cebolla, A., Etchemendy, E., Navarro-Siurana, J., Llorens, R., … & Baños, R. M. (2020). Effect of an upright (vs. stooped) posture on interpretation bias, imagery, and emotions. Journal of Behavior Therapy and Experimental Psychiatry, 68, 101560. https://doi.org/10.1016/j.jbtep.2020.101560
Mohan, A., Sen, P., Shah, C., Jain, E., & Jain, S. (2021). Prevalence and risk factor assessment of digital eye strain among children using online e-learning during the COVID-19 pandemic: Digital eye strain among kids (DESK study-1). Indian journal of ophthalmology, 69(1), 140-144. https://doi.org/10.4103/ijo.IJO_2535_20
Muchacka-Cymerman, A. (2022). ‘I wonder why sometimes I feel so angry’ The associations between academic burnout, Facebook intrusion, phubbing, and aggressive behaviours during pandemic Covid 19. Polish Psychological Bulletin, 53(4). https://doi.org/10.24425/ppb.2022.143376
Nakshine, V. S., Thute, P., Khatib, M. N., & Sarkar, B. (2022). Increased screen time as a cause of declining physical, psychological health, and sleep patterns: a literary review. Cureus, 14(10). https://doi.org/10.7759/cureus.30051
Nawaz, S., Bhowmik, J., Linden, T., & Mitchell, M. (2024). Validation of a modified problematic use of mobile phones scale to examine problematic smartphone use and dependence. Heliyon, 10(2). https://doi.org/10.1016/j.heliyon.2024.e24832
Nicholas, A. J. (2020). Preferred learning methods of generation Z. Faculty and Staff – Articles & Papers. Digital Commons @ Salve Regina. Salve Regina University. https://digitalcommons.salve.edu/fac_staff_pub/74
OHSU. (2022). Myopia on the rise, especially among children. Casey Eye Institute. Oregan Health and Science University. Accessed July 7, 2024. https://www.ohsu.edu/casey-eye-institute/myopia-rise-especially-among-children
Orsolini, L., Longo, G., & Volpe, U. (2023). The mediatory role of the boredom and loneliness dimensions in the development of problematic internet use. International Journal of Environmental Research and Public Health, 20(5), 4446. https://doi.org/10.3390/ijerph20054446
Pandey, R., Gaur, S., Kumar, R., Kotwal, N., & Kumar, S. (2020). Curse of the technology-computer related musculoskeletal disorders and vision syndrome: a study. International Journal of Research in Medical Sciences, 8(2), 661. https://doi.org/10.18203/2320-6012.ijrms20200253
Park, J. C., Kim, S., & Lee, H. (2020). Effect of work-related smartphone use after work on job burnout: Moderating effect of social support and organizational politics. Computers in human behavior, 105, 106194. https://doi.org/10.1016/j.chb.2019.106194
Paulus, M.P. (2013). The breathing conundrum-interoceptive sensitivity and anxiety. Depress Anxiety.30(4), 315-20. https://doi.org/10.1002/da.22076
Peper, E. (2021). Resolve eyestrain and screen fatigue. Well Being Journal, 30(1), 24-28. https://wellbeingjournal.com/resolve-eyestrain-and-screen-fatigue/
Peper, E., Booiman, A., Lin, I-M, Harvey, R., & Mitose, J. (2016). Abdominal SEMG Feedback for Diaphragmatic Breathing: A Methodological Note. Biofeedback. 44(1), 42-49. https://doi.org/10.5298/1081-5937-44.1.03
Peper, E., Chen, S., Heinz, N. & Harvey, R. (2023). Hope for menstrual cramps (dysmenorrhea) with breathing. Biofeedback, 51(2), 44–51. https://doi.org/10.5298/1081-5937-51.2.04
Peper, E., Harvey, R., Cuellar, Y., & Membrila, C. (2022). Reduce anxiety. NeuroRegulation, 9(2), 91–97. https://doi.org/10.15540/nr.9.2.91
Peper, E., Harvey, R. & Faass, N. (2020). TechStress: How Technology is Hijacking Our Lives, Strategies for Coping, and Pragmatic Ergonomics. Berkeley: North Atlantic Books. https://www.amazon.com/Beyond-Ergonomics-Prevent-Fatigue-Burnout/dp/158394768X
Peper, E., Harvey, R., & Mason, L. (2019). “Don’t slouch!” Improve health with posture feedback. Townsend Letter-The Examiner of Alternative Medicine, 436, 58-61. https://www.researchgate.net/publication/337424599_Don%27t_slouch_Improve_health_with_posture_feedback
Peper, E., Harvey, R., Mason, L., & Lin, I.-M. (2018). Do better in math: How your body posture may change stereotype threat response. NeuroRegulation, 5(2), 67–74. http://dx.doi.org/10.15540/nr.5.2.67
Peper, E., Harvey, R. & Rosegard, E. (2024). Increase attention, concentration and school performance with posture feedback. Biofeedback, 52(2). https://doi.org/10.5298/1081-5937-52.02.07
Peper, E. & Lin, I-M. (2012). Increase or decrease depression-How body postures influence your energy level. Biofeedback, 40 (3), 126-130. https://doi.org/10.5298/1081-5937-40.3.01
Peper, E., Lin, I-M, & Harvey, R. (2017a). Posture and mood: Implications and applications to therapy. Biofeedback, 35(2), 42-48. https://doi.org/10.5298/1081-5937-45.2.03
Peper, E., Lin, I-M., Harvey, R., & Perez, J. (2017). How posture affects memory recall and mood. Biofeedback.45 (2), 36-41. https://doi.org/10.5298/1081-5937-45.2.01
Peper, E., Mason, L., Harvey, R., Wolski, L, & Torres, J. (2020). Can acid reflux be reduced by breathing? Townsend Letters-The Examiner of Alternative Medicine, 445/446, 44-47. https://www.townsendletter.com/article/445-6-acid-reflux-reduced-by-breathing/
Quach, S., Thaichon, P., Martin, K. D., Weaven, S., & Palmatier, R. W. (2022). Digital technologies: tensions in privacy and data. Journal of the Academy of Marketing Science, 50(6), 1299-1323. https://doi.org/10.1007/s11747-022-00845-y
Resnik, D. B. (2021). Standards of evidence for institutional review board decision-making. Accountability in research, 28(7), 428-455. https://doi.org/10.1080/08989621.2020.1855149
Roggio, F., Ravalli, S., Maugeri, G., Bianco, A., Palma, A., Di Rosa, M., & Musumeci, G. (2021). Technological advancements in the analysis of human motion and posture management through digital devices. World journal of orthopedics, 12(7), 467. https://doi.org/10.5312/wjo.v12.i7.467
Sankaridurg, P., Tahhan, N., Kandel, H., Naduvilath, T., Zou, H., Frick,K.D., Marmamula, S., Friedman, D.S., Lamoureux, e. Keeffe, J. Walline, J.J., Fricke, T.R., Kovai, V., & Resnikoff, S. (2021) IMI Impact of Myopia. Invest. Ophthalmol. Vis. Sci, 62(5), 2. https://doi.org/10.1167/iovs.62.5.2
Satılmış, S. E., Cengız, R., & Güngörmüş, H. A. (2023). The relationship between university students’ perception of boredom in leisure time and internet addiction during social isolation process. Bağımlılık Dergisi, 24(2), 164-173. https://doi.org/10.51982/bagimli.1137559
Schenarts, P. J. (2020). Now arriving: surgical trainees from generation Z. Journal of surgical education, 77(2), 246-253. https://doi.org/10.1016/j.jsurg.2019.09.004
Schneider, M. (2016). Vision for life. Ten Steps to Natural Eyesight Improvement. Berkeley: North Atlantic books. https://www.amazon.com/Vision-Life-Revised-Eyesight-Improvement/dp/1623170087
Singapore National Eye Centre. (2024). Severe myopia cases among children in Singapore almost doubled in past decade. CAN. Accessed July 4, 2024. https://www.channelnewsasia.com/singapore/myopia-children-cases-almost-double-glasses-eye-checks-4250266
Smits, J. A., Monfils, M. H., Otto, M. W., Telch, M. J., Shumake, J., Feinstein, J. S., … & Exposure Therapy Consortium. (2022). CO2 reactivity as a biomarker of exposure-based therapy non-response: study protocol. BMC psychiatry, 22(1), 831. https://doi.org/10.1186/s12888-022-04478-x
STAT (2024). The society of teachers of the Alexander Technique. Assessed July 27, 2024. https://alexandertechnique.co.uk/
Stuart, S., Godfrey, A., & Mancini, M. (2022). Staying UpRight in Parkinson’s disease: A pilot study of a novel wearable postural intervention. Gait & Posture, 91, 86-93. https://doi.org/10.1016/j.gaitpost.2021.09.202
Swatzyna, R. (2023). Personal communications.
Szymkowiak, A., Melović, B., Dabić, M., Jeganathan, K., & Kundi, G. S. (2021). Information technology and Gen Z: The role of teachers, the internet, and technology in the education of young people. Technology in Society, 65, 101565. https://doi.org/10.1016/j.techsoc.2021.101565
Tsai, H. Y., Peper, E., & Lin, I. M.*(2016). EEG patterns under positive/negative body postures and emotion recall tasks. NeuroRegulation, 3(1), 23-27. https://doi.org/10.15540/nr.3.1.23
Van den Bergh, O., Zaman, J., Bresseleers, J., Verhamme, P., Van Diest, I. (2013). Anxiety, pCO2 and cerebral blood flow, International Journal of Psychophysiology, 89 (1), 72-77. https://doi.org/10.1016/j.ijpsycho.2013.05.011
Veritas Health. (2020). Text Neck Symptoms and Causes Video. YouTube video, accessed August 29, 2024. https://www.spine-health.com/conditions/neck-pain/how-does-text-neck-cause-pain?source=YT
Wennberg, P., Boraxbekk, C., Wheeler, M., et al. (2016). Acute effects of breaking up prolonged sitting on fatigue and cognition: a pilot study. BMJ Open, 6, e009630. https://doi.org/10.1136/bmjopen-2015-009630
Yang, K. H. (2022). Selling consumer data for profit: Optimal market-segmentation design and its consequences. American Economic Review, 112(4), 1364-1393. https://www.aeaweb.org/articles/pdf/doi/10.1257/aer.20210616
[1] Correspondence should be addressed to: Erik Peper, Ph.D., Institute for Holistic Health Studies, Department of Recreation, Parks, Tourism and Holistic Health, San Francisco State University, 1600 Holloway Avenue, San Francisco, CA 94132 Email: epeper@sfsu.edu; web: www.biofeedbackhealth.org; blog: www.peperperspective.com
[2] I thank Ronald Swatzyna (2023), Licensed Clinical Social Worker for sharing this exercise with me. He discovered that a difference in the number of eye contacts depending how he walked. When he walked a 3.1 mile loop around the park in a poor posture- shoulders forward, head down position- and then reversed direction and walked in good posture with the shoulders back and the head level, that that he make about 5 times as many eye contacts with good posture compared to the poor posture. He observed that he make about five times as many eye contacts with good posture as compared to the poor posture.

