Digital fatigue and what to do
Posted: July 22, 2021 Filed under: Uncategorized 6 CommentsErik Peper, PhD and Monica Almendras
The article was adapted from the recent book, How Technology is Hijacking our Lives, Strategies for Coping and Pragmatic Ergonomics, and was originally published on the Big Q https://www.thebigq.org/2021/08/02/why-do-we-have-zoom-fatigue-and-what-can-we-do-about-it/
Why is it that after studying, working, entertaining and socializing at the computer screen or looking at texts, Instagram, Facebook, Tiktok or responding to notifications on the cellphone, we often feel exhausted (zoom fatigue) and experience neck, back and shoulders discomfort, or eye irritation? Time disappears as we surf the web and go down the rabbit hole by clicking on one and then another link or responding to social media. As time flies, we tend to be unaware that our muscles tighten, our breathing become shallow and quicker, our blinking rates decreases and our posture slouches forward as we bring our nose close to the screen to see the text more clearly.
Become aware what happens when you do the following experiential practices
Observe what happens when you mouse
Sit comfortable in an erect posture as if you are in front of your computer and hold a small object that you can use to simulate mousing to the side of the keyboard. With an actual mouse (or the sham mouse), pretend to draw the letters of your name and your street address backward, right to left. Be sure each letter is very small (less than half an inch in height). After drawing each letter, right click. Draw the letters and numbers as quickly as possible without making any mistakes for fifteen seconds. Stop and observe what happened in your body.
If you are like almost all participants you tightened your neck and shoulders, stiffened your trunk, held your breath and most did not blink. All this occurred without awareness. Over time, this covert tension can contribute to discomfort, soreness, pain, or eventual injury.
Observe the effect of low static muscle tension
You probably felt discomfort in the muscles of your hip. As you lifted your knee up, you most likely also held your breath and tightened your neck and back. Holding your muscles in a static position for more than a few minutes creates discomfort. Yet, when you walk you use the same muscles and usually do not experience discomfort. The main difference is that during walking you sequentially tighten and relax these muscles. Each time the muscle relaxes, blood flow is restored to remove the waste produces of metabolism and supply nutrients and oxygen to the muscle tissue. For more information, see the blog, Reactivate your second heart.
From the evolutionary perspective, people typically shifted between sitting, walking, and moving in varied ways during specified forms of labor which tends to tighten and relax different muscles. Therefore, incorporate dynamic movement’ during the day: Stand up, wiggle and move several times an hour. To avoid sitting disease, install a break reminder program such as StretchBreak on your computer or other digital devices. When people implement taking breaks, they report having much more energy at the end of the day. As one participant stated: “There is now life after five”. What he meant was that at the end of the day when he got home, he still had energy to other things.
Observe how breathing and opening eyes affect tearing
Inhale with a gasp as you open your eyes. Close your eyes, then exhale and inhale with a gasp as if you are surprised and at the same time open your eyes then look as if you are quickly responding to a notification. Repeat one or two time and be sure to open your eyes wide the moment you gasp as you inhale
Exhale and slowly open your eyes. Close your eyes, then inhale by allowing your abdomen to expand and begin exhaling and slowly open your eyes. Repeat one or two more times as you open your eyes midway through the exhalation, while your shoulders relax. What did you experience?
Most likely when you opened your eyes while exhaling you found that your eyes felt more relaxed with more tearing moisture in the eyes, while gasping and looking the eyes felt tense and more dry. In most cases when we focus without awareness intensely at the screen we create eye tension. Thus, practice blinking by resting and closing your eyes then gently open your eyes as you exhale and then looking at the far distance relax the muscles of the eyes. For detailed instructions see the blog, Are you encouraging your child to get into accidents or even blind when growing up?
We are usually unaware that our bodies respond automatically and that these patterns occur covertly and totally without awareness while working at the computer or responding to texts. We only notice when symptoms of discomfort occur. Fortunately, it is possible to monitor the degree of muscle tension with an electromyograph (EMG). The unaware muscle tension can be identified by physiological recording of the electrical activity produced when they contract. With biofeedback and coaching people can learn to become aware of the covert tension and as shown in Figure 1.
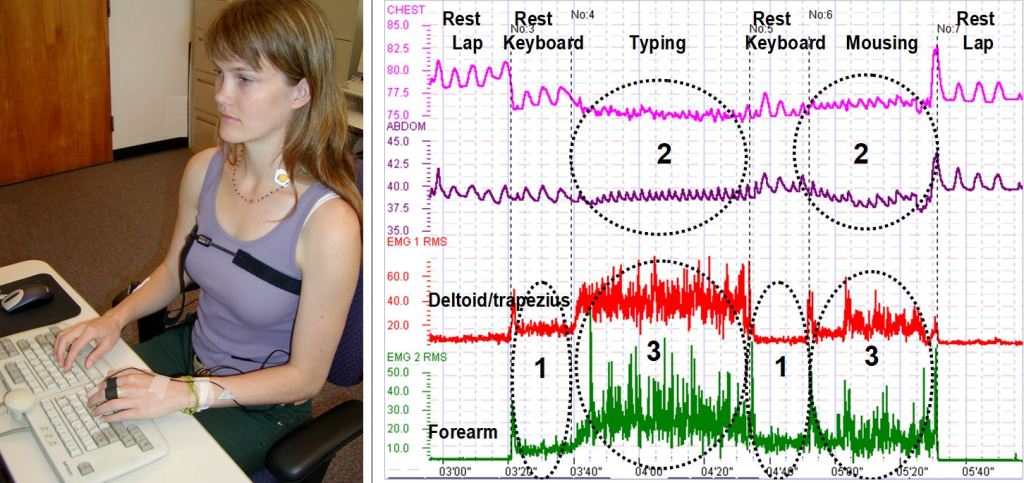
Figure 1. A representative recording of a person working at the computer. Note the following: 1) forearm and shoulder (deltoid/trapezius) muscle tension increased as the person rests her hands on the keyboard without typing; 2) respiration rate increased during typing and mousing; 3) shoulder muscle tension increased during typing and mousing; and, 4) there were no rest periods in the shoulder muscles as long as the fingers are either resting, typing, or mousing. Reproduced by permission from Peper & Harvey, 2008.
Even though the physiological recording showed increase tension when the hands were resting on the keyboard, the person reported being relaxed. The person was also not aware that her neck and shoulder muscles stayed contracted without any momentary rest and recovery periods nor that her breathing rate and heart rate significantly increased. The covert muscle activity and shallow breathing will also interact with the person’s stress level, as well as ergonomic equipment use and the posture throughout the day. Similarly, we tend to be unaware that we slouch which would increase neck and back tension as well as, affect breathing as illustrated in figure 2.
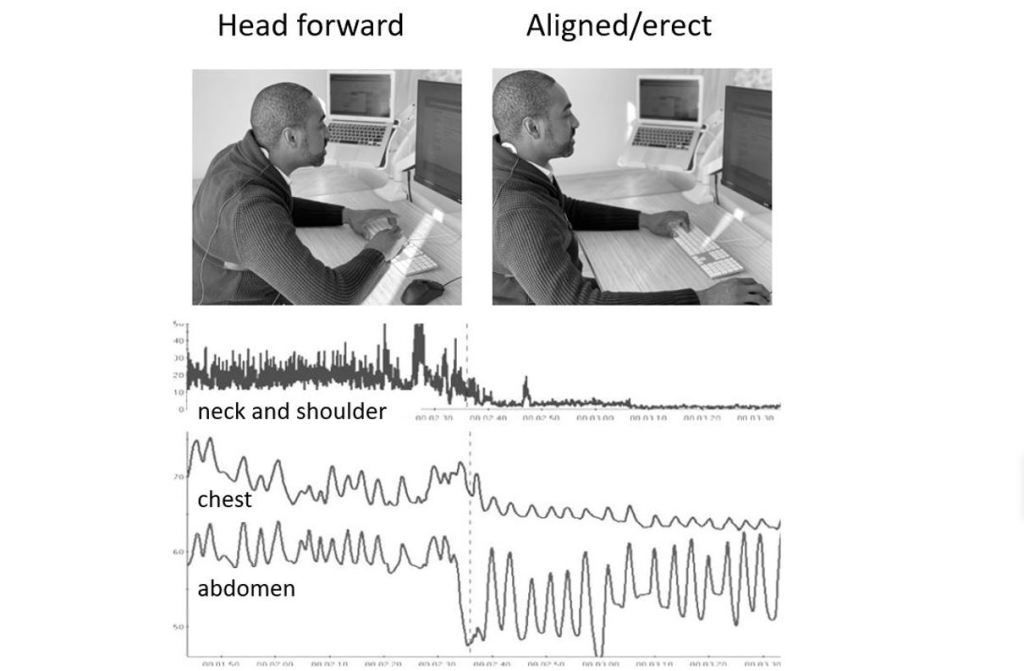
Figure 2. The effect of slouching on neck and shoulder muscle tension and breathing. Reproduced by permission from Peper, E., Harvey, R. and Faass, N. (2020). TechStress-How Technology is Hijacking our Lives, Strategies for Coping and Pragmatic Ergonomics, Berkeley, CA. North Atlantic Books.
Maintaining and optimizing health at the computer means re-envisioning our relationship with technology—reclaiming health, happiness, and sanity in a plugged-in world. We have the ability to control everything from our mobile phones without needing to get up from our seat. Work, social life and online learning all involve the mobile phone or some type of smart devices. A convenient little device that is supposed to simplify our lives has actually trapped us into a vicious cycle of relying on it for every single thing we must do. We spend most of our day being exposed to digital displays on our smartphones, computers, gaming consoles, and other digital devices, immersing ourselves in the content we are viewing. From work related emails or tasks, to spending our free time looking at the screen for texting, playing games, and updating social media sites on a play-by-play of what we are eating, wearing, and doing. A typical thing to do on our devices is to click on one hyperlink after the other and create a vicious cycle in which we are trapped for hours until we realize we need to move. As we do this, we are unaware how much time has frittered away without actually doing anything productive and then, we realize we have wasted another day.
Transform digital fatique into digital health (adapted from https://news.sfsu.edu/news-story/professors-share-tips-healthy-tech-usage-during-pandemic)
Get up and move
About every 20 minutes, stand up and move your body. Consider doing a quick dance to a favorite song or taking a walk around the block. “It will feel silly, yet actively moving is one of the quickest energizers,” Stretching and moving will also relax those muscles that you tense constantly when working at a desk. Think you’ll forget to take a break? Install the free Stretch Break app as a great tool to remind you. For more background information, see the blog, Sitting disease is the new health hazard.
Blink and look far off
Our blinking rate significantly decreases while looking at a screen, which contributes to eye strain. A good way to address this is by blinking every time you click on a hyperlink or after you finish typing a paragraph. To relax the eyes, look at the far distance. “Looking out into the distance disrupts constant near-focus muscle tension in the eyes.” For more suggestions, see the blog, Resolve Eyestrain and Screen Fatigue.
Avoid phones and screens right before bed
Many people use their phones before bed, which can make it more difficult to sleep. Take a break from your phone half an hour or more before bedtime. Electronic screens emit blue light, which can send a signal to your brain that it’s daytime. This suppresses your body’s production of the hormone melatonin, which helps your body know when it’s time to sleep. In addition, keeping up with social media and watching digital media tends to be thought-provoking or anxiety-inducing may stimulate the mind and promote wakefulness. For more suggestions, see the blog, Are LED screens harming you?
Optimize ergonomics
Make sure your computer setup is ergonomically friendly. Your desktop keyboard should be positioned so that your forearms are a few inches above your waist. The top of your screen should be around eyebrow level, which should naturally cause your eyes to look slightly downward at the screen.
Unfortunately, using a laptop or a phone causes people to look down in an unhealthy way that can make them slouch and induce neck or back pain. The solution is to get an external keyboard along with a laptop stand. Getting an external monitor can also help. For more detailed suggestions, see the blogs, Cartoon ergonomics for working at the computer and laptop and Reduce TechStress at Home.
Sit erect and stop slouching
As we work at the computer, we unknowingly tend to slouch which increases the risk of neck and shoulder discomfort and evoking thoughts and feelings. Take control of your slouching with a posture feedback device and app such as UpRight Go [3] that reminds you when you slouch as shown in Figure 3. Each time you the device signals you that you slouch, sit up straight, move, breathe, and think of a positive thought. For more suggestions, see the blog, “Don’t slouch!” Improve health with posture feedback.

Figure 3. Using posture feedback to become aware of slouching. Reproduced by permission from Peper, E., Harvey, R. and Faass, N. (2020). TechStress-How Technology is Hijacking our Lives, Strategies for Coping and Pragmatic Ergonomics, Berkeley, CA. North Atlantic Books.
Practice slow diaphragmatic breathing
Breathe deeply and slowly to restore a natural rhythm. As we work, we tend to breathe more shallowly, which increases anxiety and our heart rate. To counteract this, take three deep breaths for five seconds, then exhale very slowly for six seconds. For more instructions on slower diaphragmatic breathing, see the blog, Healing irritable bowel syndrome with diaphragmatic breathing.
Give undivided attention and be present
Phones have become so ingrained in our lives that we use them constantly throughout the day. Harvey stresses that people should make a conscious effort to limit phone usage, especially when socializing. When we respond to a phone notification during a Zoom hangout with friends or while talking to our family members, people may feel dismissed. This often increases a sense of social isolation, so give people your total attention when interacting with them. For more suggestions, see the blog, Configure your brain to learn and avoid Zoom fatigue.
For detailed information and practices, see the book by Erik Peper, Richard Harvey and Nancy Faass,TechStress-How Technology is Hijacking our Lives, Strategies for Coping and Pragmatic Ergonomics, North Atlantic Press. https://www.amazon.com/Beyond-Ergonomics-Prevent-Fatigue-Burnout/dp/158394768X/

Reduce your risk of COVID-19 variants and future pandemics
Posted: July 5, 2021 Filed under: behavior, health, Nutrition/diet, self-healing | Tags: COVID-19, immune, pandemic, prevention, vitamin D 2 CommentsErik Peper, PhD and Richard Harvey, PhD
The number of hospitalizations and deaths from COVID-19 are decreasing as more people are being vaccinated. At the same time, herd immunity will depend on how vaccinated and unvaccinated people interact with one another. Close-proximity, especially indoor interactions, increases the likelihood of transmission of coronavirus for unvaccinated individuals. During the summer months, people tend to congregate outdoors which reduces viral transmission and also increases vitamin D production which supports the immune system (Holick, 2021)..
Most likely, COVID-19 disease will become endemic because the SARS-CoV-2 virus will continue to mutate. Already Pfizer CEO Albert Bourla stated on April 15, 2021 that people will “likely” need a third dose of a Covid-19 vaccine within 12 months of getting fully vaccinated. Although, at this moment the vaccines are effective against several variants, we need to be ready for the next COVID XX outbreak.
To reduce future infections, the focus of interventions should 1) reduce virus exposure, 2) vaccinate to activate the immune system, and 3) enhance the innate immune system competence. The risk of illness may relate to virus density exposure and depend upon the individual’s immune competence (Gandhi & Rutherford, 2020; Mukherjee, 2020) which can be expressed in the following equation.

Reduce viral load (hazardous exposure)
Without exposure to the virus and its many variants, the risk is zero which is impossible to achieve in democratic societies. People do not live in isolated bubbles but in an interconnected world and the virus does not respect borders or nationalities. Therefore, public health measures need to focus upon strategies that reduce virus exposure by encouraging or mandating wearing masks, keeping social distance, limiting social contact, and increasing fresh air circulation.
Wearing masks reduces the spread of the virus since people may shed viruses one or two days before experiencing symptoms (Lewis et al., 2021). When a person exhales through the mask, a good fitting N95 mask will filter out most of the virus and thereby reduce the spread of the virus during exhalation. To protect oneself from inhaling the virus, the mask needs be totally sealed around the face with the appropriate filters. Systematic observations suggest that many masks such as bandanas or surgical masks do not filter out the virus (Fisher et al., 2020).
Fresh air circulation reduces the virus exposure and is more important than the arbitrary 6 feet separation (CDC, May 13, 2021). If separated by 6 feet in an enclosed space, the viral particles in the air will rapidly increase even when the separation is 10 feet or more. On the other hand, if there is sufficient fresh air circulation, even three feet of separation would not be a problem. The spatial guidelines need to be based upon air flow and not on the distance of separation as illustrated in the outstanding graphical modeling schools by Nick Bartzokas et al. (February 26, 2021) in the New York Times article, Why opening windows is a key to reopening schools.
The public health recommendations of sheltering-in-place to prevent exposure or spreading the virus may also result in social isolation. Thus, shelter-in-place policies have resulted in compromising physical health such as weight gain (e.g. average increase of more than 7lb in weight in America according to Lin et al., 2021), reduced physical activity and exercise levels (Flanagan et al., 2021) and increased anxiety and depression (e.g. a three to four fold increase in the self-report of anxiety or depression according to Abbott, 2021). Increases in weight, depression and anxiety symptoms tend to decrease immune competence (Leonard, 2010). In addition, the stay at home recommendations especially in the winter time meant that individuals are less exposed to sunlight which results in lower vitamin D levels which is correlated with increased COVID-19 morbidity (Seheult, 2020).
Increase immune competence
Vaccination is the primary public health recommendation to prevent the spread and severity of COVID-19. Through vaccination, the body increases its adaptive capacity and becomes primed to respond very rapidly to virus exposure. Unfortunately, as Pfizer Chief Executive Albert Bourla states, there is “a high possibility” that emerging variants may eventually render the company’s vaccine ineffective (Steenhuysen, 2021). Thus, it is even more important to explore strategies to enhance immune competence independent of the vaccine.
Public Health policies need to focus on intervention strategies and positive health behaviors that optimize the immune system capacity to respond. The research data has been clear that COVID -19 is more dangerous for those whose immune systems are compromised and have comorbidities such as diabetes and cardiovascular disease, regardless of age.
Comorbidity and being older are the significant risk factors that contribute to COVID-19 deaths. For example, in evaluating all patients in the Fair Health National Private Insurance Claims (FH NPIC’s) longitudinal dataset, researchers identified 467,773 patients diagnosed with COVID-19 from April 1, 2020, through August 31, 2020. The severity of the illness and death from COVID-19 depended on whether the person had other co-morbidities first as shown in Figure 1.

Figure 1. The distribution of patients with and without a comorbidity among all patients diagnosed with COVID-19 (left) and all deceased COVID-19 patients (right) April-August 2020. Reproduced by permission from: https://www.ajmc.com/view/contributor-links-between-covid-19-comorbidities-mortality-detailed-in-fair-health-study
Each person who died had about 2 or 3 types of pre-existing co-morbidities such as cardiovascular disease, hypertension, diabetes, obesity, congestive heart failure, chronic kidney disease, respiratory disease and cancer (Ssentongo et al., 2020; Gold et al., 2020). The greater the frequency of comorbidities the greater the risk of death, as shown in Figure 2.

Figure 2. Across all age groups, the risk of COVID-19 death increased significantly as a patient’s number of comorbidities increased. Compared to patients with no comorbidities. Reproduced by permission from https://s3.amazonaws.com/media2.fairhealth.org/whitepaper/asset/Risk%20Factors%20for%20COVID-19%20Mortality%20among%20Privately%20Insured%20Patients%20-%20A%20Claims%20Data%20Analysis%20-%20A%20FAIR%20Health%20White%20Paper.pdf
Although the risk of serious illness and death is low for young people, the presence of comorbidity increases the risk. Kompaniyets et al. (2021) reported that for patients under 18 years with severe COVID-19 illness who required ICU admission, mechanical ventilation, or died most had underlying medical conditions such as asthma, neurodevelopmental disorders, obesity, essential hypertension or complex chronic diseases such as malignant neoplasms or multiple chronic conditions.
Consistent with earlier findings, the Fair Health National Private Insurance Claims (FH NPIC’s) longitudinal dataset also showed that the COVID-19 mortality rate rose sharply with age as shown in Figure 3.
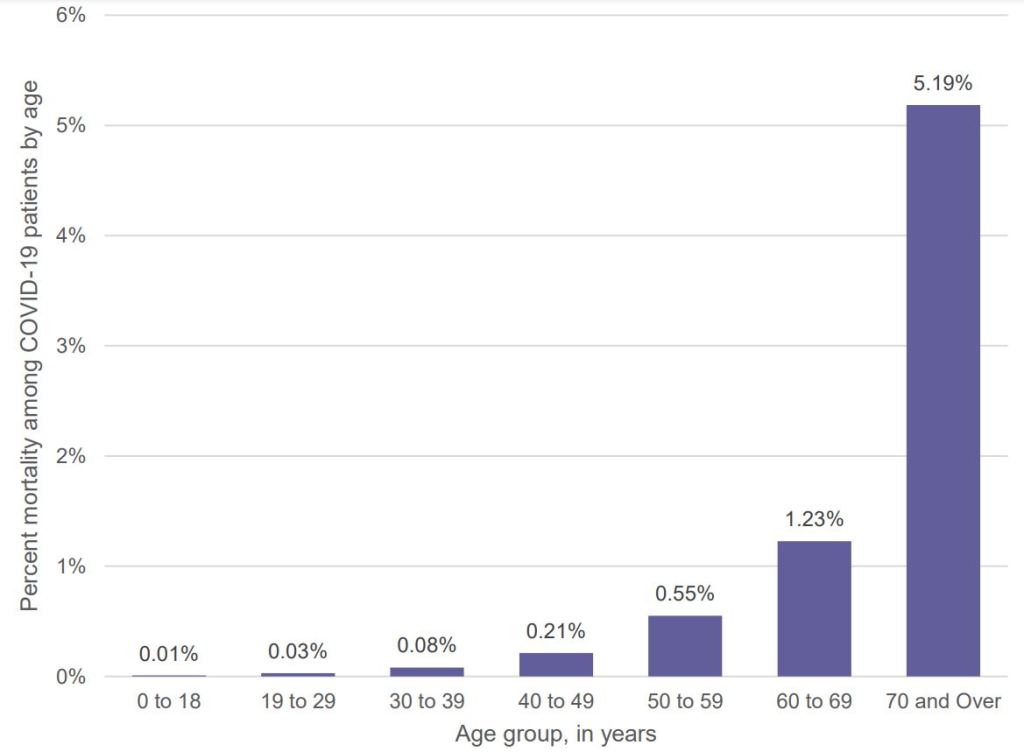
Figure 3 Percent mortality among COVID-19 patients by age, April-August 2020. Reproduced by permission from: https://s3.amazonaws.com/media2.fairhealth.org/whitepaper/asset/Risk%20Factors%20for%20COVID-19%20Mortality%20among%20Privately%20Insured%20Patients%20-%20A%20Claims%20Data%20Analysis%20-%20A%20FAIR%20Health%20White%20Paper.pdf
Optimize antibody response from vaccinations
Assuming that the immune system reacts similarly to other vaccinations, higher antibody response is evoked when the vaccine is given in the morning versus the afternoon or after exercise (Long et al., 2016; Long et al., 2012). In addition, the immune response may be attenuated if the person suppresses the body’s natural immune response–the flulike symptoms which may occur after the vaccination–with Acetaminophen (Tylenol (Graham et al, 1990).
Support the immune system with a healthy life style
Support the immune system by implementing a lifestyle that reduces the probability of developing comorbidities. This means reducing risk factors such as vaping, smoking, immobility and highly processed foods. For example, young people who vape experience a fivefold increase to become seriously sick with COVID-19 (Gaiha, Cheng, & Halpern-Felsher, 2020); similarly, cigarette smoking increases the risk of COVID morbidity and mortality (Haddad, Malhab, & Sacre, 2021).
There are many factors that have contributed to the epidemic of obesity, diabetes, cardiovascular disease and other chronic diseases. In many cases, the environment and lifestyle factors (lack of exercise, excessive intake of highly processed foods, environmental pollution, social isolation, stress, etc.) significantly contribute to the initiation and development of comorbidities. Genetics also is a factor; however, the generic’s risk factor may not be triggered if there are no environmental/behavioral exposures. Phrasing it colloquially, Genetics loads the gun, environment and behavior pulls the trigger. Reducing harmful lifestyle behaviors and environment is not simply an individual’s responsibility but a corporate and governmental responsibility. At present, harmful lifestyles choices are actively supported by corporate and government policies that choose higher profits over health. For example, highly processed foods made from corn, wheat, soybeans, rice are grown by farmers with US government farm subsidies. Thus, many people especially of lower economic status live in food deserts where healthy non-processed organic fruits and vegetable foods are much less available and more expensive (Darmon & Drewnowski, 2008; Michels, Vynckier, Moreno, L.A. et al. 2018; CDC, 2021). In the CDC National Health and Nutrition Examination Survey that analyzed the diet of 10,308 adults, researchers Siegel et al. (2016) found that “Higher consumption of calories from subsidized food commodities was associated with a greater probability of some cardiometabolic risks” such as higher levels of obesity and unhealthy blood glucose levels (which raises the risk of Type 2 diabetes).
Immune competence is also affected by many other factors such as exercise, stress, shift work, social isolation, and reduced micronutrients and Vitamin D (Zimmermann & Curtis, 2019). Even being sedentary increases the risk of dying from COVID as reported by the Kaiser Permanente Southern California study of 50,000 people who developed COVID (Sallis et al., 2021).
People who exercised 10 minutes or less each week were hospitalized twice as likely and died 2.5 times more than people who exercised 150 minutes a week (Sallis et al., 2021). Although exercise tends to enhance immune competence (da Silveira et al, 2020), it is highly likely that exercise is a surrogate marker for other co-morbidities such as obesity and heart disease as well as aging. At the same time sheltering–in-place along with the increase in digital media has significantly reduced physical activity.
The importance of vitamin D
Low levels of vitamin D is correlated with poorer prognosis for patients with COVID-19 (Munshi et al., 2021). Kaufman et al. (2020) reported that the positivity rate correlated inversely with vitamin D levels as shown in figure 4.
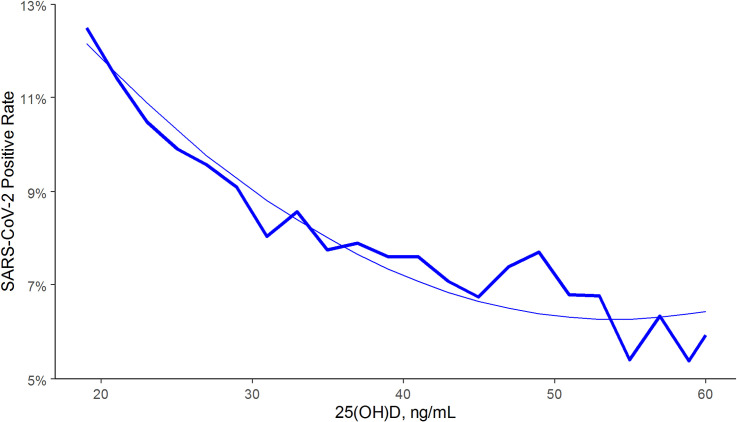
Figure 4. SARS-CoV-2 NAAT positivity rates and circulating 25(OH)D levels in the total population. From: Kaufman, H.W., Niles, J.K., Kroll, M.H., Bi, C., Holick, M.F. (2020). SARS-CoV-2 positivity rates associated with circulating 25-hydroxyvitamin D levels. PLoS One. 15(9):e0239252. https://doi.org/10.1371/journal.pone.0239252
Vitamin D is a modulator for the immune system (Baeke, Takiishi, Korf, Gysemans, & Mathieu, 2010). There is an inverse correlation of all-cause, cardiovascular, cancer, and respiratory disease mortality with hydroxyvitamin D concentrations in a large cohort study (Schöttker et al., 2013). For a superb discussion about how much vitamin D is needed, see the presentation, The D-Lightfully Controversial Vitamin D: Health Benefits from Birth until Death, by Dr. Michael F. Holick, Ph.D., M.D. from the University Medical Center Boston.
Low vitamin D levels may partially explain why in the winter there is an increase in influenza. During winter time, people have reduced sunlight exposure so that their skin does not produce enough vitamin D. Lower levels of vitamin D may be a cofactor in the increased rates of COVID among people of color and older people. The darker the skin, the more sunlight the person needs to produce Vitamin D and as people become older their skin is less efficient in producing vitamin D from sun exposure (Harris, 2006; Gallagher, 2013). Vitamin D also moderates macrophages by regulating the release, and the over-release of inflammatory factors in the lungs (Khan et al., 2021).
Watch the interesting presentation by Professor Roger Seheult, MD, UC Riverside School of Medicine, Vitamin D and COVID 19: The Evidence for Prevention and Treatment of Coronavirus (SARS CoV 2). 12/20/2020. https://www.youtube.com/watch?v=ha2mLz-Xdpg
What can be done NOW to enhance immune competence?
We need to recognize that once the COVID-19 pandemic has passed, it does not mean it is over. It is only a reminder that a new COVID-19 variant or another new virus will emerge in the future. Thus, the government public health policies need to focus on promoting health over profits and aim at strategies to prevent the development of chronic illnesses that affect immune competence. One take away message is to incorporate behavioral medicine prescriptions supporting a healthy lifestyle into treatment plans, such as prescribing a walk in the sun to increase vitamin D production and develop dietary habits of eating organic locally grown vegetable and fruits foods. Even just reducing the refined sugar content in foods and drinks is challenging although it may significantly reduce incidence and prevalence of obesity and diabetes (World Health Organization, 2017. The benefits of such an approach has been clearly demonstrated by the Pennsylvania-based Geisinger Health System’s Fresh Food Farmacy. This program for food-insecure people with Type 2 diabetes and their families provides enough fresh fruits and vegetables, whole grains, and lean proteins for two healthy meals a day five days a week. After one year there was a 40 percent decrease in the risk of death or serious complications and an 80 percent drop in medical costs per year (Brody, 2020).
The simple trope of this article ‘eat well, exercise and get good rest’ and increase your immune competence concludes with some simple reminders.
- Increase availability of organic foods since they do not contain pesticides such as glyphosate residue that reduce immune competence.
- Increase vegetable and fruits and reduce highly processed foods, simple carbohydrates and sugars.
- Decrease sitting and increase movement and exercise
- Increase sun exposure without getting sunburns
- Master stress management
- Increase social support
For additional information see: https://peperperspective.com/2020/04/04/can-you-reduce-the-risk-of-coronavirus-exposure-and-optimize-your-immune-system/
References
Baeke, F., Takiishi, T., Korf, H., Gysemans, C., & Mathieu, C. (2010). Vitamin D: modulator of the immune system,Current Opinion in Pharmacology,10(4), 482-496. https://doi.org/10.1016/j.coph.2010.04.001
Brody, J. (2020). How Poor Diet Contributes to Coronavirus Risk. The New York Times, April 20, 2020. https://www.nytimes.com/2020/04/20/well/eat/coronavirus-diet-metabolic-health.html?referringSource=articleShare
CDC. (2021). Adult Obesity Prevalence Maps. Centers for Disease Control and Prevention. https://www.cdc.gov/obesity/data/prevalence-maps.html#nonhispanic-white-adults
CDC. (May 13, 2021). Ways COVID-19 Spreads. Centers for Disease Control and Prevention. https://www.cdc.gov/coronavirus/2019-ncov/prevent-getting-sick/how-covid-spreads.html
Darmon, N. & Drewnowski, A. (2008). Does social class predict diet quality?, The American Journal of Clinical Nutrition, 87(5), 2008, 1107–1117. https://doi.org/10.1093/ajcn/87.5.1107
da Silveira, M. P., da Silva Fagundes, K. K., Bizuti, M. R., Starck, É., Rossi, R. C., & de Resende E Silva, D. T. (2021). Physical exercise as a tool to help the immune system against COVID-19: an integrative review of the current literature. Clinical and experimental medicine, 21(1), 15–28. https://doi.org/10.1007/s10238-020-00650-3
Elflein, J. (2021). COVID-19 deaths reported in the U.S. as of January 2, 2021, by age. Downloaded, 1/13/2021 from https://www.statista.com/statistics/1191568/reported-deaths-from-covid-by-age-us/
Fisher, E. P., Fischer, M.C., Grass, D., Henrion, I., Warren, W.S., & Westmand, E. (2020). Low-cost measurement of face mask efficacy for filtering expelled droplets during speech. Science Advance, (6) 36, eabd3083. https://doi.org/10.1126/sciadv.abd3083
Flanagan. E.W., Beyl, R.A., Fearnbach, S.N., Altazan, A.D., Martin, C.K., & Redman, L.M. (2021). The Impact of COVID-19 Stay-At-Home Orders on Health Behaviors in Adults. Obesity (Silver Spring), (2), 438-445. https://doi.org/10.1002/oby.23066
Gaiha, S.M., Cheng, J., & Halpern-Felsher, B. (2020). Association Between Youth Smoking, Electronic Cigarette Use, and COVID-19. Journal of Adolescent Health, 67(4), 519-523. https://doi.org/10.1016/j.jadohealth.2020.07.002
Gallagher J. C. (2013). Vitamin D and aging. Endocrinology and metabolism clinics of North America, 42(2), 319–332. https://doi.org/10.1016/j.ecl.2013.02.004
Gandhi, M. & Rutherford, G. W. (2020). Facial Masking for Covid-19 — Potential for “Variolation” as We Await a Vaccine. New England Journal of Medicine, 383(18), e101 https://www.nejm.org/doi/full/10.1056/NEJMp2026913
Gold, M.S., Sehayek, D., Gabrielli, S., Zhang, X., McCusker, C., & Ben-Shoshan, M. (2020). COVID-19 and comorbidities: a systematic review and meta-analysis. Postgrad Med, 132(8), 749-755. https://doi.org/10.1080/00325481.2020.1786964
Graham, N.M., Burrell, C.J., Douglas, R.M., Debelle, P., & Davies, L. (1990). Adverse effects of aspirin, acetaminophen, and ibuprofen on immune function, viral shedding, and clinical status in rhinovirus-infected volunteers. J Infect Dis., 162(6), 1277-82. https://doi.org/10.1093/infdis/162.6.1277
Haddad, C., Malhab, S.B., & Sacre, H. (2021). Smoking and COVID-19: A Scoping Review. Tobacco Use Insights, 14, First Published February 15, 2021. https://doi.org/10.1177/1179173X21994612
Harris, S.S. (2006). Vitamin D and African Americans. The Journal of Nutrition, 136(4), 1126-1129. https://doi.org/10.1093/jn/136.4.1126
Kaufman, H.W., Niles, J.K., Kroll, M.H., Bi, C., Holick, M.F. (2020). SARS-CoV-2 positivity rates associated with circulating 25-hydroxyvitamin D levels. PLoS One. 15(9):e0239252. https://doi.org/10.1371/journal.pone.0239252
Khan, A. H., Nasir, N., Nasir, N., Maha, Q., & Rehman, R. (2021). Vitamin D and COVID-19: is there a role?. Journal of Diabetes & Metabolic Disorders, 1-8. https://doi.org/10.1007/s40200-021-00775-6
Kompaniyets, L., Agathis, N.T., Nelson, J.M., et al. (2021). Underlying Medical Conditions Associated With Severe COVID-19 Illness Among Children. JAMA Netw Open. 4(6):e2111182. https://doi.org/10.1001/jamanetworkopen.2021.11182
Leonard B. E. (2010). The concept of depression as a dysfunction of the immune system. Current immunology reviews, 6(3), 205–212. https://doi.org/10.2174/157339510791823835
Lewis, N. M., Duca, L. M., Marcenac, P., Dietrich, E. A., Gregory, C. J., Fields, V. L….Kirking, H. L. (2021). Characteristics and Timing of Initial Virus Shedding in Severe Acute Respiratory Syndrome Coronavirus 2, Utah, USA. Emerging Infectious Diseases, 27(2), 352-359. https://doi.org/10.3201/eid2702.203517
Long, J.E., Drayson, M.T., Taylor, A.E., Toellner, K.M., Lord, J.M., & Phillips, A.C. (2016). Morning vaccination enhances antibody response over afternoon vaccination: A cluster-randomised trial. Vaccine, 34(24), 2679-85. https://doi.org/10.1016/j.vaccine.2016.04.032.
Long. J.E., Ring, C., Drayson, M., Bosch, J., Campbell, J.P., Bhabra, J., Browne, D., Dawson, J., Harding, S., Lau, J., & Burns, V.E. (2012). Vaccination response following aerobic exercise: can a brisk walk enhance antibody response to pneumococcal and influenza vaccinations? Brain Behav Immun., 26(4), 680-687. https://doi.org/10.1016/j.bbi.2012.02.004
Merelli, A. (2021, February 2). Pfizer’s Covid-19 vaccine is set to be one of the most lucrative drugs in the world. QUARTZ. https://qz.com/1967638/pfizer-will-make-15-billion-from-covid-19-vaccine-sales/
Michels, N., Vynckier, L., Moreno, L.A. et al. (2018). Mediation of psychosocial determinants in the relation between socio-economic status and adolescents’ diet quality. Eur J Nutr, 57, 951–963. https://doi.org/10.1007/s00394-017-1380-8
Mukherjee, S. (2020). How does the coronavirus behave inside a patient? We’ve counted the viral spread across peoples; now we need to count it within people. The New Yorker, April 6, 2020. https://www.newyorker.com/magazine/2020/04/06/how-does-the-coronavirus-behave-inside-a-patient?utm_source=onsite-share&utm_medium=email&utm_campaign=onsite-share&utm_brand=the-new-yorker
Munshi, R., Hussein, M.H., Toraih, E.A., Elshazli, R.M., Jardak, C., Sultana, N., Youssef, M.R., Omar, M., Attia, A.S., Fawzy, M.S., Killackey, M., Kandil, E., & Duchesne, J. (2020) Vitamin D insufficiency as a potential culprit in critical COVID-19 patients. J Med Virol, 93(2), 733-740. https://doi.org/10.1002/jmv.26360
Renoud. L, Khouri, C., Revol, B., et al. (2021) Association of Facial Paralysis With mRNA COVID-19 Vaccines: A Disproportionality Analysis Using the World Health Organization Pharmacovigilance Database. JAMA Intern Med. Published online April 27, 2021. https://doi.org/10.1001/jamainternmed.2021.2219
Sallis, R., Young, D. R., Tartof, S.Y., et al. (2021). Physical inactivity is associated with a higher risk for severe COVID-19 outcomes: a study in 48 440 adult patients. British Journal of Sports Medicine. Published Online First: 13 April 2021. http://dx.doi.org/10.1136/bjsports-2021-104080
Schöttker, B., Haug, U., Schomburg, L., Köhrle, L., Perna, L., Müller. H., Holleczek, B., & Brenner. H. (2013). Strong associations of 25-hydroxyvitamin D levels with all-cause, cardiovascular, cancer and respiratory disease mortality in a large cohort study. American Journal of Clinical Nutrition, 97(4), 782–793 2013; https://doi.org/10.3945/ajcn.112.047712
Siegel, K.R., McKeever Bullard, K., Imperatore. G., et al. (2016). Association of Higher Consumption of Foods Derived From Subsidized Commodities With Adverse Cardiometabolic Risk Among US Adults. JAMA Intern Med. 176(8), 1124–1132. https://doi.org/10.1001/jamainternmed.2016.2410
Ssentongo P, Ssentongo AE, Heilbrunn ES, Ba DM, Chinchilli VM (2020) Association of cardiovascular disease and 10 other pre-existing comorbidities with COVID-19 mortality: A systematic review and meta-analysis. PLoS ONE 15(8): e0238215. https://doi.org/10.1371/journal.pone.0238215
Steenhuysen, J. 2021, Jan 30). Fresh data show toll South African virus variant takes on vaccine efficacy. Accessed January 31, 2021. https://www.reuters.com/article/us-health-coronavirus-vaccines-variant/fresh-data-show-toll-south-african-virus-variant-takes-on-vaccine-efficacy-idUSKBN29Z0I7
World Health Organization. (2017). Sugary drinks1 – a major contributor to obesity and diabetes. WHO/NMH/PND/16.5 Rev. https://apps.who.int/iris/bitstream/handle/10665/260253/WHO-NMH-PND-16.5Rev.1-eng.pdf?sequence=1
Zimmermann, P. & Curtis, N. (2019). Factors That Influence the Immune Response to Vaccination. Clinical Microbiology Reviews, 32(2), 1-50. https://doi.org/10.1128/CMR.00084-18