Hope for dry eyes and eye strain
Posted: March 2, 2026 Filed under: attention, behavior, Breathing/respiration, computer, digital devices, emotions, health, Pain/discomfort, relaxation, screen fatigue, self-healing, stress management, techstress, Uncategorized, vision, zoom fatigue | Tags: behavioral optometry, blinking, digital eye strain, dry eyes, eyes, ophthalmology, optometry, prarasympathetic regulation 1 CommentAdapted from: Peper, E., Yoshino, A., & Harvey, R. Hope for Dry eyes and Eye Strain: How Breathing-Blinking Patterns Influence Dry Eye.
Many times during the day, I let my shoulders and face relax, and with each exhalation I feel the upper eyelids slightly dropping down at the same time as I am relaxing my jaw and mouth while sitting tall. I sense my tongue and throat sinking and feeling an increase in the space between my upper and lower molars. At the same time, I sense my eyes becoming soft and sinking down as my face muscle relax and are pulled down by gravity while sensing a gentle smile. My eyes are not trying to focus on anything. I continue to breathe slowly allowing a pause before inhaling and feel totally safe and at peace. While doing this, I sense moisture at the lower eyelids. After I have inhaled and as I exhale, I slowly open my eyes, and return to my work. My eyes feel slightly moist and as I blink, the eyelids glide smoothly over the corneal surface.
Background
Dry eyes and eye strain are far more common than most people realize. More than 50% of adults in the United States and Europe experience irritated or burning eyes, dryness, eye strain, headaches, tired or heavy eyes, sensitivity to bright light, and general eye discomfort (Wozniak et al., 2025). The prevalence increases with age and is higher among people who smoke, wear contact lenses, or spend excessive time looking at screens—typically more than six hours per day (Uchino et al,, 2013).
Prolonged, intense screen use—often referred to as digital eye strain or computer vision syndrome—occurs when people focus and concentrate, and the muscles involved with near vision contract and do not relax (Chu et al., 2014). During near vision, the ciliary muscles tighten around the lens to allow near focus, and the medial rectus muscles contract to converge the eyes. These muscles stay contracted and only relax when looking into the distance. This ongoing tension and increased sympathetic activation combined with reduced blinking decrease tearing, and contribute to dry eye symptoms because the tears are not able to provide adequate moisture. As a result, the eyes may become irritated, red and inflamed, which increases eye discomfort (Sheppard & Wolffsohn, 2018; Portello et al., 2012; Sheedy et al., 2003).
When someone is vigilant, fearful, or anticipates a threat, sympathetic activation increases (Ranti et al., 2020) and “eye blink are inhibited at precise moments in time so as to minimize the loss of visual information that occurs during a blink. The more important the visual information is to the viewer, the more likely he or she will be to inhibit blinking” (Ranti et al., 2020).
Without being aware, many people are in a chronic state of vigilance and unknowingly are scanning the world for threats to which they must react. Clinically, I often observe this when guiding clients in relaxation. For example, when I give the instruction, “Let me lift your hand,” some clients immediately lift their hand towards me. This nonverbal response suggests that they are constantly vigilant and are monitoring the world around them—always ready to act instead of trusting that they do not have to act and that the world is safe. In most cases, their breathing pattern tends to be shallow and thoracic.
Would it be possible that this ongoing vigilance,which increases sympathetic arousal contributes to the experience of dry eye syndrome? It could be one factor explaining why women have a higher incidence of dry eye disease as well as anxiety than men since the world is often less safe for women, and they breathe more thoracically and less diaphragmatically (abdominally) than men. Shallow chest breathing is also associated with increased in anxiety (Fugl-Meyer, 1974; Mendes et al., 2020; Wilhelm et al., 2001; Banushi eat al., 2023; McLean et al., 2011; Jalnapurkar, et al., 2018).
Note: The risk of dry eye can also be further increased by a wide range of medical conditions and medications, such as diabetes; glaucoma and glaucoma medications; allergies; autoimmune diseases; arthritis; thyroid disease; high cholesterol; acne treatments; antihistamines; antidepressants; and a history of refractive surgery, conjunctival infections, or corneal abrasions. Dry eye also occurs more frequently in women (Mohamed et al., 2024).
What is usually recommended to resolve dry eyes
The primary and effective first-line treatment to reduce the symptoms of dry eye disease is the use of artificial tears (lubricating eye drops) to provide relief (Maity et al., 2025). Another recommendation to reduce eye strain associated with computer use is to implement the 20/20/20 rule developed by the American Optometric Association–take a 20-second break every 20 minutes and look at something 20 feet away (AOA, 2026). Although the 20/20/20 practice can reduce eye strain and momentarily reduce some of the symptoms associated with dry eye disease especially if the eyes are closed, how we orient, breathe and look may contribute to the experience of dry eye discomfort.
Experience how to evoke dry eyes
Sit comfortably, look around, and observe how your eyes feel. Close your eyes. Now imagine there is a threat. Take a very quick gasp through an open mouth by inhaling into your upper chest and keep breathing very shallowly and irregularly. At the same time, open your eyes wide while being vigilant and looking for danger. Simultaneously, tense your body, inclining it slightly backward as if trying to avoid something. Do not blink, as you may miss the potential threat approaching you (adapted from Lemeignan et al., 1990; Bloch, 2017). A sample physiological recording of this pattern is shown in Figure 1.
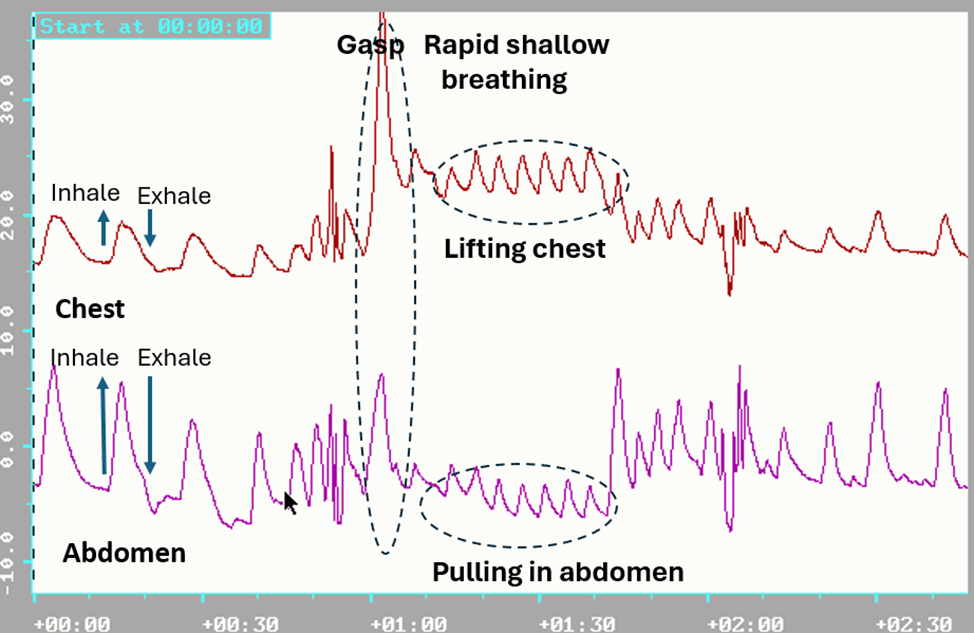
Figure 1. Breathing pattern in response to a threat; a rapid gasp into the chest and pulling the abdomen in to protect while breathing shallowly and rapidly.
Most participants report that almost immediately they feel their eyes getting cooler and after 15 seconds, drier. This facial, breathing, and posture pattern is an exaggeration of the somatic expression of fear that is evoked when we are vigilant and feel unsafe, and it increases sympathetic arousal (Kalawski, 2020).
In most cases, this pattern is automatic, and occurs without awareness, and increases sympathetic activity (Narkiewicz et al., 2006). On the other hand, slow diaphragmatic breathing tends to reduce sympathetic activity (Harada et al., 2014; Lehrer & Gevirtz, 2014). Clinically, the vigilance pattern can often be observed as a person slightly lifts and expands their chest during inhalation and drops and constricts it during exhalation, while breathing shallowly and rapidly without any abdomen expansion or constriction. It is often punctuated with brief breath holding and a reduced blinking rate during concentration.
To investigate these observations more systematically, we compared the practice of gasping while opening the eyes with gentle exhalation while opening the eyes—a pattern that may reduce sympathetic activation and alter the subjective sensation of eye dryness.
Participants: 13 males and 13 females; average age, 39 years
Procedure: While sitting comfortably with their eyes closed, participants were guided through the following two practices:
1.Gasp while opening the eyes
Sit comfortably and look around and observe how your eyes feel. Now close your eyes. Now imagine there is a threat. Take a very quick gasp through an open mouth by inhaling into your upper chest and keep breathing very shallowly and irregularly. At the same time, open your eyes wide while being vigilant and looking for danger. Simultaneously, tense your body, inclining it slightly backward as if trying to avoid something. Do not blink, as you may miss the potential threat approaching you. Repeat three times.
2. Gentle exhalation while opening the eyes
Sit comfortably and look around and observe how your eyes feel. Now close your eyes. Breathe comfortably and inhale by allowing your abdomen to extend and widen while feeling your eyes sinking in their sockets and becoming softer as you gently start exhaling. While gently exhaling, begin to open your eyes very slowly, looking down through your eyelashes without caring what you see, allowing your jaw and face muscles to relax and feeling a slight smile. When you feel the urge to inhale, allow your eyes to close and let your abdomen expand as you inhale slowly. Repeat three times.
After these two practices, the participants filled out a short assessment questionnaire in which they rated how their eyes felt on a scale from -5 (dry), 0 (normal), to 5 (moist/tearing), and rated which eye-opening procedure allowed their eyes to be more relaxed and moist.
Results
92.3% of the participants reported that opening their eyes during exhalation significantly increased eye relaxation and moisture, as shown in Figure 2. A one-way analysis of variance (ANOVA) revealed a significant difference between the inhale condition (M = −0.19, n = 26) and the exhale condition (M = 1.00, n = 25), F(1, 49) = 9.65, p = .003. The experience of eye irritation was correlated (r = 0.64) with the self-rating of experiencing anxiety and fear during the last three months.
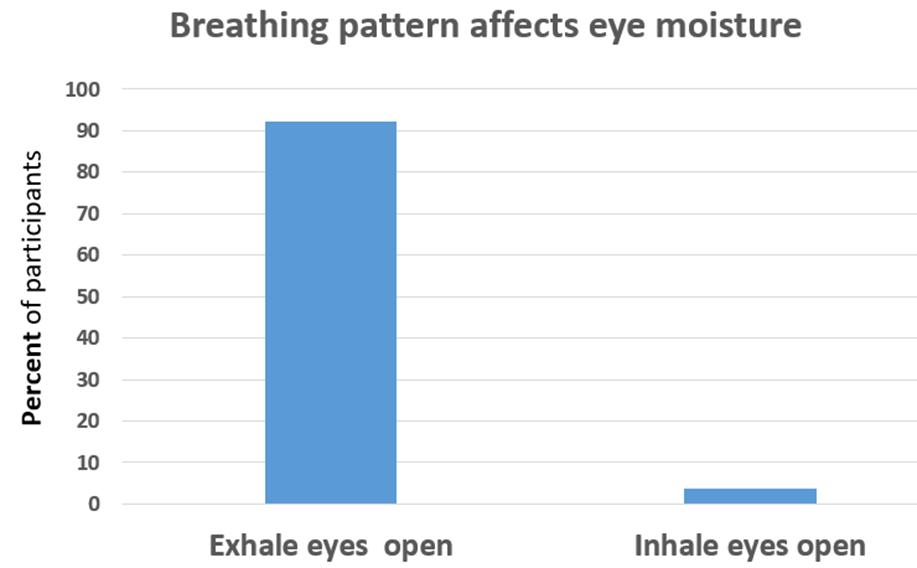
Figure 2. Gently opening the eyes during exhalation increases the experience of moisture and relaxation in the eyes.
Discussion
The results suggest that increased moisture and eye relaxation could be evoked by changing breathing-blinking patterns. Nearly all participants experienced an increase in tearing and eye relaxation; however, long-term benefits most likely occur if the person implements this practice many times during the day. By changing the breathingg-blink pattern and peacefully looking at the world with a smile, one would decrease sympathetic arousal and increase parasympathetic activity. This approach should be taught as the first self-care intervention to reduce eye irritation.
Recommendations to decrease dry eye and improve eye health
- Experience how the two different breathing and eye-opening practices described above affect your eye dryness or moistness.
- When you sense the first onset of minimal eye discomfort or when looking at screens on your computer or cellphone, implement the following practice for about 10 to 15 seconds. Allow your eyelids to close. Be aware of the sensations in your eyes, let your face and jaw relax as if they are being pulled down by gravity while sensing the eyes becoming soft and sinking into their sockets. Breathe diaphragmatically by allowing the abdomen to expand when you inhale. While gently exhaling, slowly open your eyes slightly while looking down with a gentle smile and sensing the moisture beginning to occur in the eyes. Repeat twice.
- During the day, implement the 20/20/20 vision-regeneration practice (every 20 minutes, take a 20-second break and look at something 20 feet away without caring what you see), as shown in Figure 3.
- Read and incorporated the many practices described in the superb book, Vision for Life; Ten Steps to Natural Eye Improvement, by Meir Schneider (2012).

Figure 3. The 20/20/20 rule poster to prevent eye strain (AOA, 2026).
Do these practices many times and be aware of the sensations in your eyes and face. This passive awareness, in conjunction with slower breathing, tends to reduce sympathetic arousal and increase parasympathetic activity, which facilitates increased tearing. As one participant reported when she practiced this:
What a surprise it was when I closed my eyes and breathed slowly and diaphragmatically, and then, as I began to exhale, I very slowly began to open my eyes while looking down and through my eyelashes, while feeling my eyes sink into their sockets. Tearing occurred spontaneously, and my eyes felt lubricated. What a relief. It provided hope that I could help myself instead of only depending on lubricating eye drops whenever my eyes felt dry and irritated.
Two books to maintain and improve vision and reduce techstress
Vision for Life: Ten Steps to Natural Eye Improvement by Meir Schneider (2016) offers many strategies you can immediately incorporate into your daily life to improve and restore your vision. It provides guidelines on how to reverse developing vision issues before they cause damage and how to remedy existing problems, including near- and far-sightedness, lazy eye, as well as more serious conditions such as cataracts, glaucoma, optic neuritis, detached retinas and retinal tears, macular degeneration, and retinitis pigmentosa.

TechStress: How Technology is Hijacking our Lives, Strategies for Coping, and Pragmatic Ergonomics by Erik Peper, Richard Harvey, and Nancy Faass (2020) offers practical tools to avoid the evolutionary traps that trip us up and address the problems associated with technological overuse. It includse effective strategies and practices that individuals can use to optimize their workspace, reduce physical strain, correct posture, and improve vision. It provides fresh insights on reducing stress and enhancing health.

Additional blogs that offer strategies to improve vision
References
AOA. (2026). 20/20/20/ to prevent digital eyes strain. American Optometric Association. https://www.aoa.org/AOA/Images/Patients/Eye%20Conditions/20-20-20-rule.pdf
Banushi, B., Brendle, M., Ragnhildstveit, A., Murphy, T., Moore, C., Egberts, J., & Robison, R. (2023). Breathwork interventions for adults with clinically diagnosed anxiety disorders: A scoping review. Brain Sciences, 13(2), 256. https://doi.org/10.3390/brainsci13020256
Bloch, S. (2017). Alba Emoting: A scientific method for emotional induction. Scotts Valley, CA: CreateSpace Independent Publishing Platform. https://www.amazon.com/Alba-Emoting-Scientific-Emotional-Induction/dp/154254884
Chu, C.A., Rosenfield, M., Portello, J.K. (2014). Blink patterns: reading from a computer screen versus hard copy. Optom Vis Sci., 91(3),297-302. https://doi.org/10.1097/OPX.0000000000000157
Craig, J. P., Nichols, K. K., Akpek, E. K., et al. (2017). TFOS DEWS II definition and classification report. The Ocular Surface, 15(3), 276–283. https://doi.org/10.1016/j.jtos.2017.05.008
Dartt, D. A. (2009). Neural regulation of lacrimal gland secretory processes: Relevance in dry eye diseases. Progress in Retinal and Eye Research, 28(3), 155–177. https://doi.org/10.1016/j.preteyeres.2009.04.003
Fugi-Meyer, A.R. (1974). Relative respiratory contribution of the rib cage and the abdomen in males and females with special regard to posture. Respiration, 31(3), 240–251. https://doi.org/10.1159/000193113
Harada, D., Asanoi, H., Takagawa, J., Ishise, H., Ueno, H., Oda, Y., Goso, Y., Joho, S., & Inoue, H. (2014). Slow and deep respiration suppresses steady-state sympathetic nerve activity in patients with chronic heart failure: from modeling to clinical application. American Journal of Physiology-Heart and Circulatory Physiology, 307(8), H1159–H1168. https://doi.org/10.1152/ajpheart.00109.2014
Jalnapurkar, I., Allen, M., & Pigott, T. (2018). Sex differences in anxiety disorders: A review. Journal of Psychiatry, Depression & Anxiety, 4, 011. https://doi.org/10.24966/PDA-0150/100011
Kalawski, J.P. (2020) The Alba Method and the Science of Emotions. Integr. Psych. Behav. 54, 903–919. https://doi.org/10.1007/s12124-020-09525-4
Lehrer, P. M., & Gevirtz, R. (2014). Heart rate variability biofeedback: How and why does it work? Frontiers in Psychology, 5, Article 756. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4104929/
Lemeignan, M., Guitart, L., & Bloch, S. (1990). Autonomic differentiation of emotional effector pattern of 6 basic emotions. Proceedings of the Fifth International Congress of Psychophysiology, Budapest, July 9–14, 199
Maity, M., Allay, M. B., Ali, M. H., Basu, S., & Singh, S. (2025). Effect of different artificial tears on tear film parameters in dry eye disease. Optometry and Vision Science, 102(1), 37–43. https://doi.org/10.1097/OPX.0000000000002206
McLean, C. P., Asnaani, A., Litz, B. T., & Hofmann, S. G. (2011). Gender differences in anxiety disorders: Prevalence, course of illness, comorbidity and burden of illness. Journal of Psychiatric Research, 45(8), 1027–1035. https://doi.org/10.1016/j.jpsychires.2011.03.006
Mendes, L. P. S., Vieira, D. S. R., Gabriel, L. S., Ribeiro-Samora, G. A., Dornelas de Andrade, A., Brandão, D. C., Goes, M. C., Fregonezi, G. A. F., Britto, R. R., & Parreira, V. F. (2020). Influence of posture, sex, and age on breathing pattern and chest wall motion in healthy subjects. Brazilian Journal of Physical Therapy, 24(3), 240–248. https://doi.org/10.1016/j.bjpt.2019.02.007
Mohamed, Z., Alrasheed, S., Abdu, M., & Allinjawi, K. (2024). Dry eye disease prevalence and associated risk factors among the Middle East population: A systematic review and meta-analysis. Cureus, 16(9), e70522. https://doi.org/10.7759/cureus.70522
Narkiewicz, K., van de Borne, P., Montano, N., Hering, D., Kara, T., & Somers, V. K. (2006). Sympathetic neural outflow and chemoreflex sensitivity are related to spontaneous breathing rate in normal men. Hypertension, 47(1), 51–55. https://doi.org/10.1161/01.HYP.0000197613.47649.0
Peper, E., Harvey, R., & Faass, N. (2020). TechStress: How Technology is Hijacking our Lives, Strategies for Coping, and Pragmatic Ergonomics, North Atlantic Books. https://www.amazon.com/Beyond-Ergonomics-Prevent-Fatigue-Burnout/dp/158394768X
Portello, J.K., Rosenfield, M., Bababekova, Y., et al. (2012). Computer-related visual symptoms in office workers. Ophthalmic and Physiological Optics, 32, 375–82. https://doi.org/10.1111/j.1475-1313.2012.00925.x
Ranti, C., Jones, W., Klin, A. et al. Blink Rate Patterns Provide a Reliable Measure of Individual Engagement with Scene Content. Sci Rep 10, 8267 (2020). https://doi.org/10.1038/s41598-020-64999-x
Schneider, M. (2016). Vision for Life: Ten Steps to Natural Eye Improvement. North Atlantic Books. https://www.amazon.com/Vision-Life-Revised-Eyesight-Improvement/dp/1623170087
Sheedy, J.E., Hayes, J.N., & Engle, J.(2003). Is all asthenopia the same? Optom Vis Sci, 80, 732–9. https://doi.org/10.1097/00006324-200311000-00008
Sheppard, A. L., & Wolffsohn, J. S. (2018). Digital eye strain: prevalence, measurement and amelioration. BMJ open Ophthalmology, 3(1), e000146. https://doi.org/10.1136/bmjophth-2018-000146
Stern, M. E., Gao, J., Siemasko, K. F., Beuerman, R. W., & Pflugfelder, S. C. (2004). The role of the lacrimal functional unit in the pathophysiology of dry eye. Experimental Eye Research, 78(3), 409–416. https://doi.org/10.1016/j.exer.2003.09.003
Swamynathan, S. K., & Wells, A. (2020). Conjunctival goblet cells: Ocular surface functions, disorders that affect them, and the potential for their regeneration. The Ocular Surface, 18(1), 19–26. https://doi.org/10.1016/j.jtos.2019.11.005
Uchino, M., Yokoi, N., Uchino, Y., Dogru, M., Kawashima, M., Komuro, A., Sonomura, Y., Kato, H., Kinoshita, S., Schaumberg, D.A., & Tsubota, K. (2013). Prevalence of Dry Eye Disease and its Risk Factors in Visual Display Terminal Users: The Osaka Study. American Journal of Ophthalmology, 156(4), 759-766.e1, https://doi.org/10.1016/j.ajo.2013.05.040
The epidemiology of dry eye disease: report of the Epidemiology Subcommittee of the International Dry Eye WorkShop (2007). Ocul Surf. , 5(2), 93-107. https://doi.org/10.1016/s1542-0124(12)70082-4
Wilhelm, F. H., Gevirtz, R., & Roth, W. T. (2001). Respiratory dysregulation in anxiety, functional cardiac, and pain disorders: Assessment, phenomenology, and treatment. Behavior Modification, 25(4), 513–545. https://doi.org/10.1177/0145445501254003
Wozniak, P., et al. (2025, September 12–16). Dry eye symptoms, severity, treatment and unmet needs: An analysis of the United States of America and a multinational snapshot (NESTS Study) [Poster presentation]. 43rd Congress of the European Society of Cataract and Refractive Surgeons (ESCRS), Copenhagen, Denmark. https://www.sciencedaily.com/releases/2025/09/250914205829.htm
Ziemssen, F., & Ruprecht, K. W. (2005).Autonomic dysfunction in dry eye syndrome. Ophthalmologe, 102(8), 744–749. https://doi.org/10.1007/s00347-005-1169-1