Reactivate your second heart
Posted: June 14, 2021 Filed under: behavior, computer, digital devices, ergonomics, Evolutionary perspective, Exercise/movement, health, Pain/discomfort, posture, screen fatigue, self-healing, zoom fatigue | Tags: blood clots, blood flow, calf muscle, cardiovascular disease, deep vein thrombosis, edema, exhaustion, Sitting disease, tired legs, Type 2 diabetes 6 CommentsMonica Almendras and Erik Peper
Adapted from: Almendras, M. & Peper, E. (2021). Reactivate your second heart. Biofeedback, 49(4), 99-102. https://doi.org/10.5298/1081-5937-49.04.07
Have you ever wondered why after driving long distances or sitting in a plane for hours your feet and lower leg are slightly swollen (Hitosugi, Niwa, & Takatsu, 2000)? It is the same process by which soldiers standing in attention sometimes faint or why salespeople or cashiers, especially those who predominantly stand most of the day, have higher risk of developing varicose veins. By the end of the day, they feel that their legs being heavy and tired? In the vertical position, gravity is the constant downward force that pools venous blood and lymph fluid in the legs. The pooling of the blood and reduced circulation is a contributing factor why airplane flights of four or more hours increases the risk for developing blood clots-deep vein thrombosis (DVT) (Scurr, 2002; Kuipers et al., 2007). When blood clots reaches the lung, they can cause a pulmonary embolisms that can be fatal. In other cases, they may even travel to the brain and cause strokes.[1]
Sitting without moving the leg muscles puts additional stress on your heart, as the blood and lymph pools in the legs. Tightening and relaxing the calf muscles can prevent the pooling of the blood. The inactivity of your calf muscles does not allow the blood to flow upwards. The episodic contractions of the calf muscles squeezes the veins and pumps the venous blood upward towards the heart as illustrated in figure 1. Therefore, it is important to stand, move, and walk so that your calf muscle can act as a second heart (Prevosti, April 16, 2020).

Figure 1. Your calf muscles are your second heart! The body is engineered so that when you walk, the calf muscles pump venous blood back toward your heart. Reproduced by permission from Dr. Louis Prevosti of the Center for Vein Restoration (https://veinatlanta.com/your-second-heart/).
To see the second heart in action watch the YouTube video, Medical Animation Movie on Venous Disorders, by the Sigvaris Group Europe (2017).
If you stand too long and experienced slight swelling of the legs, raise your feet slightly higher than the head, to help drain the fluids out of the legs. Another way to reduce pooling of fluids and prevent blood clots and edema is to wear elastic stockings or wrap the legs with intermittent pneumatic compression (IPC) devices that periodically compresses the leg (Zhao et al., 2014). You can also do this by performing foot rotations or other leg and feet exercises. The more the muscle of the legs and feet contract and relax, the more are the veins episodically compressed which increases venous blood return. Yet in our quest for efficiency and working in front of screens, we tend to sit for long time-periods.
Developing sitting disease
Have you noticed how much of the time you sit during the day? We sit while studying, working, socializing and entertaining in front of screens. This sedentary behavior has significantly increased during the pandemic (Zheng et al, 2010). Today, we do not need to get up because we call on Amazon’s Alexa, Apple’s Siri or Google’s Hey Google to control timers, answer queries, turn on the lights, fan, TV, and other home devices. Everything is at our fingertips and we have finally become The Jetsons without the flying cars (an American animated sitcom aired in the 1960s). There is no need to get up from our seat to do an activity. Everything can be controlled from the palm of our hand with a mobile phone app.
With the pandemic, our activities involve sitting down with minimum or no movement at all. We freeze our body’s position in a scrunch–a turtle position–and then we wonder why we get neck, shoulder, and back pains–a process also observed in young adults or children. Instead of going outside to play, young people sit in front of screens. The more we sit and watch screens, the poorer is our mental and physical health (Smith et al., 2020; Matthews et al., 2012). We are meant to move instead of sitting in a single position for eight or more hours while fixating our attention on a screen.
The visual stimuli on screen captures our attention, whether it is data entry, email, social media, or streaming videos (Peper, Harvey & Faass, 2020). While at the computer, we often hold up our index finger on the mouse and wait with baited breath to react. Holding this position and waiting to click may look harmless; however, our right shoulder is often elevated and raised upward towards our ear. This bracing pattern is covert and contributes to the development of discomfort. The moment your muscles tighten, the blood flow through the muscle is reduced (Peper, Harvey, & Tylova, 2006). Muscles are most efficient when they alternately tighten and relax. It is no wonder that our body starts to scream for help when feeling pain or discomfort on our neck, shoulders, back and eyes.
Why move?

Figure 2a and 2b Move instead of sit (photos source: Canva.com).
The importance of tightening and then relaxing muscles is illustrated during walking. During the swing phase of walking, the hip flexor muscles relax, tighten, relax again, tighten again, and this is repeated until the destination is reached. It is important to relax the muscles episodically for blood flow to bring nutrients to the tissue and remove the waste product. Most people can walk for hours; however, they can only lift their foot from the floor (raise their leg up for a few minutes) till discomfort occurs.
Movement is what we need to do and play is a great way to do it. Dr. Joan Vernikos (2016) who conducted seminal studies in space medicine and inactivity physiology investigated why astronauts rapidly aged in space and lost muscle mass, bone density and developed a compromised immune system. As we get older, we are hooked on sitting, and this includes the weekends too. If you are wondering how to separate from your seat, there are ways to overcome this. In the research to prevent the deterioration caused by simulating the low gravity experience of astronauts, Dr. Joan Vernikos (2021) had earthbound volunteers lie down with the head slightly lower than the feet on a titled bed. She found that standing up from lying down every 30-minutes was enough to prevent the deterioration of inactivity, standing every hour was not enough to reverse the degeneration. Standing stimulated the baroreceptors in the neck and activated a cardiovascular response for optimal health (Vernikos, 2021).
We have forgotten something from our evolutionary background and childhood, which is to play and move around. When children move around, wiggle, and contort themselves in different positions, they maintain and increase their flexibility. Children can jump and move their arms up, down, side to side, forward, and backward. They do this every day, including the weekends.
When was the last time you played with a child or like a child? As an adult, we might feel tired to play with a child and it can be exhausting after staring at the screen all day. Instead of thinking of being tired to play with your child, consider it as a good workout. Then you and your child bond and hopefully they will also be ready for a nap. For you, not only do you move around and wake up those muscles that have not worked all day, you also relax the tight muscles, stretch and move your joints. Do playful activities that causes the body to move in unpredictable fun ways such as throwing a ball or roleplaying being a different animal. It will make both of you smile–smiling helps relaxation and rejuvenates your energy.
It is not how much exercise you do, it is how long you sit. The longer you sit without activating your second heart the more are you at risk for cardiovascular disease and diabetes independent of how much exercise you do (Bailey et al., 2019).
Use it or lose it! Activate your calves!
- Interrupt sitting at your desk/computer every 30-minutes by getting up and walking around.
- Stand up and walk around when using your phone.
- Organize walking meetings instead of sitting around a table.
- Invest in a sit-stand desk while working at the computer. While working, alternate positions. There should be a balance between standing and sitting, because too much of one can lead to problems. By taking a short standing up break to let your blood pump back to the heart is beneficial to avoid health problems. Exercise alone, a fancy new ergonomic chair or expensive equipment is not enough to be healthy, it is important to add those mini breaks in between (Buckley et al, 2015).
For a holistic perspective to stay healthy while working with computers and cellphones, see the comprehensive book by Peper, Harvey and Faass (2020), TechStress: How Technology is Hijacking Our Lives, Strategies for Coping, and Pragmatic Ergonomics.
References
Buckley, J.P., Hedge, A., Yates, T., et al. (2015). The sedentary office: an expert statement on the growing case for change towards better health and productivity British Journal of Sports Medicine, 49, 1357-1362.
Prevosti, L. (2020, April 16). Your second heart. https://veinatlanta.com/your-second-heart/
Vernikos, J. (2021, February 25). Much ado about standing. Virtual Ergonomic Summit. American Posture Institute. https://api.americanpostureinstitute.com/virtual-ergonomics-summit-free-ticket?r_done=1
[1] We even wonder if excessive sitting during the COVID-19 pandemic is a hidden risk factor of the rare negative side effects of blood clots in the brain, that can occur with the AstraZeneca and Johnson and Johnson coronavirus vaccine (Mahase, 2021).
Simple acts of kindness
Posted: December 29, 2020 Filed under: behavior, emotions, health, mindfulness, self-healing, stress management | Tags: kindness 1 CommentAs we emerge from the COVID pandemic and look forward to the New Year, we can bring joy and happiness though through simple acts of kindness.
There is hope in these crazy times—three inspirational TED talks
Posted: December 16, 2020 Filed under: behavior, emotions, health, mindfulness, self-healing, Uncategorized | Tags: hope, racial bias, resilience 2 CommentsI just received an email from the Rick Hansen Foundation that inspired me to share its recommendations. In 1957 at the age of 15, Rick Hansen injured his spinal cord and was paralyzed from the waist down. He is an inspiration for all of us. In these crazy times of sheltering in place, experiencing social isolation, anxiety, depression, racial bias, and also happiness and joy, he recommends the following TED talks to increase resilience, overcome racial bias, and achieve self-acceptance. Enjoy watching the talks as they suggest strategies to deal with adversity and offer hope for the New Year.
3 Secrets of resilient people by Dr. Lucy Hone, Co-director of the New Zealand Institute of Wellbeing & Resilience and adjunct fellow at the University of Canterbury in Christchurch, New Zealand.
How racial bias works-and how to disrupt it by Stanford University social psychologist, Jennifer L. Eberhardt
To overcome challenges, stop comparing yourself to other by wheelchair athlete Dean Furnes
Tips to Reduce Zoom Fatigue
Posted: November 15, 2020 Filed under: behavior, computer, digital devices, ergonomics, Exercise/movement, health, laptops, Neck and shoulder discomfort, Pain/discomfort, self-healing, stress management, Uncategorized, vision 1 CommentAdapted from the book, TechStress: How Technology
is Hijacking our Lives, Strategies for Coping and Pragmatic Ergonomics, by Erik Peper, Richard Harvey and Nancy Faass.






Peper, E., Harvey, R., & Faass, N. (2020), TechStress-How Technology is Hijacking our Lives, Strategies for Coping and Pragmatic Ergonomics. Berkeley, CA: North Atlantic Books.
Ways to reduce TechStress
Posted: August 13, 2020 Filed under: ADHD, behavior, computer, digital devices, emotions, ergonomics, Evolutionary perspective, Exercise/movement, health, Neck and shoulder discomfort, Nutrition/diet, Pain/discomfort, posture, relaxation, self-healing, stress management, Uncategorized 5 CommentsWe are excited about our book, TechStress-How Technology is Hijacking our Lives, Strategies for Coping and Pragmatic Ergonomics, that was published August 25, 2020.

Evolution shapes behavior — and as a species, we’ve evolved to be drawn to the instant gratification, constant connectivity, and the shiny lights, beeps, and chimes of our ever-present devices. In earlier eras, these hardwired evolutionary patterns may have set us up for success, but today they confuse our instincts, leaving us vulnerable and stressed out from fractured attention, missed sleep, skipped meals, aches, pains, and exhaustion and often addicted to our digital devices.
Tech Stress offers real, practical tools to avoid evolutionary pitfalls programmed into modern technology that trip us up. You will find a range of effective strategies and best practices to individualize your workspace, reduce physical strain, prevent sore muscles, combat brain drain, and correct poor posture. The book also provides fresh insights on reducing psychological stress on the job, including ways to improve communication with coworkers and family.
Although you will have to wait to have the book delivered to your home, you can already begin to implement ways to reduce physical discomfort, zoom/screen fatigue and exhaustion. Have a look the blogs below.
How evolution shapes behavior
How to optimize ergonomics
Cartoon ergonomics for working at the computer and laptop
Hot to prevent and reduce neck and shoulder discomfort
Why do I have neck and shoulder discomfort at the computer?
Relieve and prevent neck stiffness and pain
How to prevent screen fatigue and eye discomfort
Resolve Eyestrain and Screen Fatigue
How to improve posture and prevent slouching
“Don’t slouch!” Improve health with posture feedback
How to improve breathing and reduce stress
Anxiety, lightheadedness, palpitations, prodromal migraine symptoms? Breathing to the rescue!
How to protect yourself from EMF
Cell phone radio frequency radiation increases cancer risk

Available from: https://www.penguinrandomhouse.com/books/232119/tech-stress-by-erik-peper-phd/
Do nose breathing FIRST in the age of COVID-19
Posted: May 30, 2020 Filed under: Breathing/respiration, health, self-healing, Uncategorized | Tags: anxiety, COVID-19, HRV, nasal breathing, respiration 4 Comments
Breathing affects every cell of our body and should be the first intervention strategy to improve physical and mental well-being (Peper & Tibbetts, 1994). Breathing patterns are much more subtle than indicated by the respiratory function tests (spirometry, lung capacity, airway resistance, diffusing capacity and blood gas analysis) or commonly monitored in medicine and psychology (breathing rate, tidal volume, peak flow, oxygen saturation, end-tidal carbon dioxide) (Gibson, Loddenkemper, Sibille & Lundback, 2019).
When a person feels safe, healthy and peaceful, the breathing is effortless and the breath flows in and out of the nose without awareness. Functional and dysfunctional breathing patterns includes an assessment of the whole body pattern by which breathing occurs such as nose versus mouth breathing, alternation of nasal patency, the rate of air flow rate during inhalation and exhalation, the length of time during inhalation and exhalation, the post exhalation pause time. the pattern of transition between inhaling and exhaling, the location and timing of expansion in the truck, the range of diaphragmatic movement, and the subjective quality of breathing effort (Gilbert, 2019; Peper, Gilbert, Harvey & Lin, 2015; Nestor, 2020).
Breathing patterns affect sympathetic and parasympathetic nervous systems (Levin & Swoap, 2019). Inhaling tends to activate the sympathetic nervous system (fight/flight response) while exhaling activates the parasympathetic nervous system (rest and repair response) (Lehrer & Gevirtz, 2014). To observe how breathing affects your heart rate, monitor your pulse from either the radial artery in the wrist or the carotid artery in your neck as shown in Figure 1 and practice the following.
After sensing the baseline rate of your pulse, continue to feel your radial artery pulse in your wrist or at the carotid artery in your neck. Then inhale for the count of four hold for a moment and gently exhale for the count of 5 or 6. Repeat two or three times.
Most people observe that during inhalation, their heart rate increased (sympathetic activation for action) and during exhalation, the heart rate decreases (restoration during safety).
Nearly everyone who is anxious tends to breathe rapidly and shallowly or when stressed, unknowingly gasp or holds their breath–they may even freeze up and blank out (Peper et al, 2016). In addition, many people habitually breathe through their mouth instead of their nose and wake up tired with a dry mouth with bad breath. Mouth breathing combined with chest breathing in the absence of slower diaphragmatic breathing (the lower ribs and abdomen expand during inhalation and constrict during exhalation) is a risk factor for disorders such as irritable bowel syndrome, hypertension, tiredness, anxiety, panic attacks, asthma, dysmenorrhea, epilepsy, cold hands and feet, emphysema, and insomnia. Many of our clients who aware of their dysfunctional breathing patterns and are able to implement effortless breathing report significant reduction in symptoms (Chaitow, Bradley, & Gilbert, 2013; Peper, Mason, Huey, 2017; Peper & Cohen, 2017; Peper, Martinez Aranda, & Moss, 2015).
Breathing is usually overlooked as a first treatment strategy-it is not as glamorous as drugs, surgery or psychotherapy. Teaching breathing takes skill since practitioners needs to be experienced. Namely, they need to be able to demonstrate in action how to breathe effortlessly before teaching it to others. Although it seems unbelievable, a small change in our breathing pattern can have major physical, mental, and emotional effects as can be experienced in the following practice.
Begin by breathing normally and then exhale only 70% of the inhaled air, and inhale normally and again exhale only 70% of the inhaled air. With each exhalation exhale on 70% of the inhaled air. Continue this for 30 seconds. Stop and note how you feel.
Almost every reports that the 30 seconds feels like a minute and experience some of the following symptoms listed in table 1.
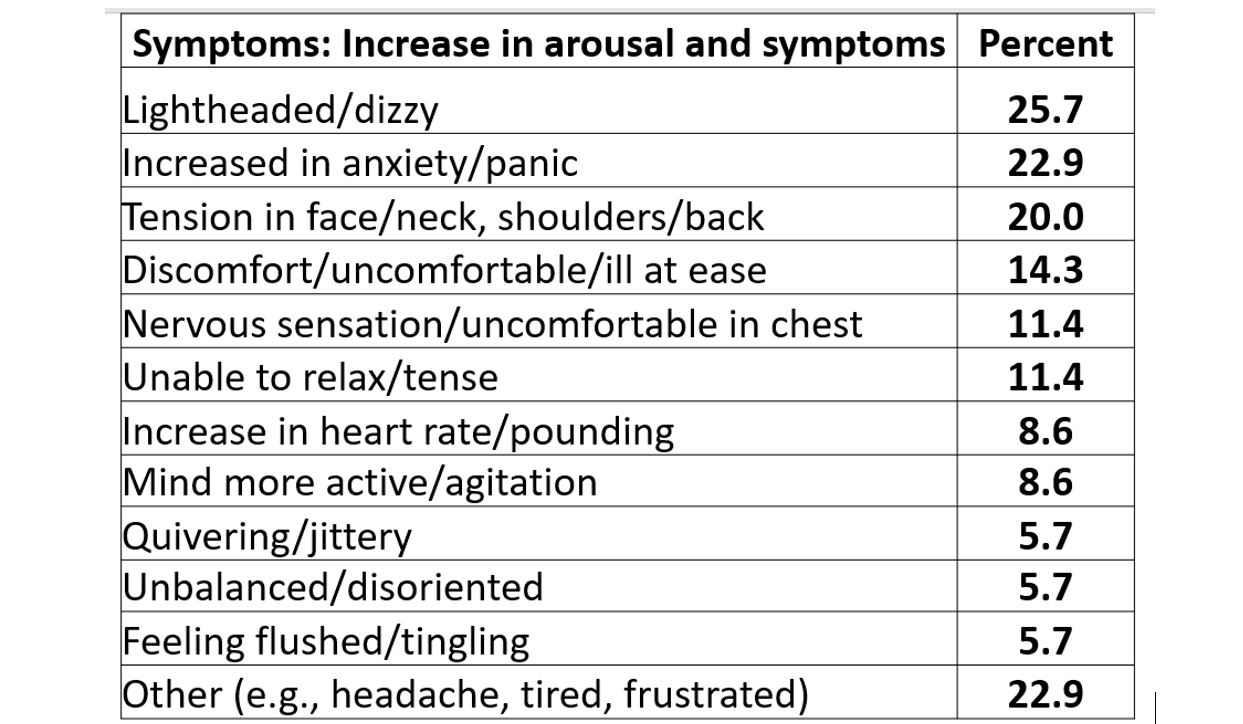
Table 1. Symptoms experienced after 30-45 seconds of sequentially exhaling 70% percent of the inhales air (Peper & MacHose, 1993).
Even though many therapists have long pointed out that breathing is essential, it is usually the forgotten ingredient. It is now being rediscovered in the age of the COVID-19 as respiratory health may reduce the risk of COVID-19.
Simply having very sick patients lie on their side or stomach can improve gas exchange. By lying on your side or prone, breathing is easier as the lung can expand more which appears to reduce the utilization of respirators and intubation (Long & Singh, 2020; Farkas, 2020). This side or prone breathing approach is thousands of years old.
One of the natural and health promoting breathing patterns to promote lung health is to breathe predominantly through the nose. The nose filters, warms, moisturizes and slows the airflow so that airway irritation is reduced. Nasal breathing also increases nitric oxide production that significantly increases oxygen absorption in the body. More importantly for dealing with COVID-19, nitric oxide, produced and released inside the nasal cavities and the lining of the blood vessels, acts as an anti-viral and is a secondary strategy to protect against viral infections (Mehta, Ashkar & Mossman, 2012). During inspiration through the nose, the nitric oxide helps dilate the airways in your lungs and blood vessels (McKeown, 2016).
To increase your health, breathe through your nose, yes, even at night (McKeown, 2020). As you practice this during the day be sure that the lower ribs and abdomen expand during inhalation and decrease in diameter during exhalation. It is breathing without effort although many people will report that it initially feels unnatural. Exhale to the count of about 5 or 6 and inhale (allow the air to flow in) to the count of 4 or 5. Mastering nasal breathing takes practice, practice and practice. See the following for more information.
Watch the Youtube presentation by Patrick McKeown author of the Oxygen Advantage, Practical 40 minute free breathing session with Patrick McKeown to improve respiratory health. https://www.youtube.com/watch?v=AiwrtgWQeDc&t=680s
Listen to Terry Gross interviewing James Nestor on “How The ‘Lost Art’ Of Breathing Can Impact Sleep And Resilience” on May 27, 2020 on the NPR radio show, Fresh Air.
Look at the Peperperspective blogs that focus on breathing in the age of Covid-19.
Read science writer James Nestor’s book, Breath The new science of a lost art, Breath The new science of a lost art.

References
Allen, R. (2017).The health benefits of nose breathing. Nursing in General Practice.
Christopher, G. (2019). A Guide to Monitoring Respiration. Biofeedback, 47(1), 6-11.
Farkas, J. (2020). PulmCrit – Awake Proning for COVID-19. May 5, 2020.
Long, L. & Singh, S. (2020). COVID-19: Awake Repositioning / Proning. EmDocs
McKeown, P. (2016). Oxygen advantage. New York: William Morrow.
Nestor, James. (2020). Breath The new science of a lost art. New York: Riverhead Books
Can changing your breathing pattern reduce coronavirus exposure?
Posted: April 1, 2020 Filed under: Breathing/respiration, health, relaxation, self-healing, Uncategorized | Tags: coronavirus, COVID-19 9 Comments
This blog is based upon our breathing research that began in the 1990s, This research helped identify dysfunctional breathing patterns that could contribute to illness. We developed coaching/teaching strategies with biofeedback to optimize breathing patterns, improve health and performance (Peper and Tibbetts, 1994; Peper, Martinez Aranda and Moss, 2015; Peper, Mason, and Huey, 2017).
For example, people with asthma were taught to reduce their reactivity to cigarette smoke and other airborne irritants (Peper and Tibbitts, 1992; Peper and Tibbetts, 2003). The smoke of cigarettes or vaping spreads out as the person exhales. If the person was infected, the smoke could represent the cloud of viruses that the other people would inhale as is shown in Figure 1.
Figure 1. Vaping by young people in Riga, Latvia (photo by Erik Peper).
To learn how to breathe differently, the participants first learned effortless slow diaphragmatic breathing. Then were taught that the moment they would become aware of an airborne irritant such as cigarette smoke, they would hold their breath and relax their body and move away from the source of the polluted air while exhaling very slowly through their nose. When the air was clearer they would inhale and continue effortless diaphragmatically breathing (Peper and Tibbetts, 1994). From this research we propose that people may reduce exposure to the coronavirus by changing their breathing pattern; however, the first step is prevention by following the recommended public health guidelines.
- Social distancing (physical distancing while continuing to offer social support)
- Washing your hands with soap for at least 20 seconds
- Not touching your face
- Cleaning surfaces which could have been touched by other such as door bell, door knobs, packages.
- Wear a mask to protect other people and your community. The mask will reduce the shedding of the virus to others by people with COVID-19 or those who are asymptomatic carriers.
Reduce your exposure to the virus when near other people by changing your breathing pattern
Normally when startled or surprised, we tend to gasp and inhale air rapidly. When someone sneezes, coughs or exhales near you, we often respond with a slight gasp and inhale their droplets. To reduce inhaling their droplets (which may contain the coronavirus virus), implement the following:
- When a person is getting too close
- Hold your breath with your mouth closed and relax your shoulders (just pause your breathing) as you move away from the person.
- Gently exhale through your nose (do not inhale before exhaling)-just exhale how little or much air you have
- When far enough away, gently inhale through your nose.
- Remember to relax and feel your shoulders drop when holding your breath. It will last for only a few seconds as you move away from the person. Exhale before inhaling through your nose.
- When a person coughs or sneezes
- Hold your breath, rotate you head away from the person and move away from them while exhaling though your nose.
- If you think the droplets of the sneeze or cough have landed on you or your clothing, go home, disrobe outside your house, and put your clothing into the washing machine. Take a shower and wash yourself with soap.
- When passing a person ahead of you or who is approaching you
- Inhale before they are too close and exhale through your nose as you are passing them.
- After you are more than 6 feet away gently inhale through your nose.
- When talking to people outside
- Stand so that the breeze/wind hits both people from the same side so that the exhaled droplets are blown away from both of you (down wind).
These breathing skills seem so simple; however, in our experience with people with asthma and other symptoms, it took practice, practice, and practice to change their automatic breathing patterns. The new pattern is pause (stop) the breath and then exhale through your nose. Remember, this breathing pattern is not forced and with practice it will occur effortlessly.
The following blogs offer instructions for mastering effortless diaphragmatic breathing.
https://peperperspective.com/2018/10/04/breathing-reduces-acid-reflux-and-dysmenorrhea-discomfort/
https://peperperspective.com/2017/03/19/enjoy-sex-breathe-away-the-pain/
https://peperperspective.com/2015/02/18/reduce-hot-flashes-and-premenstrual-symptoms-with-breathing/
https://peperperspective.com/2015/09/25/resolving-pelvic-floor-pain-a-case-report/
References
Peper, E., Mason, L., Huey, C. (2017). Healing irritable bowel syndrome with diaphragmatic breathing. Biofeedback. (45-4). /
Life has choices
Posted: December 29, 2019 Filed under: emotions, health, self-healing, Uncategorized | Tags: hospice 4 CommentsWhen you woke up this morning, how did you feel? Were you looking forward to the day anticipating with joy what would occur or were you dreading the day as if once again you had to step on the treadmill of life?

Whenever I ask this question of college students in their junior or senior year at an urban university about 20% will answer that they are looking forward to the day. The majority answer, “Well not really”, or even “Oh shit, another day”. For many students the burden of working 40 plus hours a week to pay for rent and tuition, worrying about financial debt, the challenge of commuting, and finding time to do the homework is overwhelming. Focusing on quality of life is not only a challenge for students, but for all of us.
Each day ask yourself, “Am I looking forward to my day and my activities?” If the answer is “No,” begin to explore new options. Ask yourself, “What would I like to do? Start to explore and imagine new options and then begin to plan how to implement them so that you are on the path to where you want to be.
Creating a worthwhile life is an ongoing challenge. An inspiring essay by Steven James articulates this by exploring factors that contribute to sickness and health during the height of the AIDs epidemic. He outline rules that contribute to 1) how to get sick, 2) how to get sicker (if you are already sick), and 3) how to stay well (or get better, if you are not so well to begin with).
| Steven James’s Totally Subjective, Nonscientific Guide to Illness and Health: Ten-Step Programs
How to Get Sick · Don’t pay attention to your body. Eat plenty of junk food, drink too much, take drugs, have lots of unsafe sex with lots of different partners—and, above all, feel guilty about it. If you are overstressed and tired, ignore it and keep pushing yourself. · Cultivate the experience of your life as meaningless and of little value. · Do the things you don’t like, and avoid doing what you really want. Follow everyone else’s opinions and advice, while seeing yourself as miserable and “stuck.” · Be resentful and hypercritical, especially toward yourself. · Fill your mind with dreadful pictures, and then obsess over them. Worry most, if not all, of the time. · Avoid deep, lasting, intimate relationships. · Blame other people for all your problems. · Do not express your feelings and views openly and honestly. Other people wouldn’t appreciate it. If at all possible, do not even know what your feelings are. · Shun anything that resembles a sense of humor. Life is no laughing matter! · Avoid making any changes that would bring you greater satisfaction and joy. How to Get Sicker (If You’re Already Sick) · Think about all the awful things that could happen to you. Dwell upon negative, fearful images. · Be depressed, self-pitying, envious, and angry. Blame everyone and everything for your illness. · Read articles, books, and newspapers, watch TV programs, surf the net, and listen to people who reinforce the viewpoint that there is NO HOPE. You are powerless to influence your fate. · Cut yourself off from other people. Regard yourself as a pariah. Lock yourself up in your room and contemplate death. · Hate yourself for having destroyed your life. Blame yourself mercilessly and incessantly. · Go to see lots of different doctors. Run from one to another, spend half your time in waiting rooms, get lots of conflicting opinions and lots of experimental drugs, starting one program after another without sticking to any. · Quit your job, stop work on any projects, give up all activities that bring you a sense of purpose and fun. See your life as essentially pointless, and at an end. · Complain about your symptoms, and if you associate with anyone, do so exclusively with other people who are unhappy and embittered. Reinforce each other’s feelings of hopelessness. · Don’t take care of yourself. What’s the use? Try to get other people to do it for you, and then resent them for not doing a good job. · Think how awful life is, and how you might as well be dead. But make sure you are absolutely terrified of death, just to increase the pain.
|
| How to Stay Well (Or Get Better, If You’re Not So Well to Begin With)
· Do things that bring you a sense of fulfillment, joy, and purpose, that validate your worth. See your life as your own creation and strive to make it a positive one. · Pay close and loving attention to yourself, tuning in to your needs on all levels. Take care of yourself, nourishing, supporting, and encouraging yourself. · Release all negative emotions—resentment, envy, fear, sadness, anger. Express your feelings appropriately; don’t hold onto them. Forgive yourself. · Hold positive images and goals in your mind, pictures of what you truly want in your life. When fearful images arise, refocus on images that evoke feelings of peace and joy. · Love yourself, and love everyone else. Make loving the purpose and primary expression of your life. · Create fun, loving, honest relationships, allowing for the expression and fulfillment of needs for intimacy and security. Try to heal any wounds in past relationships, as with old lovers, and with your mother and father. · Make a positive contribution to your community, through some form of work or service that you value and enjoy. · Make a commitment to health and well-being, and develop a belief in the possibility of wholeness. Develop your own healing program, drawing on the support and advice of experts without becoming enslaved to them. · Accept yourself and everything in your life as an opportunity for growth and learning. Be grateful. When you fuck up, forgive yourself, learn what you can from the experience, and then move on. · Keep a sense of humor. |
As you go into the New Year, remind yourself that life has choices.
Toning quiets the mind and increases HRV more quickly than mindfulness practice
Posted: September 21, 2019 Filed under: behavior, Breathing/respiration, emotions, health, mindfulness, Pain/discomfort, relaxation, self-healing, stress management, Uncategorized | Tags: heart rate variability, intrusive thoughts, meditation, rumination 6 CommentsDisruptive thoughts, ruminations and worrying are common experiences especially when stressed. Numerous clinical strategies such as cognitive behavioral therapy attempt to teach clients to reduce negative ruminations (Kopelman-Rubin, Omer, & Dar, 2017). Over the last ten years, many people and therapists practice meditative techniques to let go and not be captured by negative ruminations, thoughts, and emotions. However, many people continue to struggle with distracting and wandering thoughts.
Just think back when you’re upset, hurt, angry or frustrated. Attempting just to observe without judgment can be very, very challenging as the mind keeps rehearsing and focusing on what happened. Telling yourself to stop being upset often doesn’t work because your mind is focused on how upset you are. If you can focus on something else or perform physical activity, the thoughts and feelings often subside.
Over the last fifteen years, mindfulness meditation has been integrated and adapted for use in behavioral medicine and psychology (Peper, Harvey, & Lin, 2019). It has also been implemented during bio- and neurofeedback training (Khazan, 2013; Khazan, 2019). Part of the mindfulness instruction is to recognize the thoughts without judging or becoming experientially “fused” with them. A process referred to as “meta-awareness” (Dahl, Lutz, & Davidson, 2015). Mindfulness training combined with bio- and neurofeedback training can improve a wide range of psychological and physical health conditions associated with symptoms of stress, such as anxiety, depression, chronic pain, and addiction (Creswell, 2015, Khazan, 2019).
Mindfulness is an effective technique; however, it may not be more effective than other self-regulations strategies (Peper et al, 2019). Letting go of worrying thoughts and rumination is even more challenging when one is upset, angry, or captured by stressful life circumstances. Is it possible that other strategies beside mindfulness may more rapidly reduce wandering and intrusive thoughts? In 2015, researchers van der Zwan, de Vente, Huiznik, Bogels, & de Bruin found that physical activity, mindfulness meditation and heart rate variability biofeedback were equally effective in reducing stress and its related symptoms when practiced for five weeks.
Our research explored whether other techniques from the ancient wisdom traditions could provide participants tools to reduce rumination and worry. We investigated the physiological effects and subject experiences of mindfulness and toning. Toning is vocalizing long and sustained sounds as a form of mediation. (Watch the video the toning demonstration by sound healer and musician, Madhu Anziani at the end of the blog.)
COMPARING TONING AND MINDFULNESS
The participants were 91 undergraduate college students (35 males, 51 females and 5 unspecified; average age, 22.4 years, (SD = 3.5 years).
After sitting comfortably in class, each student practiced either mindfulness or toning for three minutes each. After each practice, the students rated the extent of mind wandering, occurrence of intrusive thoughts and sensations of vibration on a scale from 0 (not all) to 10 (all the time). They also rated pre and post changes in peacefulness, relaxation, stress, warmth, anxiety and depression. After completing the assessment, they practice the other practice and after three minutes repeated the assessment.
The physiological changes that may occur during mindfulness practice and toning practice was recorded in a separate study with 11 undergraduate students (4 males, 7 females; average age 21.4 years. Heart rate and respiration were monitored with ProComp Infiniti™ system (Thought Technology, Ltd., Montreal, Canada). Respiration was monitored from the abdomen and upper thorax with strain gauges and heartrate was monitored with a blood volume pulse sensor placed on the thumb.
After the sensors were attached, the participants faced away from the screen so they did not receive feedback. They then followed the same procedure as described earlier, with three minutes of mindfulness, or toning practice, counterbalanced. After each condition, they completed a subjective assessment form rating experiences as described above.
RESULTS: SUBJECTIVE FINDINGS
Toning was much more successful in reducing mind wandering and intrusive thoughts than mindfulness. Toning also significantly increased awareness of body vibration as compared to mindfulness as shown in Figure 1.
Figure 1. Differences between mindfulness and toning practice.
There was no significant difference between toning and mindfulness in the increased self-report of peacefulness, warmth, relaxation, and decreased self-report of anxiety and depression as shown in Figure 2.
Figure 2. No significant difference between toning and mindfulness practice in relaxation or stress reports.
RESULTS: PHYSIOLOGICAL FINDINGS
Respiration rate was significantly lower during toning (4.6 br/min) as compared to mindfulness practice (11.6 br/min); heart rate standard deviation (SDNN) was much higher during toning condition (11.6) (SDNN 103.7 ms) than mindfulness (6.4) (SDNN 61.9 ms). Two representative physiological recording are shown in Figure 3.

Figure 3. Representative recordings of breathing and heart rate during mindfulness and toning practice. During toning the respiration rate (chest and abdomen) was much slower than during mindfulness and baseline conditions. Also, during toning heart rate variability was much larger than during mindfulness or baseline conditions.
DISCUSSION
Toning practice is a useful strategy to reduce mind wandering as well as inhibit intrusive thoughts and increase heart rate variability (HRV). Most likely toning uses the same neurological pathways as self-talk and thus inhibits the negative and hopeless thoughts. Toning is a useful meditation alternative because it instructs people to make a sound that vibrates in their body and thus they attend to the sound and not to their thoughts.
Physiologically, toning immediately changed the respiration rate to less than 6 breaths per minute and increases heart rate variability. This increase in heart rate variability occurs without awareness or striving. We recommend that toning is integrated as a strategy to complement bio-neurofeedback protocols. It may be a useful approach to enhance biofeedback-assisted HRV training since toning increases HRV without trying and it may be used as an alternative to mindfulness, or used in tandem for maximum effectiveness.
TAKE HOME MESSAGE
1) When people report feeling worried and anxious and have difficulty interrupting ruminations that they first practice toning before beginning mindfulness meditation or bio-neurofeedback training.
2) When training participants to increase heart rate variability, toning could be a powerful technique to increase HRV without striving
TONING DEMONSTRATION AND INSTRUCTION BY SOUND HEALER MADHU ANZIANI
For the published article see: Peper, E., Pollack, W., Harvey, R., Yoshino, A., Daubenmier, J. & Anziani, M. (2019). Which quiets the mind more quickly and increases HRV: Toning or mindfulness? NeuroRegulation, 6(3), 128-133.
REFERENCES
Creswell, J. D. (2015). Mindfulness Interventions. Annual Review of Psychology, 68, 491-516.
van der Zwan, J. E., de Vente, W., Huizink, A. C., Bogels, S. M., & de Bruin, E. I. (2015). Physical activity, mindfulness meditation, or heart rate variability biofeedback for stress reduction: A randomized controlled trial. Applied Psychophysiology and Biofeedback, 40(4), 257-268. https://doi.org/10.1007/s10484-015-9293-x
