Hope for abdominal discomfort
Posted: June 21, 2022 Filed under: behavior, biofeedback, Breathing/respiration, emotions, Evolutionary perspective, healing, health, Pain/discomfort | Tags: functional abdominal pain, heart rate variability, HRV, IBS, irritable bowel syndrome, neurasthenia, Rap, recurrent abdominal pain, respiration 3 CommentsAdapted from: Peper, E. & Harvey, R. (2022). Nausea and GI discomfort: A biofeedback assessment model to create a rational for training. Biofeedback, 50(1), 24–32. https://doi.org/10.5298/1081-5937-50.1.05
Abdominal discomfort and pain such as functional abdominal pain, acid reflux or irritable bowel affects many people. Teaching slower biofeedback-assisted HRV breathing with biofeedback is a useful strategy by which the person may be able to reduce symptoms. This essay provides detailed instruction for a first session assessment for clients who have abdominal discomfort (functional abdominal pain). Descriptions include how the physiological recording can be used to understand a possible etiology of the illness, to create a biological/evolutionary based explanation that is readily understood by the client, and finally to offer self-regulation suggestions to improve health.
Background of abdominal discomfort (irritable bowel syndrome, acid reflux, functional abdominal pain, recurrent abdominal pain)
Irritable bowel syndrome (IBS) affects 7% to 21% of the general population in Western cultures with a global prevalence estimated at around 11% (Fairbrass, Costantino, Gracie, & Ford, 2020). The chronic symptoms (i.e., lasting more than 30 days) usually include abdominal cramping, discomfort or pain, bloating, loose or frequent stools and constipation, which can significantly reduce the quality of life (Chey et al., 2015). A precursor of IBS in children is called recurrent abdominal pain (RAP), which affects 0.3% to 19% of school children (Chitkara et al., 2005). Both IBS and RAP appear to be functional illnesses, as no organic causes have been identified to explain the symptoms. IBS and RAP are contrasted to various types of diseases such as Crohn’s disease, inflammatory bowel disease or ulcerative colitis.
Multiple factors may contribute to IBS, such as genetics, food allergies, previous treatment with antibiotics, infections, psychological status and stress. More recently, dietary factors contributing to changes in the intestinal and colonic microbiome resulting in small intestine bacterial overgrowth have been suggested as another risk factor (Dupont, 2014). Generally, standard medical treatments (reassurance, dietary manipulation and of pharmacological therapy) are often ineffective in reducing IBS symptoms (Chey et al., 2015). On the other hand, complementary and alternative approaches such as biofeedback-assisted relaxation techniques (Davidoff & Whitehead, 1996; Goldenberg et al., 2019; Stern et al. 2014), autogenic training (Luthe & Schultz, 1969) and cognitive therapy are more effective than traditional medical treatment (Vlieger et al., 2008).
Biofeedback-assisted relaxation training typically moderates IBS or RAP symptoms by restoring balance in the nervous system (sympathetic/parasympathetic autonomic balance), such as through heart rate variability (HRV) breathing training. For example, Sowder et al. (2010) as well as Sun et al. (2016) demonstrated that functional abdominal pain can be reduced with HRV feedback training. In most cases, increased vagal tone was achieved by breathing at about six breaths per minute. While Taneja et al. (2004) reported that yogic breathing decreased diarrhea-predominant irritable bowel syndrome symptoms significantly more than conventional treatment in a randomized control study.Sympathetic/parasympathetic balance can be enhanced by increasing HRV, which occurs when a person breathes at their resonant frequency, which is usually 5–7 breaths per minute. For most people, the HRV training means breathing at much slower rate. A benefit of slow abdominal breathing appears to be a self-control strategy that can reduce symptoms of IBS, RAP and similar functional abdominal pain symptoms.
Mastery of effortless diaphragmatic breathing can be affected by injury, surgery or similar insults to the abdominal area (Peper et al., 2015). In addition, dysregulation of diaphragm, which is enervated by the phrenic nerve and the vagus nerve, along with dysregulation of other abdominal muscles appears to be associated with irritable bowel syndrome (Bordoni & Morabito, 2018). It is likely that slower biofeedback-assisted HRV breathing training restores abdominal muscles and diaphragmatic movement, theoretically by tonic and phasic regulation of the phrenic and vagal nerve activity (cf. Marchenko et al., 2015; Streeter et al., 2012). The theory, simply stated, is that HRV breathing training at an individual’s resonant frequency produces increases in regulatory neurotransmitters, particularly gamma amino butyric acid (GABA). Many of our students who complain of abdominal discomfort report reductions of symptoms following HRV breathing training.
Consistently for more than 40 years, we have taught undergraduate students a semester-long integrated stress management program that includes modified progressive relaxation, slow diaphragmatic breathing and changing internal language as outlined in the book, Make Health Happen, by Peper, Gibney & Holt (2002). At the end of each semester, numerous students report that their anxiety, gastrointestinal distress and other symptoms related to self-described IBS or RAP have decreased or disappeared (Peper et al., 2014; Peper, Miceli, & Harvey, 2016; Peper, Mason, Huey, 2017; Peper et al., 2020). Abdominal discomfort is prevalent experience of distress by college students. In our recent survey of 99 undergraduate students, 41% self-reported abdominal discomfort (25% irritable bowel or acid reflux), 86% self-reported anxiety, 70% neck and shoulder tension and 48% headaches. After practicing slower breathing (i.e., typically directing them to breath abdominally at a rate of about six breaths a minute) and focus on slower exhalation and allowing the air to flow in without effort as the abdominal wall expands, as a homework assignment for a week, many reported that their symptoms significantly decreased (Peper, Harvey, Cuellar, & Membrila, in press).
Case example illustrating how to use the physiological recording to guide the client discussion and provide motivation
A 16-year-old high school junior suffered from abdomen discomfort for years. The symptoms mainly consisted of frequent constipation, and when it occurred, great discomfort from nausea. After having been diagnosed and undergoing all the necessary tests by the gastroenterologist, there was no identifiable cause of the chief complaints. Biofeedback was suggested as an alternative to medications for symptom reduction. During the biofeedback assessment and training session, the client discussed what she would like to learn from the session. It was challenging for her to respond to those questions. Not being able to report what the client would like from a training session is also a very common experience when working with students. A useful strategy is to describe experiences of other students that the clients could relate to, and imply that their abdominal discomfort is somewhat commonplace in other students.
Discussed during the session was the link between being very sensitive and reactive to other people’s feeling and being concerned about what others think of her. The client nodded her head in agreement. When describing herself, she discussed being very perfectionistic using a scale from being lackadaisical/undemanding to being perfectionistic (i.e., self-oriented perfectionism, self-worth contingencies, concern over mistakes, doubts about actions, self-criticism, socially prescribed perfectionism, other-oriented perfectionism, hypercriticism; see Smith, Saklofske, Stoeber, & Sherry, 2016).
Furthermore, the client sat slouched in the chair. Possibly her slouched posture implied a state of powerlessness instead of empowerment, a state of being ready to react and protect (Carney, Cuddy, & Yap, 2010; Cuddy, 2012; Peper, Lin, & Harvey, 2017).
Working hypotheses. The client was very sensitive and continuously reacted to external and internal signals with sympathetic arousal, while masking her reactions. These ongoing flight/flight responses would decrease intestinal peristalsis and abdominal blood flow, which would result in nausea, constipation and abdominal distress. Namely, the body reacts to the stimuli as signals of danger and blood flow is shunted away from the abdomen into the large muscles to run and fight. To paraphrase Stanford University professor Robert Sapolsky (2004): Why should the body digest food and repair itself, if it is going to be the predator’s lunch? It is only when we are safe that we can digest and regenerate.
The session began by exploring how pressure on the abdomen could potentially affect experiences of nausea and abdominal distress. After explaining how the diaphragm descends and how abdominal content in the stomach can be displaced (spread out) during inhalation, we systematically changed her posture by placing and adjusting a small pillow behind her middle back so that she could sit tall. The tall posture resulted in an open feeling of empowerment not felt during slouching. She observed that breathing was slightly easier and felt there was more space in her abdomen. As she began to feel more comfortable during the training session, we discussed the impact of posture on the body. We also discussed the relationship between thoughts of perfectionism and abdominal discomfort. The discussion also included an exploration of why some people tend to curl-up and slouch in a protective posture (e.g., head down to protect the neck region and big bones of the arms and legs positioned to protect the core organs) when feeling self-consciousness or perfectionistic about body image.
Biofeedback monitoring for assessment
Psychophysiology was recorded with multichannel physiological system (Procomp Infinity System running Biograph Infinity software version 6.7.1, Thought Technology Ltd). Respiration was monitored with strain-gauge sensors placed around the abdomen and thoracic regions (for a discussion on sensor placement see Peper et al., 2016 and Chu et al., 2019). Blood volume pulse was recorded with the sensor placed on the left thumb. The thumb was used because the participant had small and cold fingers (for a discussion about blood volume pulse, see Peper et al, 2007 and Peper, Shafer, & Lin, 2010). Skin conductance was recorded with the sensor wrapped around the left index and middle fingers with the electrodes on the finger pads (for a discussion about skin conductance and normal values, see Khazan, 2019, and Shafer et al, 2016).
After sensors were attached and the signals explained, the client sat comfortably while looking at the screen. Unexpectedly the clinician clapped his hands and made a loud noise. The client reacted with a momentary startle and smile. The physiological response, showed an increase in skin conductance, decrease in pulse amplitude, decrease in abdominal diameter, and increase in heart rate, is shown in Figure 1.
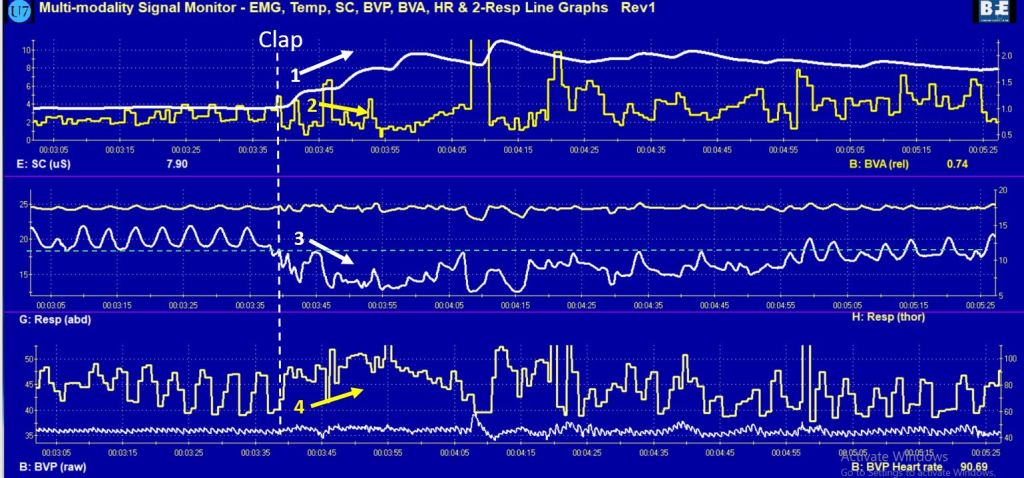
Figure 1. Physiological response to a loud noise (clap) (1) increased skin conductance, (2) decrease in pulse amplitude, (3) decrease in decreased abdominal circumference, and (4) increased heart rate and decreased heart rate variability.
The client was aware that she reacted to the clap; however, she was totally unaware how much her body responded. The computer screen display of her physiological reaction made the invisible visible. It provided the opportunity to discuss how various body reactions related to heart rate, breathing, and skin conductance could contribute to experiences of abdominal discomfort.
She was unaware that skin conductance did not return to baseline levels for more than 20 minutes. An elevated skin conductance level may mean that the body’s reaction to the hand-clap noise triggered a defense reaction and maintained the increased sympathetic activity for more than 20 minutes. Having a sustained flight/fight reaction to external stimuli such as a hand-clap would most likely affect digestive and peristalsis processes, contributing to symptoms found in IBS and RAP. The observations made during biofeedback monitoring led to a discussion of how sympathetic activation affects the gastrointestinal track.
Blood volume pulse amplitude decreased, which indicated a decrease in blood flow through her hands, which would decrease hand temperature and again indicated a systemic sympathetic activation.
Abdominal circumference decreased, which indicated that she tightened her abdominal muscles as a protective response to the hand-clap. She was unaware of the abdominal muscles tightening; however, she stated that she was aware that her breathing had changed. The abdominal muscle, which pulled the abdomen in, took almost two minutes to relax. The sustained muscle constriction around the abdomen increased pressure around the core organs, which may contribute to ongoing abdominal discomfort. A fight-flight reaction includes body bracing (e.g. tightened muscles, head down to protect the neck, big bones of arms and legs curled to protect core organs), and she confirmed that she experienced neck and shoulder tensions.
The discussion of abdominal muscle tension led to another discussion of how holding your stomach in may relate to self-image. For example, tight clothing can contribute to constricted movement around the abdomen. Wearing corsets contributed to psychophysiological symptoms, mainly for women in the late 19th and early 20th centuries, during a time when women who wore very tight corsets were diagnosed with neurasthenia. Simply stated, neurasthenia was characterized as a condition of mental and/or physical fatigue with at least two of the following symptoms: dyspepsia, dizziness, muscular aches or pains, tension headaches, inability to relax, irritability and sleep disturbance.
“Dyspepsia” was the commonly reported symptom of neurasthenia, which included upset stomach, a gnawing or burning stomach pain, heartburn, bloating, and or burping, nausea, and vomiting. The constricted waist region that resulted from wearing a corset in the name of fashion compromises the functions of both digestion and breathing. When the person inhales, the abdomen cannot expand as the diaphragm is flattening and pushing downward. Thus, the person is forced to breathe more shallowly by lifting their ribs; this increases neck and shoulder tension as well as the risk of anxiety, heart palpitation, and fatigue (Cohen & White, 1947; Courtney, 2009).
It also can contribute to abdominal discomfort since the abdomen is being squeezed by the corset and forcing the abdominal organs upward. Even architects of the Victorian era recognized a need for a place to position a chair or chaise lounge, such as at the top of some stairs, because people wearing corsets could faint, pass out or otherwise experience breathlessness through the effort of climbing the stairs with restrictive clothing around their abdomen (Melissa, 2015). Many of these symptoms could be easily reduced by wearing looser clothing and learning slower diaphragmatic breathing. In modern times, a related phenomenon results when people wear items of clothing that are too tight around their waist or abdomen (e.g., tight jeans) in service to fashion trends often labeled as designer jean syndrome (MacHose & Peper, 1991; Stonehewer, 2009). Similarly, when people wear garments that are too tight around their chest or thoracic region (e.g., tight vests) in service to external protection (e.g., athletes, industrial workers, police or soldiers wearing heavy, restrictive gear), then restrictive ventilatory disorders can occur (Harty et al., 1999). Simply stated, when the muscles related to breathing are restricted from moving, respiration is affected.
The client’s heart rate increased and stayed high for more than 30 seconds. The first decrease in heart rate at about 20 seconds after the hand-clap was a long sigh of relief as breathing (i.e., oxygen/carbon dioxide exchange) started again. It took almost 90 seconds before breathing and heart rate returned to normal as reflected by measures of HRV. The computer screen showing increased heart rate was reviewed with the client to explain how her body reacted with a fight-flight response to the hand-clap, as well as how regulating breathing through biofeedback training could lower the heart rate and reduce the sympathetic activation and enhance the parasympathetic activation.
Body responds to cognitive stressful thoughts
After discussion about the psychophysiological response to the hand-clap (a physical external stressor) and how other external stressors (e.g., startling noise) or internal stressors (e.g., perfectionistic ruminations) could trigger a similar response of abdominal muscle tightening, the assessment was repeated by having her relax and then think about a mental stressor, as shown in Figure 2.

Figure 2. Physiological responses to thinking about a past stressor (1) increased skin conductance, (2) decreased pulse amplitude, (3) decreased abdominal circumference, and (4) increased heart rate and decreased HRV.
The physiological response pattern to thinking about a past stressor was similar to the bodily reaction to a loud noise. The skin conductance increased and blood volume pulse amplitude decreased immediately after hearing (e.g., anticipating) the task of evoking/thinking of a past stressor. Most likely, the initial response was triggered by performance anxiety, then 6 seconds later the heart rate increased and breathing changed as she began experiencing the somatic reaction evoked by the recall of a negative stressor. The recordings also showed that her pulse amplitude decreased. The decrease in pulse amplitude suggested that her hands would probably become colder, which was confirmed by her self-report that she often experienced cold hands and feet. She reported being aware of the feeling an emotional reaction, but mainly noticing the change of breathing in her chest, and she was unaware of the abdominal changes. The client was surprised by how her body reacted to emotional thoughts. The recording viewed on the computer screen demonstrated objectively that her thoughts (initial performance anxiety) had a physical effect on her body. Specifically, experiencing the emotions that were evoked by recalling the stressful memory had a direct effect on the body in the same way that a physical external threat leads to a fight-flight response.
Building a psychophysiological model
Using these recorded computer images reflecting physical reactions to the hand clap and emotional thoughts, the discussion focused on how abdominal discomfort could be the result of activating a normal biological survival response. Survival responses would occur hundreds of times throughout a day, especially when worrying. Each thought would evoke the response, and the awareness of body reaction would evoke another reaction. Similar to how awareness of blushing amplifies blushing.
The client shared that she was very sensitive and reactive especially when other people were upset. She reported feeling “cursed” by their sensitivity and reactivity. The linguistic metaphor that could be used to describe her reactions is “she could not stomach what was going on.”
The discussion about physiological reactions provided the client with a model how her disorder (IBS and RAP) could have developed and been maintained over the years. The model matched her subjective experience: when stressed, the discomfort often increased. The discussion shifted to reframing her internal labels. Instead of describing her sensitivity as a curse, the sensitivity was reframed and labeled a gift; namely, she could sense many people’s emotional reactions, to which they would react in a variety of ways. She just needed to learn how to manage this sensitivity. Once she learned to manage it, she would have many advantages in interpersonal relations at home and at work. She would be able to sense what other people are experiencing. By reframing her symptoms as a result of a survival physiological response pattern, it reduces self- blame and offers solutions about how to master and change reactions and thereby have more control in the world.
Training to demonstrate control is possible.
The discussion was followed by teaching her diaphragmatic breathing in sitting and lying down positions. As she had no history of abdominal injuries, similar to many of our students, she rapidly demonstrated slower diaphragmatic breathing as shown in Figures 3 and 4.

Figure 3. The client practiced a few slower diaphragmatic breaths in the sitting and reclining position, which increased heart rate variability, decreased skin conductance and increased blood volume pulse amplitude.

Figure 4. Practicing slower diaphragmatic breathing at about six breaths per minute in a reclining position increased HRV.
With tactile coaching, she demonstrated that she could breathe at about six breaths per minute with the heart rate increasing during inhalation and decreasing during exhalation. She reported feeling more relaxed and that the sensations of nausea had disappeared. Additionally, her hands felt warmer. This recording provided proof that there was hope and that she could do something about her body’s psychophysiological responses.
The discussion focused on how breathing affecting heart rate variability. Namely, if she allowed exhalation to occur without effort, her heart rate decreased (the vagal response of slowing the heart) and thereby increased the parasympathetic activation that would support digestion and gastrointestinal functioning. Often when people practice effortless diaphragmatic breathing, abdominal noises (borborygmus)– the gurgling, rumbling, or squeaking noise from the abdomen–occur and indicate that intestinal activity is being activated, and that food, liquids and digestive juice are moving through the intestines. It is usually a positive indicator that the person is relaxing and sympathetic activity has been reduced.
During the last part of session, we reviewed how posture affects physiology, emotions and cognitions, as well as how posture and breathing would be the first step in beginning to reduce symptoms and enhance health. To provide additional information using video and bibliotherapy/education, we suggested that she watches the embedded videos in the blogs listed at the end of the article.
Recommendations for future sessions and home practice
The recommended strategies for future sessions would focus on teaching the client to master slow diaphragmatic breathing and practicing that for 10–20 minutes per day. The teaching techniques would incorporate imagery to imagine air flowing down their arms and legs as she exhaled. . More importantly, the focus would shift to generalize the skill during the day; namely, whenever she would become aware of feeling stressed or observed herself holding her breath or breathing in her chest, she would use that as the cue to shift to slower abdominal breathing. Had the client continued training, future sessions would focus on mastering slower diaphragmatic breathing. The training would include relaxing the lower abdominal muscles during inhalation, increasing control of HRV, practicing imagining stress and use image to trigger slower breathing, and cognitive reframing practices to interrupt worrying and promote self-acceptance. The final goal is to generalize these skills into daily life as illustrated in the successful cases described in the following blogs
Blogs on posture:
References
Bordoni, B. & Morabito, B. (2018). Symptomatology correlations between the diaphragm and irritable bowel syndrome. Cureus, 10(7), e3036. https://doi.org/10.7759/cureus.3036
Carney, D. R., Cuddy, A. J., & Yap, A. J. (2010). Power posing: brief nonverbal displays affect neuroendocrine levels and risk tolerance. Psychological Science, 10, 1363-1368. https://dx.doi.org/10.1177/0956797610383437
Chey, W. D., Kurlander, J., & Eswaran, S. (2015). Irritable bowel syndrome: a clinical review. Jama, 313(9), 949–958. https://doi.org/10.1001/jama.2015.0954
Chitkara, D. K., Rawat, D. J., & Talley, N. J. (2005). The epidemiology of childhood recurrent abdominal pain in Western countries: a systematic review. American journal of Gastroenterology, 100(8), 1868–1875. https://doi.org/10.1111/j.1572-0241.2005.41893.x
Chu, M., Nguyen, T., Pandey, V., Zhou, Y., Pham, H. N., Bar-Yoseph, R., Radom-Aizik, S., Jain, R., Cooper, D. M., & Khine, M. (2019). Respiration rate and volume measurements using wearable strain sensors. NPJ digital medicine, 2(1), 1–9. https://doi.org/10.1038/s41746-019-0083-3
Cohen, M. E. & White, P. D. (1947). Studies of breathing, pulmonary ventilation and subjective awareness of shortness of breath (dyspnea) in neurocirculatory asthenia, effort syndrome, anxiety neurosis. Journal of Clinical Investigation, 26(3), 520–529. https://doi.org/10.1172/JCI101836
Courtney, R. (2009). The functions of breathing and its dysfunctions and their relationship to breathing therapy. International Journal of Osteopathic Medicine, 12, 78–85. https://doi.org/10.1016/j.ijosm.2009.04.002
Cuddy, A. (2012). Your body language shapes who you are. Technology, Entertainment, and Design (TED) Talk, available at: http://www.ted.com/talks/amy_cuddy_your_body_language_shapes_who_you_are
Davidoff, A. L., & Whitehead, W. E. (1996). Biofeedback, relaxation training, and cognitive behavior modification: Treatments for functional GI disorders, In Olden, K, W. (ed). Handbook of Functional Gastrointestinal Disorders. CRC Press, 361–384.
Dupont, H. L. (2014). Review article: evidence for the role of gut microbiota in irritable bowel syndrome and its potential influence on therapeutic targets. Alimentary Pharmacology & Therapeutics, 39(10), 1033–1042. https://doi.org/10.1111/apt.12728
Fairbrass, K. M., Costantino, S. J., Gracie, D. J., & Ford, A. C. (2020). Prevalence of irritable bowel syndrome-type symptoms in patients with inflammatory bowel disease in remission: a systematic review and meta-analysis. The Lancet Gastroenterology & Hepatology, 5(12), 1053–162. https://doi.org/10.1016/s2468-1253(20)30300-9
Goldenberg, J. Z., Brignall, M., Hamilton, M., Beardsley, J., Batson, R. D., Hawrelak, J., Lichtenstein, B., & Johnston, B. C. (2019). Biofeedback for treatment of irritable bowel syndrome. Cochrane Database of Systematic Reviews, (11). https://doi.org/10.1002/14651858.CD012530.pub2
Harty, H. R., Corfield, D. R., Schwartzstein, R. M., & Adams, L. (1999). External thoracic restriction, respiratory sensation, and ventilation during exercise in men. Journal of Applied Physiology, 86(4), 1142–1150. https://doi.org/10.1152/jappl.1999.86.4.1142
Khazan, I. (2019). A guide to normal values for biofeedback. Biofeedback, 47(1), 2–5. https://doi.org/10.5298/1081-5937-47.1.03
Luthe, W. & Schultz, J. H. (1969). Autogenic Therapy Volume II: Medical Applications. Grune & Stratton.
MacHose, M., & Peper, E. (1991). The effect of clothing on inhalation volume. Biofeedback and Self-Regulation, 16(3), 261–265. https://doi.org/10.1007/BF01000020
Marchenko, V., Ghali, M. G., & Rogers, R. F. (2015). The role of spinal GABAergic circuits in the control of phrenic nerve motor output. American Journal of Physiology-Regulatory, Integrative and Comparative Physiology, 308(11), R916–R926. https://doi.org/10.1152/ajpregu.00244.2014
Melissa. (2015). Why women fainted so much in the 19th century. May 20, 2015. Downloaded October 2, 2021. http://www.todayifoundout.com/index.php/2015/05/women-fainted-much-19th-century/
Peper, E., Gibney, K. H., & Holt, C. F. (2002). Make Health Happen—Training Yourself to Create Wellness. Kendall/Hunt Publishing Company.
Peper, E., Gilbert, C. D., Harvey, R. & Lin, I-M. (2015). Did you ask about abdominal surgery or injury? A learned disuse risk factor for breathing dysfunction. Biofeedback. 34(4), 173–179. https://doi.org/10.5298/1081-5937-43.4.06
Peper, E., Groshans, G. H., Johnston, J., Harvey, R., & Shaffer, F. (2016). Calibrating respiratory strain gauges: What the numbers mean for monitoring respiration. Biofeedback, 44(2), 101–105. https://doi.org/10.5298/1081-5937-44.2.06
Peper, E., Harvey, R., Cuellar, Y., & Membrila, C.(in press). Reduce anxiety. NeuroRegulation.
Peper, E., Harvey, R., Lin, I. M., Tylova, H., & Moss, D. (2007). Is there more to blood volume pulse than heart rate variability, respiratory sinus arrhythmia, and cardiorespiratory synchrony? Biofeedback, 35(2), 54–61. https://www.researchgate.net/publication/259560204_Is_There_More_to_Blood_Volume_Pulse_Than_Heart_Rate_Variability_Respiratory_Sinus_Arrhythmia_and_Cardiorespiratory_Synchrony
Peper, E., Lin, I-M, & Harvey, R. (2017). Posture and mood: Implications and applications to therapy. Biofeedback, 35(2), 42–48. https://doi.org/10.5298/1081-5937-45.2.03
Peper, E., Lin, I-M, Harvey, R., Gilbert, M., Gubbala, P., Ratkovich, A., & Fletcher, F. (2014). Transforming chained behaviors: Case studies of overcoming smoking, eczema and hair pulling (trichotillomania). Biofeedback, 42(4), 154–160. https://doi.org/10.5298/1081-5937-42.4.06
Peper, E., Mason, L., Harvey, R., Wolski, L, & Torres, J. (2020). Can acid reflux be reduced by breathing? Townsend Letters-The Examiner of Alternative Medicine, 445/446, 44–47. https://www.townsendletter.com/article/445-6-acid-reflux-reduced-by-breathing/
Peper, E., Mason, L., Huey, C. (2017). Healing irritable bowel syndrome with diaphragmatic breathing. Biofeedback, 45(4), 83–87. https://doi.org/10.5298/1081-5937-45.4.04
Peper, E., Miceli, B., & Harvey, R. (2016). Educational model for self-healing: Eliminating a chronic migraine with electromyography, autogenic training, posture, and mindfulness. Biofeedback, 44(3), 130–137. https://www.aapb.org/files/publications/biofeedback/2016/biof-44-03-130-137.pdf
Peper, E., Shaffer, F., & Lin, I. M. (2010). Garbage in; Garbage out—Identify blood volume pulse (BVP) artifacts before analyzing and interpreting BVP, blood volume pulse amplitude, and heart rate/respiratory sinus arrhythmia data. Biofeedback, 38(1), 19–23. https://doi.org/10.5298/1081-5937-38.1.19
Sapolsky, R. (2004). Why Zebras Don’t Get Ulcers. Owl Books ISBN: 978-0805073690
Shaffer, F., Combatalade, D., Peper, E., & Meehan, Z. M. (2016). A guide to cleaner electrodermal activity measurements. Biofeedback, 44( 2), 90–100. https://doi.org/10.5298/1081-5937-44.2.01
Smith, M. M., Saklofske, D. H., Stoeber, J., & Sherry, S. B. (2016). The big three perfectionism scale: A new measure of perfectionism. Journal of Psychoeducational Assessment, 34(7), 670–687. https://doi.org/10.1177/0734282916651539
Sowder, E., Gevirtz, R., Shapiro, W., & Ebert, C. (2010). Restoration of vagal tone: a possible mechanism for functional abdominal pain. Applied Psychophysiology and Biofeedback, 35(3), 199–206. https://doi.org/10.1007/s10484-010-9128-8
Stern, M. J., Guiles, R. A., & Gevirtz, R. (2014). HRV biofeedback for pediatric irritable bowel syndrome and functional abdominal pain: A clinical replication series. Applied Psychophysiology and Biofeedback, 39(3), 287–291. https://doi.org/10.1007/s10484-014-9261-x
Stonehewer, L. (2009). Dysfunctional breathing for women’s health physiotherapists. Journal of the Association of Chartered Physiotherapists in Women’s Health, 104, 38–40. https://pogp.csp.org.uk/system/files/stonehewer_hr.pdf
Streeter, C. C., Gerbarg, P. L., Saper, R. B., Ciraulo, D. A., & Brown, R. P. (2012). Effects of yoga on the autonomic nervous system, gamma-aminobutyric-acid, and allostasis in epilepsy, depression, and post-traumatic stress disorder. Medical hypotheses, 78(5), 571–579. https://doi.org/10.1016/j.mehy.2012.01.021
Sun, X., Shang, W., Wang, Z., Liu, X., Fang, X., & Ke, M. (2016). Short-term and long-term effect of diaphragm biofeedback training in gastroesophageal reflux disease: An open-label, pilot, randomized trial. Diseases of the Esophagus, 29(7), 829–836. https://doi.org/10.1111/dote.12390
Taneja. I., Deepak, K.K., Poojary, G., Acharya, I.N., Pandey, R.M., & Sharma, M.P. (2004). Yogic versus conventional treatment in diarrhea-predominant irritable bowel syndrome: a randomized control study. Appl Psychophysiol Biofeedback, 29(1), 19-33. https://doi.org/10.1023/b:apbi.0000017861.60439.95
Vlieger, A. M., Blink, M., Tromp, E., & Benninga, M. A. (2008). Use of complementary and alternative medicine by pediatric patients with functional and organic gastrointestinal diseases: results from a multicenter survey. Pediatrics, 122(2), e446–e451. https://doi.org/10.1542/peds.2008-0266
Meditation Myths and Tips for Practice
Posted: May 19, 2022 Filed under: behavior, Breathing/respiration, cognitive behavior therapy, emotions, healing, health, meditation, mindfulness, self-healing | Tags: Mindfulness-based cognitive therapy, mindfulness-based stress reduction, TM, transcendental meditation Leave a commentMindfulness-based strategies are drawn from ancient Buddhist practices and have found acceptance as one of the major behavioral medicine techniques of today (Hilton et al, 2016; Khazan, 2013). Throughout this blog the term mindfulness will refer broadly to a mental state of paying total attention to the present moment, with a non-judgmental awareness of inner and outer experiences (Baer, Smith, & Allen, 2004; Kabat-Zinn, 1994). This approach is the common core for many stress management approaches (Peper, Harvey, & Lin, 2019).
Background
Transcendental meditation (TM), a form of concentrative meditation involving repetition of a sacred word or phrase known as a mantra, was a popular meditation technique introduced in the United States from India and participants reported improvement of mental and physical health (Wallace, 1970; Paul-Labrador et al, 2006; Rainforth et al, 2007; Hawkins, 2003). To make TM more acceptable for the western audience, Herbert Benson, MD, adapted and simplified the TM process and then labelled a core element, the ‘relaxation response’ (Benson, Beary, & Carol, 1974; Benson & Clipper, 1992). Instead of giving people a secret mantra and part of a spiritual tradition, he recommend using the word “one” as the mantra. Since that time numerous studies have demonstrated that when patients practice the relaxation response, many clinical symptoms were reduced.
In 1979, Jon Kabat-Zinn introduced a manual for a standardized Mindfulness-Based Stress Reduction (MBSR) program at the University of Massachusetts Medical Center (Kabat-Zinn, 1994; Kabat-Zin, 2003). The eight-week program combined mindfulness as a form of insight meditation with mindful yogic movement exercises designed to focus awareness on body sensations, thoughts, feelings, and behaviors. Mindfulness based programs have become a predominant approach used in behavioral medicine.
Mindfulness-based cognitive therapy (MBCT) and mindfulness-based stress reduction (MBSR) combine mindfulness meditation training with cognitive therapy and is a useful approach to reduce a variety of mental and physical conditions such as stress, anxiety, depression, addiction, disordered eating, chronic pain, sleep disturbances, and high blood pressure (Andersen et al., 2013; Carlson, Speca, Patel, & Goodey, 2003; Fjorback, Arendt, Ørnbøl, Fink, & Walach, 2011; Greeson, & Eisenlohr-Moul, 2014; Hoffman et al., 2012; Marchand, 2012; Baer, 2015; Demarzo et al, 2015; Khoury et al, 2013; Khoury et al, 2015; Teasdale, Segal, & Williams, 1995; Kabat-Zinn, 1994; Kabat-Zin, 2003; Zimmermann, Burrell, , & Jordan, 2018). Although in most cases, MBSR is helpful, in some cases meditation can evoke negative physical and/or psychological outcomes and inhibit prosocial behavior (Kreplin et al, 2018; Lindahl et al, 2017). Based on this encouraging research, many people are learning to meditate on their own using meditation apps. However, there are many questions that can arise for people new to meditation – such as what is meditation, how do I do it, what are the challenges, and how is it helpful? Some people also develop misconceptions about what meditation is and can become discouraged.
Watch the outstanding presentation by Professor Jennifer Daubenmier presented for the Holistic Health Lecture Series, in which she discusses meditation myths and pragmatic tips for practice.
References
Andersen, S. R., Würtzen, H., Steding-Jessen, M., Christensen, J., Andersen, K. K., Flyger, H., … & Dalton, S. O. (2013). Effect of mindfulness-based stress reduction on sleep quality: Results of a randomized trial among Danish breast cancer patients. Acta Oncologica, 52(2), 336-344. https://doi.org/10.3109/0284186X.2012.745948
Baer, R., Smith, G., & Allen, K. (2004). Assessment of mindfulness by self-report: The Kentucky Inventory of Mindfulness Skills. Assessment, 11, 191–206. https://doi.org/10.1177/1073191104268029
Benson, H., Beary, J. F., & Carol, M. P. (1974).The Relaxation Response. Psychiatry, 37(1), 37-46. https://www.tandfonline.com/loi/upsy20
Benson, H. & Clipper, M.Z. (1992). The Relaxation Response. Wings Books.
Carlson, L. E., Speca, M., Patel, K. D., & Goodey, E. (2003). Mindfulness‐based stress reduction in relation to quality of life, mood, symptoms of stress, and immune parameters in breast and prostate cancer outpatients. Psychosomatic Medicine, 65(4), 571-581. https://doi.org/10.1097/01.psy.0000074003.35911.41
Demarzo, M. M., Montero-Marin, J., Cuijpers, P., Zabaleta-del-Olmo, E., Mahtani, K. R., Vellinga, A., Vicens, C., López-del-Hoyo, Y., & García-Campayo, J. (2015). The Efficacy of Mindfulness-Based Interventions in Primary Care: A Meta-Analytic Review. Annals of family medicine, 13(6), 573–582. https://doi.org/10.1370/afm.1863
Fjorback, L. O., Arendt, M., Ørnbøl, E., Fink, P., & Walach, H. (2011). Mindfulness‐Based Stress Reduction and Mindfulness‐Based Cognitive Therapy–A systematic review of randomized controlled trials. Acta Psychiatrica Scandinavica, 124(2), 102-119. https://doi.org/10.1111/j.1600-0447.2011.01704.x
Greeson, J., & Eisenlohr-Moul, T. (2014). Mindfulness-based stress reduction for chronic pain. In R. A. Baer (Ed.), Mindfulness-Based Treatment Approaches: Clinician’s Guide to Evidence Base and Applications, 269-292. San Diego, CA: Academic Press. https://www.academia.edu/8092878/Mindfulness_Based_Stress_Reduction_for_Chronic_Pain
Hawkins, M. A. (2003). Effectiveness of the Transcendental Meditation program in criminal rehabilitation and substance abuse recovery, Journal of Offender Rehabilitation, 36(1-4), 47-65. https://doi.org/10.1300/J076v36n01_03
Hilton, L., Hempel, S., Ewing, B. A., Apaydin, E., Xenakis, L., Newberry, S., …Maglione, M. A. (2016). Mindfulness meditation for chronic pain: Systematic review and meta-analysis. Annals of Behavioral Medicine, 51(2), 199-213. https://doi.org/10.1007/s12160-016-9844-2
Hoffman, C. J., Ersser, S. J., Hopkinson, J. B., Nicholls, P. G., Harrington, J. E., & Thomas, P. W. (2012). Effectiveness of mindfulness-based stress reduction in mood, breast-and endocrine-related quality of life, and well-being in stage 0 to III breast cancer: A randomized, controlled trial. Journal of Clinical Oncology, 30(12), 1335-1342. https://doi.org/10.1200/JCO.2010.34.0331
Kabat-Zinn, J. (1994). Wherever you go, there you are: Mindfulness meditation in everyday life. New York: Hyperion.
Kabat-Zinn, J. (2003). Mindfulness-based stress reduction (MBSR). Constructivism in the Human Sciences, 8, 73–107. https://www.proquest.com/openview/fef538e3ed2210c1201ef2a946faed43/1?pq-origsite=gscholar&cbl=29080
Khazan, I. Z. (2013). The clinical handbook of biofeedback: A step-by-step guide for training and practice with mindfulness. John Wiley & Sons.
Khoury, B., Lecomte, T., Fortin, G., Masse, M., Therien, P., Bouchard, V., Chapleau, M., Paquin, K., & Hofmann, S. G. (2013). Mindfulness-based therapy: A comprehensive meta-analysis. Clinical Psychology Review, 33(6), 763-771. https://doi.org/10.1016/j.cpr.2013.05.005
Khoury, B., Sharma, M., Rush, S. E., & Fournier, C. (2015). Mindfulness-based stress reduction for healthy individuals: A meta-analysis. Journal of Psychosomatic Research, 78(6), 519-528. https://doi.org/10.1016/j.jpsychores.2015.03.009
Kreplin, U., Farias, M., & Brazil, I. A. (2018). The limited prosocial effects of meditation: A systematic review and meta-analysis. Sci Rep, 8, 2403. https://doi.org/10.1038/s41598-018-20299-z
Lindahl, J. R., Fisher, N. E., Cooper, D. J., Rosen, R. K, & Britton, W. B. (2017) The varieties of contemplative experience: A mixed-methods study of meditation-related challenges in Western Buddhists. PLoSONE, 12(5): e0176239. https://doi.org/10.1371/journal.pone.0176239
Marchand, W. R. (2012). Mindfulness-based stress reduction, mindfulness-based cognitive therapy, and Zen meditation for depression, anxiety, pain, and psychological distress. Journal of Psychiatric Practice, 18(4), 233-252. https://doi.org/10.1097/01.pra.0000416014.53215.86
Paul-Labrador, M., Polk, D., Dwyer, J.H. et al. (2006). Effects of a randomized controlled trial of Transcendental Meditation on components of the metabolic syndrome in subjects with coronary heart disease. Archive of Internal Medicine, 166(11), 1218-1224. https://doi.org/10.1001/archinte.166.11.1218
Peper, E., Harvey, R., & Lin, I-M. (2019). Mindfulness training has themes common to other technique. Biofeedback. 47(3), 50-57. https://doi.org/10.5298/1081-5937-47.3.02
Rainforth, M.V., Schneider, R.H., Nidich, S.I., Gaylord-King, C., Salerno, J.W., & Anderson, J.W. (2007). Stress reduction programs in patients with elevated blood pressure: A systematic review and meta-analysis. Current Hypertension Reports, 9(6), 520–528. https://doi.org/10.1007/s11906-007-0094-3
Teasdale, J. D., Segal, Z., & Williams, J. M. (1995). How does cognitive therapy prevent depressive relapse and why should attentional control (mindfulness) training help? Behaviour Research and Therapy, 33, 25–39. https://doi.org/10.1016/0005-7967(94)e0011-7
Wallace, K.W. (1970). Physiological Effects of Transcendental Meditation. Science, 167 (3926), 1751-1754. https://doi.org/10.1126/science.167.3926.1
A breath of fresh air: Breathing and posture to optimize health
Posted: April 3, 2022 Filed under: behavior, Breathing/respiration, CBT, cognitive behavior therapy, emotions, ergonomics, Exercise/movement, health, mindfulness, Neck and shoulder discomfort, Pain/discomfort, posture, self-healing, stress management, Uncategorized | Tags: respiration 2 CommentsMost people breathe 22,000 breaths per day. We tend to breathe more rapidly when stressed, anxious or in pain. While a slower diaphragmatic breathing supports recovery and regeneration. We usually become aware of our dysfunctional breathing when there are problems such as nasal congestion, allergies, asthma, emphysema, or breathlessness during exertion. Optimal breathing is much more than the absence of symptoms and is influenced by posture. Dysfunctional posture and breathing are cofactors in illness. We often do not realize that posture and breathing affect our thoughts and emotions and that our thoughts and emotions affect our posture and breathing. Watch the video, A breath of fresh air: Breathing and posture to optimize health, that was recorded for the 2022 Virtual Ergonomics Summit.
Reduce anxiety
Posted: March 23, 2022 Filed under: behavior, Breathing/respiration, CBT, cognitive behavior therapy, digital devices, education, emotions, health, mindfulness, posture, relaxation, self-healing, stress management | Tags: anxiety, concentration, insomnia, menstrual cramps, pain 3 Comments
The purpose of this blog is to describe how a university class that incorporated structured self-experience practices reduced self-reported anxiety symptoms (Peper, Harvey, Cuellar, & Membrila, 2022). This approach is different from a clinical treatment approach as it focused on empowerment and mastery learning (Peper, Miceli, & Harvey, 2016).
As a result of my practice, I felt my anxiety and my menstrual cramps decrease. — College senior
When I changed back to slower diaphragmatic breathin, I was more aware of my negative emotions and I was able to reduce the stress and anxiety I was feeling with the deep diaphragmatic breathing.– College junior
Background
More than half of college students now report anxiety (Coakley et al., 2021). In our recent survey during the first day of the spring semester class, 59% of the students reported feeling tired, dreading their day, being distracted, lacking mental clarity and had difficulty concentrating.
Before the COVID pandemic nearly one-third of students had or developed moderate or severe anxiety or depression while being at college (Adams et al., 2021. The pandemic accelerated a trend of increasing anxiety that was already occurring. “The prevalence of major depressive disorder among graduate and professional students is two times higher in 2020 compared to 2019 and the prevalence of generalized anxiety disorder is 1.5 times higher than in 2019” As reported by Chirikov et al (2020) from the UC Berkeley SERU Consortium Reports.
This increase in anxiety has both short and long term performance and health consequences. Severe anxiety reduces cognitive functioning and is a risk factor for early dementia (Bierman et al., 2005; Richmond-Rakerd et al, 2022). It also increases the risk for asthma, arthritis, back/neck problems, chronic headache, diabetes, heart disease, hypertension, pain, obesity and ulcer (Bhattacharya et al., 2014; Kang et al, 2017).
The most commonly used treatment for anxiety are pharmaceutical and cognitive behavior therapy (CBT) (Kaczkurkin & Foa, 2015). The anti-anxiety drugs are usually benzodiazepines (e.g., alprazolam (Xanax), clonazepam (Klonopin), chlordiazepoxide (Librium), diazepam (Valium) and lorazepam (Ativan). Although these drugs they may reduce anxiety, they have numerous side effects such as drowsiness, irritability, dizziness, memory and attention problems, and physical dependence (Shri, 2012; Crane, 2013).
Cognitive behavior therapy techniques based upon the assumption that anxiety is primarily a disorder in thinking which then causes the symptoms and behaviors associated with anxiety. Thus, the primary treatment intervention focuses on changing thoughts.
Given the significant increase in anxiety and the potential long term negative health risks, there is need to provide educational strategies to empower students to prevent and reduce their anxiety. A holistic approach is one that assumes that body and mind are one and that soma/body, emotions and thoughts interchangeably affect the development of anxiety. Initially in our research, Peper, Lin, Harvey & Perez (2017) reported that it was easier to access hopeless, helpless, powerless and defeated memories in a slouched position than an upright position and it was easier to access empowering positive memories in an upright position than a slouched position. Our research on transforming hopeless, helpless, depressive thought to empowering thoughts, Peper, Harvey & Hamiel (2019) found that it was much more effective if the person first shifts to an upright posture, then begins slow diaphragmatic breathing and finally reframes their negative to empowering/positive thoughts. Participants were able to reframe stressful memories much more easily when in an upright posture compared to a slouched posture and reported a significant reduction in negative thoughts, anxiety (they also reported a significant decrease in negative thoughts, anxiety and tension as compared to those attempting to just change their thoughts).
The strategies to reduce anxiety focus on breathing and posture change. At the same time there are many other factors that may contribute the onset or maintenance of anxiety such as social isolation, economic insecurity, etc. In addition, low glucose levels can increase irritability and may lower the threshold of experiencing anxiety or impulsive behavior (Barr, Peper, & Swatzyna, 2019; Brad et al, 2014). This is often labeled as being “hangry” (MacCormack & Lindquist, 2019). Thus, by changing a high glycemic diet to a low glycemic diet may reduce the somatic discomfort (which can be interpreted as anxiety) triggered by low glucose levels. In addition, people are also sitting more and more in front of screens. In this position, they tend to breathe quicker and more shallowly in their chest.
Shallow rapid breathing tends to reduce pCO2 and contributes to subclinical hyperventilation which could be experienced as anxiety (Lum, 1981; Wilhelm et al., 2001; Du Pasquier et al, 2020). Experimentally, the feeling of anxiety can rapidly be evoked by instructing a person to sequentially exhale about 70 % of the inhaled air continuously for 30 seconds. After 30 seconds, most participants reported a significant increase in anxiety (Peper & MacHose, 1993). Thus, the combination of sitting, shallow breathing and increased stress from the pandemic are all cofactors that may contribute to the self-reported increase in anxiety.
To reduce anxiety and discomfort, McGrady and Moss (2013) suggested that self-regulation and stress management approaches be offered as the initial treatment/teaching strategy in health care instead of medication. One of the useful approaches to reduce sympathetic arousal and optimize health is breathing awareness and retraining (Gilbert, 2003).
Stress management as part of a university holistic health class
Every semester since 1976, up to 180 undergraduates have enrolled in a three-unit Holistic Health class on stress management and self-healing (Klein & Peper, 2013). Students in the class are assigned self-healing projects using techniques that focus on awareness of stress, dynamic regeneration, stress reduction imagery for healing, and other behavioral change techniques adapted from the book, Make Health Happen (Peper, Gibney & Holt, 2002).
82% of students self-reported that they were ‘mostly successful’ in achieving their self-healing goals. Students have consistently reported achieving positive benefits such as increasing physical fitness, changing diets, reducing depression, anxiety, and pain, eliminating eczema, and even reducing substance abuse (Peper et al., 2003; Bier et al., 2005; Peper et al., 2014).
This assessment reports how students’ anxiety decreased after five weeks of daily practice. The students filled out an anonymous survey in which they rated the change in their discomfort after practicing effortless diaphragmatic breathing. More than 70% of the students reported a decrease in anxiety. In addition, they reported decreases in symptoms of stress, neck and shoulder pain as shown in Figure 1.

Figure 1. Self-report of decrease in symptoms after practice diaphragmatic breathing for a week.
In comparing the self-reported responses of the students in the holistic health class to those of the control group (N=12), the students in the holistic health class reported a significant decrease in symptoms since the beginning of the semester as compared to the control group as shown in Figure 2.

Figure 2. Change in self-reported symptoms after 6 weeks of practice the integrated holistic health skills as compared to the control group who did not practice these skills.
Changes in symptoms Most students also reported an increase in mental clarity and concentration that improved their study habits. As one student noted: Now that I breathe properly, I have less mental fog and feel less overwhelmed and more relaxed. My shoulders don’t feel tense, and my muscles are not as achy at the end of the day.
The teaching components for the first five weeks included a focus on the psychobiology of stress, the role of posture, and psychophysiology of respiration. The class included didactic presentations and daily self-practice
Lecture content
- Diadactic presentation on the physiology of stress and how posture impacts health.
- Self-observation of stress reactions; energy drain/energy gain and learning dynamic relaxation.
- Short experiential practices so that the student can experience how slouched posture allows easier access to helpless, hopeless, powerless and defeated memories.
- Short experiential breathing practices to show how breathing holding occurs and how 70% exhalation within 30 seconds increases anxiety.
- Didactic presentation on the physiology of breathing and how a constricted waist tends to have the person breathe high in their chest (the cause of neurasthemia) and how the fight/flight response triggers chest breathing, breath holding and/or shallow breathing.
- Explanation and practice of diaphragmatic breathing.
Daily self-practice
Students were assigned weekly daily self-practices which included both skill mastery by practicing for 20 minutes as well and implementing the skill during their daily life. They then recorded their experiences after the practice. At the end of the week, they reviewed their own log of week and summarized their observations (benefits, difficulties) and then met in small groups to discuss their experiences and extract common themes. These daily practices consisted of:
- Awareness of stress. Monitoring how they reacted to daily stressor
- Practicing dynamic relaxation. Students practiced for 20 minutes a modified progressive relaxation exercise and observed and inhibit bracing pattern
- Changing energy drain and energy gains. Students observed what events reduced or increased their subjective energy and implemented changes in their behavior to decrease events that reduced their energy and increased behaviors that increase their enery
- Creating a memory of wholeness practice
- Practicing effortless breathing. Students practiced slowly diaphragmatic abdominal breathing for 20 minutes per day and each time they become aware of dysfunctional breathing (breath holding, shallow chest breathing, gasping) during the day, they would shift to slower diaphragmatic breathing.
Discussion
Almost all students were surprised how beneficial these practices were to reduce their anxiety and symptoms. Generally, the more the students would interrupt their personal stress responses during the day by shifting to diaphragmatic breathing the more did they experience success. We hypothesize that some of the following factors contributed to the students’ improvement.
- Learning through self-mastery as an education approach versus clinical treatment.
- Generalizing the skills into daily life and activities. Practicing the skills during the day in which the cue of a stress reaction triggered the person to breathe slowly. The breathing would reduce the sympathetic activation.
- Interrupting escalating sympathetic arousal. Responding with an intervention reduced the sense of being overwhelmed and unable to cope by the participant by taking charge and performing an active task.
- Redirecting attention and thoughts away from the anxiety triggers to a positive task.
- Increasing heart rate variability. Through slow breathing heart rate variability increased which enhanced sympathetic parasympathetic balance.
- Reducing subclinical hyperventilation by breathing slower and thereby increasing pC02.
- Increasing social support by meeting in small groups. The class discussion group normalized the anxiety experiences.
- Providing hope. The class lectures, assigned readings and videos provide hope; since, it included reports how other students had reversed their chronic disorders such as irritable bowel disease, acid reflux, psoriasis with behavioral interventions.
Although the study lacked a control group and is only based upon self-report, it offers an economical non-pharmaceutical approach to reduce anxiety. These stress management strategies may not resolve anxiety for everyone. Nevertheless, we recommend that schools implement this approach as the first education intervention to improve health in which students are taught about stress management, learn and practice relaxation and diaphragmatic breathing and then practice these skills during the day whenever they experience stress or dysfunctional breathing.
I noticed that breathing helped tremendously with my anxiety. I was able to feel okay without having that dreadful feeling stay in my chest and I felt it escape in my exhales. I also felt that I was able to breathe deeper and relax better altogether. It was therapeutic, I felt more present, aware, and energized.
See the following blogs for detailed breathing instructions
References
Adams. K.L., Saunders KE, Keown-Stoneman CDG, et al. (2021). Mental health trajectories in undergraduate students over the first year of university: a longitudinal cohort study. BMJ Open 2021; 11:e047393. https://doi.org/10.1136/bmjopen-2020-047393
Barr, E. A., Peper, E. & Swatzyna, R.J. (2019). Slouched Posture, Sleep Deprivation, and Mood Disorders: Interconnection and Modulation by Theta Brain Waves. Neuroregulation, 6(4), 181–189 https://doi.org/10.15540/nr.6.41.181
Bhattacharya, R., Shen, C. & Sambamoorthi, U. (2014). Excess risk of chronic physical conditions associated with depression and anxiety. BMC Psychiatry 14, 10 (2014). https://doi.org/10.1186/1471-244X-14-10
Bier, M., Peper, E., & Burke, A. (2005). Integrated stress management with ‘Make Health Happen: Measuring the impact through a 5-month follow-up. Poster presentation at the 36th Annual Meeting of the Association for Applied Psychophysiology and Biofeedback. Abstract published in: Applied Psychophysiology and Biofeedback, 30(4), 400. https://biofeedbackhealth.files.wordpress.com/2013/12/2005-aapb-make-health-happen-bier-peper-burke-gibney3-12-05-rev.pdf
Bierman, E.J.M., Comijs, H.C. , Jonker, C. & Beekman, A.T.F. (2005). Effects of Anxiety Versus Depression on Cognition in Later Life. The American Journal of Geriatric Psychiatry,13(8), 686-693, https://doi.org/10.1097/00019442-200508000-00007.
Brad, J., Bushman, C., DeWall, N., Pond, R.S., &. Hanus, M.D. (2014).. Low glucose relates to greater aggression in married couples. PNAS, April 14, 2014. https://doi.org/10.1073/pnas.1400619111
Chirikov, I., Soria, K. M, Horgos, B., & Jones-White, D. (2020). Undergraduate and Graduate Students’ Mental Health During the COVID-19 Pandemic. UC Berkeley: Center for Studies in Higher Education. Retrieved from https://escholarship.org/uc/item/80k5d5hw
Coakley, K.E., Le, H., Silva, S.R. et al. Anxiety is associated with appetitive traits in university students during the COVID-19 pandemic. Nutr J 20, 45 (2021). https://doi.org/10.1186/s12937-021-00701-9
Crane,E.H. (2013).Highlights of the 2011 Drug Abuse Warning Network (DAWN) Findings on Drug-Related Emergency Department Visits. 2013 Feb 22. In: The CBHSQ Report. Rockville (MD): Substance Abuse and Mental Health Services Administration (US); 2013-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK384680/
Du Pasquier, D., Fellrath, J.M., & Sauty, A. (2020). Hyperventilation syndrome and dysfunctional breathing: update. Revue Medicale Suisse, 16(698), 1243-1249. https://europepmc.org/article/med/32558453
Gilbert C. Clinical Applications of Breathing Regulation: Beyond Anxiety Management. Behavior Modification. 2003;27(5):692-709. https://doi.org/10.1177/0145445503256322
Kaczkurkin, A.N. & Foa, E.B. (2015). Cognitive-behavioral therapy for anxiety disorders: an update on the empirical evidence. Dialogues Clin Neurosci. 17(3):337-46. https://doi.org/10.31887/DCNS.2015.17.3/akaczkurkin
Kang, H. J., Bae, K. Y., Kim, S. W., Shin, H. Y., Shin, I. S., Yoon, J. S., & Kim, J. M. (2017). Impact of Anxiety and Depression on Physical Health Condition and Disability in an Elderly Korean Population. Psychiatry investigation, 14(3), 240–248. https://doi.org/10.4306/pi.2017.14.3.240
Klein, A. & Peper, W. (2013). There is Hope: Autogenic Biofeedback Training for the Treatment of Psoriasis. Biofeedback, 41(4), 194–201. https://doi.org/10.5298/1081-5937-41.4.01
Lum, L. C. (1981). Hyperventilation and anxiety state. Journal of the Royal Society of Medicine, 74(1), 1-4. https://journals.sagepub.com/doi/pdf/10.1177/014107688107400101
MacCormack, J. K., & Lindquist, K. A. (2019). Feeling hangry? When hunger is conceptualized as emotion. Emotion, 19(2), 301–319. https://doi.org/10.1037/emo0000422
McGrady, A. & Moss, D. (2013). Pathways to illness, pathways to health. New York: Springer. https://link.springer.com/book/10.1007/978-1-4419-1379-1
Peper, E., Gibney, K.H., & Holt, C.F. (2002). Make health happen: Training yourself to create wellness. Dubuque, IA: Kendall/Hunt Publishing Company. https://he.kendallhunt.com/make-health-happen
Peper, E., Harvey, R., Cuellar, Y., & Membrila, C. (2022). Reduce anxiety. NeuroRegulation, 9(2), 91–97. https://doi.org/10.15540/nr.9.2.91 https://www.neuroregulation.org/article/view/22815/14575
Peper, E., Harvey, R., & Hamiel, D. (2019). Transforming thoughts with postural awareness to increase therapeutic and teaching efficacy. NeuroRegulation, 6(3),153-169. doi:10.15540/nr.6.3.1533-1 https://www.neuroregulation.org/article/view/19455/13261
Peper, E., Lin, I-M., Harvey, R., & Perez, J. (2017). How posture affects memory recall and mood. Biofeedback.45 (2), 36-41. https://doi.org/10.5298/1081-5937-45.2.01
Peper, E., Lin, I-M, Harvey, R., Gilbert, M., Gubbala, P., Ratkovich, A., & Fletcher, F. (2014). Transforming chained behaviors: Case studies of overcoming smoking, eczema and hair pulling (trichotillomania). Biofeedback, 42(4), 154-160. https://doi.org/10.5298/1081-5937-42.4.06
Peper, E., MacHose, M. (1993). Symptom prescription: Inducing anxiety by 70% exhalation. Biofeedback and Self-Regulation 18, 133–139). https://doi.org/10.1007/BF00999790
Peper, E., Miceli, B., & Harvey, R. (2016). Educational Model for Self-healing: Eliminating a Chronic Migraine with Electromyography, Autogenic Training, Posture, and Mindfulness. Biofeedback, 44(3), 130–137. https://doi.org/10.5298/1081-5937-44.3.03
Peper, E., Sato-Perry, K & Gibney, K. H. (2003). Achieving Health: A 14-Session Structured Stress Management Program—Eczema as a Case Illustration. 34rd Annual Meeting of the Association for Applied Psychophysiology and Biofeedback. Abstract in: Applied Psychophysiology and Biofeedback, 28(4), 308. Proceeding in: http://www.aapb.org/membersonly/articles/P39peper.pdf
Richmond-Rakerd, L.S., D’Souza, S, Milne, B.J, Caspi, A., & Moffitt, T.E. (2022). Longitudinal Associations of Mental Disorders with Dementia: 30-Year Analysis of 1.7 Million New Zealand Citizens. JAMA Psychiatry. Published online February 16, 2022. https://doi.org/10.1001/jamapsychiatry.2021.4377
Shri, R. (2012). Anxiety: Causes and Management. The Journal of Behavioral Science, 5(1), 100–118. Retrieved from https://so06.tci-thaijo.org/index.php/IJBS/article/view/2205
Wilhelm, F.H., Gevirtz, R., & Roth, W.T. (2001). Respiratory dysregulation in anxiety, functional cardiac, and pain disorders. Assessment, phenomenology, and treatment. Behav Modif, 25(4), 513-45. https://doi.org/10.1177/0145445501254003
Resolving a chronic headache with posture feedback and breathing
Posted: January 4, 2022 Filed under: behavior, Breathing/respiration, computer, digital devices, ergonomics, health, laptops, Neck and shoulder discomfort, Pain/discomfort, posture, relaxation, self-healing, stress management, Uncategorized | Tags: Desktop feedback app, headache, migraine 37 Comments| Adapted from Peper, E., Covell, A., & Matzembacker, N. (2021). How a chronic headache condition became resolved with one session of breathing and posture coaching. NeuroRegulation, 8(4), 194–197. https://doi.org/10.15540/nr.8.4.194 |

This blog describes the process by which a 32 year old woman student’s chronic headaches that she had since age eighteen was resolved in a single coaching session. The student suffered two or three headache per week a week which initially began when she was eighteen after using digital devices and encouraged her to slouch as she looked down. Although she describes herself as healthy, she reported having high level of anxiety and occasional depression. She self-medicated with 2 to 10 Excedrin tablets a week. It is possible that the chronic headaches could partially be triggered by caffeine withdrawal which get resolved by taking more Excedrins (Greben et al., 1980) since Excedrin contains 65 mg of caffeine as well as 250 mg of Acetaminophen which can be harmful to liver function (Bauer et al., 2021).
The behavioral coaching intervention
During the first day in class, the student approached the instructor and she shared that she had a severe headache. During their conversation, the instructor noticed that she was breathing in her chest without abdominal movement, her shoulders were held tight, her posture slightly slouched and her hands were cold. As she was unaware of her body responses, the instructor offered to guide her through some practices that may be useful to reduce her headache. The same strategies could also be useful for the other students in the class; since, headaches, anxiety, zoom fatigue, neck and shoulder tension, abdominal discomfort, and vision problems are common and have increased as people spent more time in front of screens (Charles et al., 2021; Ahmed et al., 2021; Bauer, 2021; Kuehn, 2021; Peper et al., 2021 ).
These symptoms may occur because of bad posture, neck and shoulder tension, shallow chest breathing, stress and social isolation (Elizagaray-Garcia et al., 2020; Schulman, 2002). When people become aware of their dysfunctional somatic patterns and change their posture, breathing pattern, internal language and implement stress management techniques, they often report a reduction in symptoms such as irritable bowel syndrome, acid reflux, neck and shoulder tension, or anxiety (Peper et al, 2017a; Peper et al, 2016a). Sometimes, a single coaching session can be sufficient to improve health.
Working hypothesis: The headaches were most likely tension headaches and not migraines and may be the result of chronic neck and shoulder tension which was maintained during chest breathing and the slouched head forward body posture. If she could change her posture, relax her neck and shoulders, and breathe diaphragmatically so that the lower abdomen widen during inhalation, most likely her shoulder and neck tension would decrease. Therefore, by changing posture from a slouched to upright position combined with slower diaphragmatic breathing, the muscle tension would be reduced and the headaches would decrease.
Breathing and posture changes
She was encouraged to sit upright so that the abdomen had space to expand (Peper et al., 2020). In addition, she needed to loosen the clothing around her waist to provide room for her abdomen to expand during inhalation instead of her chest lifting (MacHose & Peper, 1991). Allowing abdominal expansion can be challenging for many paticipants since they are self-conscious about their body image, as well holding their stomach in as an unconscious learned response to avoid pain after having had abdominal surgery, or as an automatic protective response to threat (Peper et al., 2015). The upright position also allowed her to sit tall and erect in which the back of head reaches upward towards the ceiling while relaxing and feeling gravity pulling her shoulders downward and at the same time relaxing her hips and legs.
With guided verbal and tactile coaching, she learned to master slower diaphragmatic breathing in which she gently and slowly exhaled by making a sound of pssssssst (exhaling through pursed lips) which tends to activate the transverse and oblique abdominal muscles and slightly tighten the pelvic floor muscles so that her lower abdomen would slightly constrict at the end of the exhalation (Peper et al., 2016). Then, by allowing the lower abdomen and pelvic floor relax so that the abdomen could expand in 360 degrees, inhalation occurred.
While practicing the slower breathing in this relaxed upright position, she was instructed to sense/imagine feeling a flow of down and through her arms and out her hands as she exhaled (as if the air could flow through straws down her arms). After a few minutes, she felt her headache decrease and noticed that her hands had warmed. After this short coaching intervention, she went back to her seat in class and continued to practice the relaxed effortless breathing while sitting upright and allowing her shoulders to melt downward.
The use of muscle feedback to demonstrate residual covert muscle tension
During class session, she volunteered to have her trapezius muscle monitored with electromyography (EMG). The EMG indicated that her muscles were slightly tense even though she reported feeling relaxed. With a few minutes of EMG biofeedback exploration, she discovered that she could relax her shoulder muscles by feeling them being heavy and melting.
Implementing home practice with a posture app
As part of the class homework, she was assigned a self-study for two weeks with the posture feedback app, Dario Desktop. The app uses the computer/laptop camera to monitor posture and provides visual feedback in a small window on the computer screen and/or an auditory signal each time she slouches as shown in Figure 1.

Figure 1. Posture feedback to signal to participant that the person is slouching.
To observe the effect of the posture breathing training, she monitored her symptoms for three days without feedback and then installed the posture feedback application on her laptop to provide feedback whenever she slouched. The posture feedback reminded her to practice better posture during the day while working on her computer and also do a few stretches or shift to standing when using the computer for an extended period of time. Each time the feedback signal indicated she slouched, she would sit up and change her posture, breathe lower and slower and relax her shoulders.
She also monitored what factors triggered the slouching. In additionally, she added daily reminders to her phone to remind her of her posture and to stretch and stand after each hour of studying. After two weeks she recorded her symptoms for three days for the post assessment without posture feedback.
Results
The chronic headache condition which had been present for fourteen years disappeared and she has not used any medication since the first day of class. She reported after two weeks that her shoulder and back discomfort/pain, depression, anxiety and lack of motivation decreased as shown in Figure 2. At the fourteen week follow up, she continues to have no headaches and has not used any medication.

Figure 2. Changes in symptoms after implementing posture feedback for two weeks.
She used the desktop posture app every time she opened her laptop at home as often as 3-5 times per day (roughly 2-6 hours).In addition, when she felt beginning of discomfort or thought she should take medication, she would adjust her posture and breathe. While using the app, she identified numerous factors that were associated with slouching as shown in Figure 3.

Figure 3. Behaviors associated with slouching.
Discussion
The decrease in depression, anxiety and increase in motivation may be the direct result of posture change; since, a slouched position tends to increase hopeless, helpless and powerless thoughts while the upright position tends to increase subjective felt energy and easier access to empowering and positive thoughts (Peper et al., 2017b; Veenstra et al., 2017; Wilson & Peper, 2004; Tsai et al., 2016). Most likely, a major factor that contributed to the elimination of her headaches was that she implemented changes in her behavior. One major factor was using posture feedback tool at home to remind her to sit tall and relax her shoulders while practicing slower diaphragmatic breathing. As she noted, “Although it was distracting to be reminded all the time about my posture, it did decrease my neck pain. With the pain reduction, I was able to sit at the computer longer and felt more motivated.”
The combination of slower lower abdominal breathing with the upright posture reversed her protective/defensive body position (tightening the muscle in the lower abdomen and pelvic floor and pressing the knees together while curling the shoulder forward for protection). The upright posture creates a position of empowerment and trust by which the lower abdomen could expand which supported health and regeneration. In addition, the upright posture allowed easier access to positive thoughts and reduced recall of hopeless, powerless, defeated memories. It is also possible that caffeine withdrawal was a co-factor in evoking headaches (Küçer, 2010). By eliminating the medication containing caffeine, she also eliminated the triggering of the caffeine withdrawal headaches.
This case example suggests that health care providers first rule out any pathology and then teach behavioral self-healing strategies that the clients can implement instead of immediately prescribing medications. These interventions could include slower and lower diaphragmatic breathing, upright posture feedback, muscle biofeedback training, hear rate variability training, stress management, cognitive behavior therapy and facilitating health promoting lifestyles modifications such as regular sleep, exercise and healthier diet. When students implement these behavioral changes as part of a five week self-healing program, many report significant decreases in symptoms such as headaches, anxiety, neck and shoulder pain, and gastrointestinal distress (Peper et al., 2016a).
Watch April Covell describe her experience with the self-healing approach to eliminate her chronic headaches.
See the following blogs for additional instructions how to breathe diaphragmatically.
References
Ahmed, S., Akter, R., Pokhrel, N. et al. (2021). Prevalence of text neck syndrome and SMS thumb among smartphone users in college-going students: a cross-sectional survey study. J Public Health (Berl.) 29, 411–416. https://doi.org/10.1007/s10389-019-01139-4
Bauer, A.Z., Swan, S.H., Kriebel, D. et al. (2021). Paracetamol use during pregnancy — a call for precautionary action. Nat Rev Endocrinol . https://doi.org/10.1038/s41574-021-00553-7
Charles, N. E., Strong, S. J., Burns, L. C., Bullerjahn, M. R., & Serafine, K. M. (2021). Increased mood disorder symptoms, perceived stress, and alcohol use among college students during the COVID-19 pandemic. Psychiatry research, 296, 113706. https://doi.org/10.1016/j.psychres.2021.113706
Elizagaray-Garcia, I., Beltran-Alacreu, H., Angulo-Díaz, S., Garrigós-Pedrón, M., Gil-Martínez, A. (2020). Chronic Primary Headache Subjects Have Greater Forward Head Posture than Asymptomatic and Episodic Primary Headache Sufferers: Systematic Review and Meta-analysis. Pain Med, 21(10):2465-2480. https://doi.org/10.1093/pm/pnaa235
Greden, J.F., Victor, B.S., Fontaine, P., & Lubetsky, M. (1980). Caffeine-Withdrawal Headache: A Clinical Profile. Psychosomatics, 21(5), 411-413, 417-418. https://doi.org/10.1016/S0033-3182(80)73670-8
Küçer, N. (2010). The relationship between daily caffeine consumption and withdrawal symptoms: a questionnaire-based study. Turk J Med Sci, 40(1), 105-108. https://doi.org/10.3906/sag-0809-26
Kuehn, B.M. (2021). Increase in Myopia Reported Among Children During COVID-19 Lockdown. JAMA, 326(11),999. https://doi.org/10.1001/jama.2021.14475
MacHose, M. & Peper, E. (1991). The effect of clothing on inhalation volume. Biofeedback and Self-Regulation 16, 261–265 (1991). https://doi.org/10.1007/BF01000020
Peper, E., Booiman, A., Lin, I-M, Harvey, R., & Mitose, J. (2016). Abdominal SEMG Feedback for Diaphragmatic Breathing: A Methodological Note. Biofeedback. 44(1), 42-49. https://doi.org/10.5298/1081-5937-44.1.03
Peper, E., Gilbert, C.D., Harvey, R. & Lin, I-M. (2015). Did you ask about abdominal surgery or injury? A learned disuse risk factor for breathing dysfunction. Biofeedback. 34(4), 173-179. https://doi.org/10.5298/1081-5937-43.4.06
Peper, E., Lin, I-M., Harvey, R., & Perez, J. (2017b). How posture affects memory recall and mood. Biofeedback. 45 (2), 36-41. https://doi.org/10.5298/1081-5937-45.2.01
Peper, E., Mason, L., Harvey, R., Wolski, L, & Torres, J. (2020). Can acid reflux be reduced by breathing? Townsend Letters-The Examiner of Alternative Medicine, 445/446, 44-47. https://www.townsendletter.com/article/445-6-acid-reflux-reduced-by-breathing/
Peper, E., Mason, L., Huey, C. (2017a). Healing irritable bowel syndrome with diaphragmatic breathing. Biofeedback. (45-4). https://doi.org/10.5298/1081-5937-45.4.04
Peper, E., Miceli, B., & Harvey, R. (2016a). Educational Model for Self-healing: Eliminating a Chronic Migraine with Electromyography, Autogenic Training, Posture, and Mindfulness. Biofeedback, 44(3), 130–137. https://doi.org/10.5298/1081-5937-44.3.03
Peper, E., Wilson, V., Martin, M., Rosegard, E., & Harvey, R. (2021). Avoid Zoom fatigue, be present and learn. NeuroRegulation, 8(1), 47–56. https://doi.org/10.15540/nr.8.1.47
Schulman, E.A. (2002). Breath-holding, head pressure, and hot water: an effective treatment for migraine headache. Headache, 42(10), 1048-50. https://doi.org/10.1046/j.1526-4610.2002.02237.x
Tsai, H. Y., Peper, E., & Lin, I. M.* (2016). EEG patterns under positive/negative body postures and emotion recall tasks. NeuroRegulation, 3(1), 23-27. https://doi.org/10.15540/nr.3.1.23
Veenstra, L., Schneider, I.K., & Koole, S.L. (2017). Embodied mood regulation: the impact of body posture on mood recovery, negative thoughts, and mood-congruent recall. Cogntion and Emotion, 31(7), 1361-1376. https://doi.org/10.1080/02699931.2016.1225003
Wilson, V.E. and Peper, E. (2004). The effects of upright and slumped postures on the generation of positive and negative thoughts. Applied Psychophysiology and Biofeedback, 29(3), 189–195. https://doi.org/10.1023/b:apbi.0000039057.32963.34
Healing from paralysis-Music (toning) to activate health
Posted: November 22, 2021 Filed under: behavior, Breathing/respiration, emotions, healing, health, mindfulness, stress management, Uncategorized | Tags: chakra, chanting, music therapy, paralysis, quadriplegia, singing, Toning 8 CommentsMadhu Anziani and Erik Peper

In April 2009, Madhu Anziani, just one month prior to graduation from San Francisco State University with a degree in Jazz/World music performance, fell two stories and broke C5 and C7 vertebras. He became a quadriplegic (tretraplegia) and could not breathe, talk, move his arms and legs and was incontinent. He also could not remember anything about the accident because of retrograde amnesia. Even though he was paralyzed and the medical staff suggested that he focussed on how to live well as a quadriplegic, he transcended his paralysis and the prognosis and is now a well-known vocal looping arts and ceremonial song leader/composer.
His recovery against all odds provides hope that growth and healing is possible when the mind and spirit focus on possibilities and not on limitations. Alongside physical thereapy he utilized energy healing and toning/sound vibrations to recover mobility. Toning, the vocalization of an elonggated monotonous vowel sound susteained for a number of minutes tends to vibrate specific areas in the body where the chakras are located (Crowe & Scovel, 1996; Goldman, 2017). Toning compared to mindfulness meditation reduces intrusive thoughts and mind wandering. It also increases body vibration sensations and heart rate variability much more than mindfulness practice (Peper et al, 2019). The body vibrations induced by toning and music could be one of the mechanisms by which recovery can occur at an accelerated rate as it allows the person’s passive awareness and sustained attention to feel the paralyzed body and yet be relaxed in the present without judgement.
Watch Madhu’s inspirational presentation as part of the Holistic Health Lecture Series by the Institute for Holistic Health Studies, San Francisco State University. In this presentation, he describes the process of recovery and guides the viewer through toning practices to evoke quieting of mind, bliss within the heart, and a healing state of being.
For an additional discussion and guided practice in toning, see the blog, Toning quiets the mind and increases HRV more quickly than mindfulness practice.
Madu Anziani is a sound healer who endured being a tetraplegic (paralysis affecting all four
limbs) and used sound and energy healing to recover mobility. He is a SFSU graduate and most
well-known as a vocal looping artist and ceremonial song leader/composer.
http://www.firstwasthesound.com
http://madhu.bandcamp.co
REFERENCES:
Goldman, J. (2017). The 7 Secrets of Sound Healing. Carlsbad, CA: Hay House Inc.
Reduce the spread of COVID and influenza by improving building ventilation
Posted: September 14, 2021 Filed under: behavior, Breathing/respiration, COVID, health | Tags: air circulation, airborne pathogens, Cholera, influenza, John Snow, ventilation 1 CommentAdapted from the superb article by Sarah Zhang, The plan to stop every respiratory virus at once. The Atlantic. (September 7, 2021).
With good clean air circulation, the risk of transmitting or contracting airborne disease such as COVID-19 during air travel is very low (Pombal, Hosegood & Powell, 2020). Pombal, Hosegood & Powell, 2020 point out that modern airplanes maintain clean air by circulating a mix of fresh air and air recycled through HEPA filter. Air enters from overhead air inlets and flows downward toward floor level outlets at the same seat row or nearby rows. There is little airflow forward and backward between rows.
The risk of transmission or contracting airborne dieases is very high if the airplane ventilation system is not working while passengers are in the plane. For example, when a jet airliner with 54 persons aboard was delayed on the ground for three hours with an inoperative ventilation system 72 % of the passengers became ill with symptoms of cough, fever, fatigue, headache, sore throat and myalgia within 72 hours (Moser et al.,1979).
To reduce the risk of COVID and other airborne infections such as influenza, government policies need to implement strategies to reduce exposure to airborne pathogens and optimize the immune system. By improving ventilation that reduces and removes airborne pathogens, thousands, if not millions, lives will be saved from being infected or dying of COVID or influenza.
Before the COVID pandemic between 2010 and 2020 an average of 39,900 people a year died of influenza in the United States and during a severe influenza season such as that occurred in 2017-2018, 61,000 people died (CDC, 2021). Influenza, just as COVID, is caused by an airborne pathogens (viruses). Although wearing masks significantly reduces the airborne spread of the pathogens, the long term preventative solution is to implement indoor ventilation strategies so that the air is not contaminated in the same way that we expect drinking water not to cause illness. From a public health perspective, changing external environment so the virus is cannot spread is a more effective strategy than depending upon individuals’ actions to prevent the spread of the pathogens.
By improving the air filtration and fresh air circulation in rooms and buildings, COVID, influenza virus and other airborne pathogens can be significantly reduced just as that has been done in modern airplanes. This demands changes in building ventilation codes and design. It means changing the physical infrastructure and upgrading ventilation systems so that only fresh and/or filtered air circulates through the rooms. This infrastructure improvement would be analogous to what occurred in the 19th century in eventually eliminating the cholera epidemics that killed thousands of people a year.
For example in England during the 1831-1832 and 1848 cholera epidemics more than 50,000 people died each year as they became infected with the toxigenic bacterium Vibrio cholerae which was present the water or foods contaminated with feces from a a person infected with cholera bacterium. Approximately 1 in 10 people who get sick with cholera will develop severe symptoms and without treatment, death can occur within hours (CDC, 2021).
In Londong during the 1854 cholera epidemic Dr. John Snow observed that people who got cholera were drawing water from a the same water pump on Broad Street. He persuaded the authorities to remove the pump handle which eliminated the use of the contaminated water and stopped the spread of the Cholera.

The water pump in Broadwick Street.
This public health intervention provided some of the rationale in 19th century to build the infrastructure to provide clean drinking water and appropriate sewage disposal, so that cholera, typhoid as well as other waterborne diseases epidemics would not enter the drinking water supply.
We now need a similar infrastructure improvement to provide clean air in buildings to stop the spread of COVID-19 variants and influenza. How ventilation affects the spread a virus in a class room is illustrated in the outstanding graphical modeling by Nick Bartzokas et al. (February 26, 2021) in the New York Times article, Why opening windows is a key to reopening schools. The spatial guidelines need to be based upon air flow and not on the distance of separation.
In summary, to prevent future airborne illnesses, local, state and federal government need to create and implement ventilation standards so that airborne pathogens are not spread indoors by contaminated air. This is not rocket science! It is a very solvable problem and has been implemented in airplanes. When the air is HEPA filtered so that passengers do not rebreathe each other’s potentially contaminated exhaled air, airborne transmission is very low. Let’s do the same for the air circulating in buildings.
For an indepth analyses, read the superb article, The Plan to Stop Every Respiratory Virus at Once, by Sarah Zhang published September 7, 2021 in the The Atlantic.
For more details to reduce virus exposure and increase immune competence, see the previoius published blogs,
https://peperperspective.com/2021/07/05/reduce-your-risk-of-covid-19-variants-and-future-pandemics/
REFERENCES
CDC (2021). Disease Burden of Influenza. Center for Disease Control and Prevention. https://www.cdc.gov/flu/about/burden/index.html
Moser, M.R., Bender, T.R., Margolis, H.S., Noble, G.R., Kendal, A.P., & Ritter, D.G. (1979). An outbreak of influenza aboard a commercial airliner. Am J Epidemiol, 110(1), 1-6. https://doi.org/10.1093/oxfordjournals.aje.a112781
Pombal, R., Hosegood, I., & Powell, D. (2020). Risk of COVID-19 During Air Travel. JAMA, 324(17), 1798 https://doi.org/10.1001/jama.2020.19108
Zhang, S. (September 7, 2021). The plan to stop every respiratory virus at once. The Atlantic. Downloaded September 13. https://www.theatlantic.com/health/archive/2021/09/coronavirus-pandemic-ventilation-rethinking-air/620000/
Useful resources about breathing, phytonutrients and exercise
Posted: June 30, 2021 Filed under: behavior, Breathing/respiration, cancer, Evolutionary perspective, health, Nutrition/diet, self-healing, Uncategorized | Tags: diet, exercise, immune system, nasal breathing, phytonutrients, respiration 1 Comment
Dysfunctional breathing, eating highly processed foods, and lack of movement contribute to development of illnesses such as cancer, diabetes, cardiovascular disease and many chronic diseases. They also contributes to immune dysregulation that increases vulnerability to infectious diseases, allergies and autoimmune diseases. If you wonder what breathing patterns optimize health, what foods have the appropriate phytonutrients to support your immune system, or what the evidence is that exercise reduces illness and promotes longevity, look at the following resources.
Breath: the mind-body connector that underlies health and illness
Read the outstanding article by Martin Petrus (2021). How to breathe.
https://psyche.co/guides/how-to-breathe-your-way-to-better-health-and-transcendence
You are the food you eat
Watch the superb webinar presentation by Deanna Minich, MS., PHD., FACN, CNS, (2021) Phytonutrient Support for a Healthy Immune System.
Movement is life
Explore the summaries of recent research that has demonstrated the importance of exercise to increase healthcare saving and reduce hospitalization and death.
Clean the air with plants*
Posted: March 22, 2021 Filed under: Breathing/respiration, ergonomics, health, Uncategorized | Tags: air pollution, plants Leave a comment
Fresh clean air is essential for health while polluted air is an environmental health hazard. For more than fifty years the harm of air pollution has been documented. As the National Institute of Environmental Health Sciences (NIH NIEHS) points out, initially air pollution was primarily regarded as threat to respiratory health and contributed to an increases in asthma, emphysema, chronic obstructive pulmonary disease, and chronic bronchitis. More recently, air pollution has been identified as a significant risk factor for cardiovascular disease, diabetes mellitus, obesity, reproductive, neurological, and immune system disorders and ADHD (Keller et al., 2018; Perera et al, 2014; NIH NIEHS ).
Yet many of us are unaware that often the air we breathe indoors is even more polluted than the outside air. The indoor air is the sum of outdoor air plus the indoor air pollution produced from cooking and outgassing of the volatile organic compounds (VOCs) from the many materials (Wolkoff, 2028). Materials and equipment in home and office also shed micro dust particles and outgas a chemical brew of volatile organic compounds (e.g., formaldehyde, benzene and tricholorethylene). These VOCs come from paper, inks, furniture, carpet, paints, wall coverings, cleaning materials, floor tiles and the fumes produced from gas heaters and cooking stoves. In addition, copiers and laser printers often add microscopic dust particles and sometimes ozone. These gasses stay in the room where there is limited air circulation due to sealed buildings or closed windows. Reduced air circulation is also a significant risk factor for COVID-19; since, the virus keeps recirculating in unventilated rooms. See the superb graphic illustration by Bartzokas et al (Feb 26, 2021).in the New York Times of virus concentration in schools when the windows are opened. https://www.nytimes.com/interactive/2021/02/26/science/reopen-schools-safety-ventilation.html?smid=em-share).
Be proactive to reduce pollution and enhance your health by placing plants in your office and home. When the plants are placed in the office, they also enhances subjective perceptions of air quality, concentration, and workplace satisfaction as well as objective measures of productivity (Nieuwenhuis et al., 2014). Certain plants help remove carbon dioxide and convert it to oxygen, clear the indoor smog, and remove the volatile organic compounds. Warning: Be sure that your pets do not chew or eat the leaves of these plants because they could be poisonous (e.g., azaleas are poisonous for dogs and cats),
The following plants help remove carbon dioxide and by converting it into oxygen.
- Areca Palm. You will need four shoulder height plants per person to convert all the exhaled carbon dioxide into oxygen (Meattle, 20009; Meattle, 2018).
- Mother-in-law’s Tongue is a bedroom plant because it converts carbon dioxide into oxygen at night. You will need six to eight shoulder height plants per person (Meattle, 20009).
Watch Kamal Meattle short TED talk presentation, How to grow fresh air (for an updated longer presentation watch, https://www.youtube.com/watch?v=KXgWxRUGLwM). https://www.ted.com/talks/kamal_meattle_how_to_grow_fresh_air?language=en#t-100683
The following plants remove VOCs from the air (Wolverton, 2020).
- Azaleas, rubber plants, tulips, poinsettia, philodendron, money plant, and bamboo palms (formaldehyde)
- Areca palm (toluene)
- Lady palm (ammonia)
- Peace lily and chrysanthemum (acetone, methanol, trichlorethylene, benzene, ethylacetate)
To remove particulates, install an air purifier with a HEPA filter.
After renovation or installation of furniture or carpets, be sure to allow for air circulation by opening windows and doors. Explore some of the following strategies to clean the air:
- Turn the exhaust fan on when cooking and using the oven.
- Ventilate your work area (open a window or door, if possible).
- Move copier/laser printers to a well-ventilated space and/or place an exhaust fan near the printer.
- Turn off copier or laser printers when not in use (purchase new equipment that is energy efficient and shuts down when not in use).
Take a many walks outside in nature
If possible take a walk at lunch or ask coworkers to have a walking meeting so that you can get out in the fresh air. Being in nature and forest bathing (Shinrin-Yoku) is associated with a decrease in stress, regeneration and improvement in immune function (Park et al., 2010; Hansen et a., 2017; Lyu et al., 2019). Watch the presentation by Dr. Aiko Yoshino, Soaking Up the Benefits of Nature During the PandemicForum.
* Adapted from Peper, E. (2023). Clean air with plants. Townsend Letters. The Examiner of Alternative Medicine, Sunday, June 4, 2023. https://www.townsendletter.com/e-letter-11-using-plants-to-improve-indoor-air-quality/
Republished: Peper, E. (2024). Townsend e-Letter, Townsend Letters. The Examiner of Alternative Medicine, June 3, 2024. https://www.townsendletter.com/e-letter-11-using-plants-to-improve-indoor-air-quality/
References:
Meattle, K. (2018). How to grow fresh air inside your house amidst pollution. Quint Fit. https://www.youtube.com/watch?v=KXgWxRUGLwM
Nieuwenhuis, M., Knight, C., Postmes, T., & Haslam, S. A. (2014). The relative benefits of green versus lean office space: Three field experiments. Journal of Experimental Psychology: Applied, 20(3), 199–214. https://doi.org/10.1037/xap0000024
NIH NIEHS, Air Pollution and Your Health, National Institute of Health, National Institute of Environmental Health Sciences https://www.niehs.nih.gov/health/topics/agents/air-pollution/index.cfm#:~:text=Air%20pollution%20can%20affect%20lung,are%20linked%20to%20chronic%20bronchitis
Resolve Eyestrain and Screen Fatigue
Posted: June 29, 2020 Filed under: Breathing/respiration, computer, digital devices, ergonomics, Exercise/movement, health, laptops, Neck and shoulder discomfort, Pain/discomfort, relaxation, stress management, Uncategorized, vision | Tags: blurry vision, computer vision syndrome, dry eyes, eyestrain, near vision stress, zoom fatigue 13 CommentsAdapted from: Peper, E., Harvey, R. & Faass, N. (2020). TechStress: How Technology is Hijacking Our Lives, Strategies for Coping, and Pragmatic Ergonomics. Berkeley: North Atlantic Books.

Forty percent of adults and eighty percent of teenagers report experiencing significant visual symptoms (eyestrain, blurry vision, dry eyes, headaches, and exhaustion) during and immediately after viewing electronic displays. These ‘technology-associated overuse’ symptoms are often labeled as digital eyestrain or computer vision syndrome (Rosenfield, 2016; Randolph & Cohn, 2017). Even our distant vision may be affected— after working in front of a screen for hours, the world looks blurry. At the same time, we may experience an increase in neck, shoulders and back discomfort. These symptoms increase as we spend more hours looking at computer screens, laptops, tablets, e-readers, gaming consoles, and cellphones for work, taking online classes, watching streaming videos for entertainment, and keeping connected with friends and family (Borhany et al, 2018; Turgut, 2018; Jensen et al, 2002).
Eye, head, neck, shoulder and back discomfort are partly the result of sitting too long in the same position and attending to the screen without taking short physical and vision breaks, moving our bodies and looking at far objects every 20 minutes or so. The obvious question is, “Why do we stare at and are captured by, the screen?” Two answers are typical: (1) we like the content of what is on the screen; and, (2) we feel compelled to watch the rapidly changing visual scenes.
From an evolutionary perspective, our sense of vision (and hearing) evolved to identify predators who were hunting us, or to search for prey so we could have a nice meal. Attending to fast moving visual changes is linked to our survival. We are unaware that our adaptive behaviors of attending to a visual or auditory signals activate the same physiological response patterns that were once successful for humans to survive–evading predictors, identifying food, and discriminating between friend or foe. The large and small screen (and speakers) with their attention grabbing content and notifications have become an evolutionary trap that may lead to a reduction in health and fitness (Peper, Harvey & Faass, 2020).
Near vision stress
To be able to see the screen, the eyes need to converge and accommodate. To converge, the extraocular muscles of the eyes tighten; to focus (accomodation), the ciliary muscle around the lens tighten to increase the curvature of the lens. This muscle tension is held constant as long as we look at the screen. Overuse of these muscles results is near vision stress that contributes to computer vision syndrome, development of myopia in younger people, and other technology-associated overuse syndromes (Sherwin et al, 2012; Enthoven et al, 2020).
Continually overworking the visual muscles related to convergences increases tension and contributes to eyestrain. While looking at the screen, the eye muscles seldom have the chance to relax. To function effectively, muscles need to relax /regenerate after momentary tightening. For the eye muscles to relax, they need to look at the far distance– preferably objects green in color. As stated earlier, the process of distant vision occurs by relaxing the extraocular muscles to allow the eyes to diverge along with relaxing the ciliary muscle to allow the lens to flatten. In our digital age, where screen of all sizes are ubiquitous, distant vision is often limited to the nearby walls behind a screen or desk which results in keeping the focus on nearby objects and maintaining muscular tension in the eyes.
As we evolved, we continuously alternated between between looking at the far distance and nearby areas for food sources as well as signals indicating danger. If we did not look close and far, we would not know if a predator was ready to attack us. Today we tend to be captured by the screens. Arguably, all media content is designed to capture our attention such as data entry tasks required for employment, streaming videos for entertainment, reading and answering emails, playing e-games, responding to text notifications, looking at Instagram and Snapchat photos and Tiktok videos, scanning Tweets and using social media accounts such as Facebook. We are unaware of the symptoms of visual stress until we experience symptoms. To illustrate the physiological process that covertly occurs during convergence and accommodation, do the following exercise.
Sit comfortably and lift your right knee a few inches up so that the foot is an inch above the floor. Keep holding it in this position for a minute…. Now let go and relax your leg.
A minute might have seemed like a very long time and you may have started to feel some discomfort in the muscles of your hip. Most likely, you observed that when you held your knee up, you most likely held your breath and tightened your neck and back. Moreover, to do this for more than a few minutes would be very challenging.
Lift your knee up again and notice the automatic patterns that are happening in your body.
For muscles to regenerate they need momentary relaxation which allows blood flow and lymph flow to occur. By alternately tensing and relaxing muscles, they can work more easily for longer periods of time without experiencing fatigue and discomfort (e.g., we can hike for hours but can only lift our knee for a few minutes).
Solutions to relax the eyes and reduce eye strain
- Reestablish the healthy evolutionary pattern of alternately looking at far and near distances to reduce eyestrain, such as:
- Look out through a window at a distant tree for a moment after reading an email or clicking link.
- Look up and at the far distance each time you have finished reading a page or turn the page over.
- Rest and regenerate your eyes with palming. While sitting upright, place a pillow or other supports under our elbows so that your hands can cover your closed eyes without tensing the neck and shoulders.

- Cup the hands so that there is no pressure on your eyeballs, allow the base of the hands to touch the cheeks while the fingers are interlaced and resting your forehead.
- Close your eyes, imagine seeing black. Breathe slowly and diaphragmatically while feeling the warmth of the palm soothing the eyes. Feel your shoulders, head and eyes relaxing. Palm for 5 minutes while breathing at about six breaths per minute through your nose. Then stretch and go back to work.
Palming is one of the many practices that improves vision. For a comprehensive perspective and pragmatic exercises to reduce eye strain, maintain and improve vision, see the superb book by Meir Schneider, PhD., L.M.T., Vision for Life, Revised Edition: Ten Steps to Natural Eyesight Improvement.
Increased sympathetic arousal
Seeing the changing stimuli on the screen evokes visual attention and increases sympathetic arousal. In addition, many people automatically hold their breath when they see novel visual or hear auditory signals; since, they trigger a defense or orienting response. At the same time, without awareness, we may tighten our neck and shoulder muscles as we bring our nose literally to the screen. As we attend and concentrate to see what is on the screen, our blinking rate decreases significantly. From an evolutionary perspective, an unexpected movement in the periphery could be a snake, a predator, a friend or foe and the body responds by getting ready: freeze, fight or flight. We still react the same survival responses. Some of the physiological reactions that occur include:
- Breath holding or shallow breathing. These often occur the moment we receive a text notification, begin concentrating and respond to the messages, or start typing or mousing. Without awareness, we activate the freeze, flight and fight response. By breath holding or shallow breathing, we reduce or limit our body movements, effectively becoming a non-moving object that is more difficult to see by many animal predators. In addition, during breath holding, hearing become more acute because breathing noises are effectively reduced or eliminated.
- Inhibition of blinking. When we blink it is another movement signal that in earlier times could give away our position. In addition, the moment we blink we become temporarily blind and cannot see what the predator could be doing next.
- Increased neck, shoulder and back tension. The body is getting ready for a defensive fight or avoidance flight.
Experience some of these automatic physiological responses described above by doing the following two exercises.
Eye movement neck connection: While sitting up and looking at the screen, place your fingers on the back of the neck on either side of the cervical spine just below the junction where the spine meets the skull.
Feel the muscles of neck along the spine where they are attaching to the skull. Now quickly look to the extreme right and then to the extreme left with your eyes. Repeat looking back and forth with the eyes two or three times.
What did you observe? Most likely, when you looked to the extreme right, you could feel the right neck muscles slightly tightening and when you looked the extreme left, the left neck muscles slightly tightening. In addition, you may have held your breath when you looked back and forth.
Focus and neck connection: While sitting up and looking at the screen, place your fingers on the back of the neck as you did before. Now focus intently on the smallest size print or graphic details on the screen. Really focus and concentrate on it and look at all the details.
What did you observe? Most likely, when you focused on the text, you brought your head slightly forward and closer to the screen, felt your neck muscles tighten, and possibly held your breath or started to breathe shallowly.
As you concentrated, the automatic increase in arousal, along with the neck and shoulder tension and reduced blinking contributes to developing discomfort. This can become more pronounced after looking at screens to detailed figures, numerical data, characters and small images for hours (Peper, Harvey & Tylova, 2006; Peper & Harvey, 2008; Waderich et al, 2013).
Staying alert, scanning and reacting to the images on a computer screen or notifications from text messages, can become exhausting. in the past, we scanned the landscape, looking for information that will help us survive (predators, food sources, friend or foe) however today, we react to the changing visual stimuli on the screen. The computer display and notifications have become evolutionary traps since they evoke these previously adaptive response patterns that allowed us to survive.
The response patterns occur mostly without awareness until we experience discomfort. Fortunately, we can become aware of our body’s reactions with physiological monitoring which makes the invisible visible as shown in the figure below (Peper, Harvey & Faass, 2020).

Representative physiological patterns that occur when working at a computer, laptop, tablet or cellphone are unnecessary neck and shoulder tension, shallow rapid breathing, and an increase in heart rate during data entry. Even when the person is resting their hands on the keyboard, forearm muscle tension, breathing and heart rate increased.
Moreover, muscle tension in the neck and shoulder region also increased, even when those muscles were not needed for data entry task. Unfortunately, this unnecessary tension and shallow breathing contributes to exhaustion and discomfort (Peper, Harvey & Faass, 2020).
With biofeedback training, the person can learn to become aware and control these dysfunctional patterns and prevent discomfort (Peper & Gibney, 2006; Peper et, 2003). However, without access to biofeedback monitoring, assume that you respond similarly while working. Thus, to prevent discomfort and improve health and performance, implement the following.
- Practice breathing lower and slower to reduce sympathetic activation. Every few minutes remember to breathe slowly in and out through the nose. See the following blogs for more detailed instructions:
- Blink many times. Blink each time you click on a link, after typing a paragraph or after entering a few numbers.
- Get up, move, stretch and wiggle.
- Every few minutes do a small movement such as rotating your shoulders, dropping your hands to your lap.
- Every twenty minutes get up, stretch and walk around to reduce the chronic muscle tension.
- Install the free Stretch Break software on your computer or laptop to remind you to stretch… and then shows you how. Download free version from: https://stretchbreak.com/.
- Use small portable muscle biofeedback devices to learn awareness of the covert muscle tension and how to work without unnecessary muscle tension. For detailed training procedures see the free downloadable book by Erik Peper and Katherine Gibney, Muscle Biofeedback at the Computer- A Manual to Prevent Repetitive Strain Injury (RSI) by Taking the Guesswork out of Assessment, Monitoring and Training.
Finally, for a comprehensive overview based on an evolutionary perspective that explains why TechStress develops, why digital addiction occurs. and what can be done to prevent discomfort and improve health and performance, see our new book by Erik Peper, Richard Harvey and Nancy Faass, Tech Stress-How Technology is Hijack our Lives, Strategies for Coping and Pragmatic Ergonomics.

References
Peper, E. & Gibney, K. (2006). Muscle Biofeedback at the Computer- A Manual to Prevent Repetitive Strain Injury (RSI) by Taking the Guesswork out of Assessment, Monitoring and Training. The Biofeedback Federation of Europe. Download free PDF version of the book: http://bfe.org/helping-clients-who-are-working-from-home/
Schneider, M. (2016). Vision for Life, Revised Edition: Ten Steps to Natural Eyesight Improvement. Berkeley: North Atlantic Books. https://self-healing.org/shop/books/vision-for-life-2nd-ed
Turgut, B. (2018). Ocular Ergonomics for the Computer Vision Syndrome. Journal Eye and Vision, 1(2).